What is Endoscopic Brain Surgery?
How long do you have to stay in the hospital after brain surgery?
How long does it take to recover from brain surgery?
What is endoscopic brain surgery?
Are brain surgeries dangerous?
Do people recover from brain surgery?
What is the most common brain surgery?
What are the chances of surviving brain surgery?
What is Endoscopic Brain Surgery?
Endoscopic brain surgery is a procedure used primarily to treat brain tumors. It is considered a minimally invasive brain surgery that allows neurosurgeons to identify and treat conditions that are deep within the brain.
“This type of surgery allows us to treat brain tumors less invasively than traditional open brain surgery, while still affording us the ability to get an in-depth view of the brain.
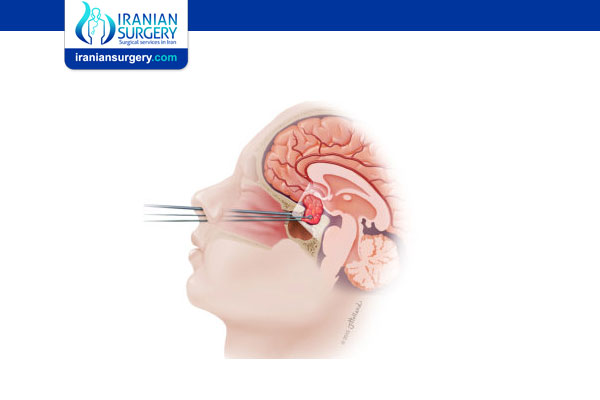
During this procedure, thin tubing that transmits video images of the brain is inserted through one or two small incisions in the skull or through an opening in the body. This tube-like instrument, called an endoscope, contains a small camera that allows the neurosurgeon to see detailed images of the problem area in the brain.
“Endoscopic approaches have truly transformed how we treat tumors, particularly because endoscopic techniques give us such a clear visualization of the tumor” .This approach also does not always require us to access the brain through the skull. We’re able to access the brain through pathways like the nose and sinuses as well.”
The neurosurgeon will use the images transmitted by the endoscope as a guide for removing the tumor or repair the affected area of the patient’s brain. The removal of the tumor or damaged area is performed with specialized surgical instruments. In minimally invasive endoscopic brain surgery we intend to reach pathology like a tumor through natural openings, like a nostril or small incisions with minimal or no brain retraction. An endoscope is inserted into this opening and used to visualize and perform the neurosurgical operation. The surgery is performed while looking at a monitor which displays magnified real-time video from the endoscope. The rest of the surgery is done with the similar techniques as to open surgery, but requires the use of special instruments and allows for less retraction and chance of injury to the brain. The same principles are used for operations of the spine.
Read more about Do arachnoid cysts require surgery?
Read more about Ovarian cyst size chart
Read more about Breast reduction size chart
Read more about Stages of fissure healing
Read more about Endoscopic Brain Surgery
Read more about What we can do for you in Iranian surgery?
Who is a candidate?
This new, endoscopic surgical technique is most commonly used in patients with benign lesions such as pituitary adenomas. However, surgeons are starting to use it to remove other selected brain tumors as well. Some of the types of lesions that may be treated with this new approach include:
- Pituitary tumors
- Meningiomas (tumors arising from the lining of the brain)
- Craniopharyngiomas (a type of tumor derived from pituitary gland tissue)
- Rathke's cleft cysts (benign cystic lesions that affect mainly the pituitary gland)
- Chordomas (rare, slow-growing malignant tumors at the base of the skull)
- Spinal fluid leaks/rhinorrhea
Read more about: Brain cancer treatment Iran
What is its done?
The goal of surgery depends on what the procedure is for. This may be to remove a tumor, biopsy a mass, decompress a cranial nerve, remove a herniated disc, or treat any number of neurosurgical problems.
What happens before surgery?
You will have an office visit with a neurosurgeon, ENT surgeon, and endocrinologist before surgery. A consult with an ophthalmologist may be necessary if you have vision problems. During the office visit, the surgeon will explain the procedure, its risks and benefits, and answer any questions. Next, you will sign consent forms and complete paperwork to inform the surgeon about your medical history (i.e., allergies, medicines, bleeding history, anesthesia reactions, previous surgeries). Discuss all medications (prescription, over-the-counter, and herbal supplements) you are taking with your health care provider. Some medications need to be continued or stopped the day of surgery. You may be scheduled for presurgical tests (e.g., blood test, electrocardiogram, chest X-ray, and CT scan) several days before surgery.
Stop taking all non-steroidal anti-inflammatory medicines (Naprosyn, Advil, Motrin, Nuprin, Aleve) and blood thinners (coumadin, Plavix, aspirin) 1 week before surgery. Additionally, stop smoking and chewing tobacco 1 week before and 2 weeks after surgery as these activities can cause bleeding problems. No food or drink is permitted past midnight the night before surgery.
Read more about Cancer treatment in Iran
Read more about Side effects of having only one testicle
Read more about Rectal bleeding
Read more about Laser Eye Surgery in Iran
Read more about: Spinal stenosis treatment
The day of surgery
- Shower using antibacterial soap. Dress in freshly washed, loose-fitting clothing.
- Wear flat-heeled shoes with closed backs.
- If you have instructions to take regular medication the morning of surgery, do so with small sips of water.
- Remove make-up, hairpins, contacts, body piercings, nail polish, etc.
- Leave all valuables and jewelry at home (including wedding bands).
- Bring a list of medications (prescriptions, over-the-counter, and herbal supplements) with dosages and the times of day usually taken.
- Bring a list of allergies to medication or foods.
Read more about: Spinal Tumor surgery
What happens after surgery?
After surgery you will be taken to the recovery room, where vital signs are monitored as you awake from anesthesia. Then you'll be transferred to a regular room or the intensive care unit (ICU) for observation and monitoring. You will be encouraged to get out of bed as soon as you are able (sitting in a chair, walking).
After surgery you may experience nasal congestion, nausea, and headache. Medication can control these symptoms. An MRI of the brain will be obtained the day after surgery. In 1 to 2 days, you'll be released from the hospital and given discharge instructions.
How long do you have to stay in the hospital after brain surgery?
You might stay in hospital for around 3 to 10 days after surgery. How long you stay in hospital depends on your operation and how long you take to recover. As soon as it is safe, you will be allowed to go home where you continue to recover.
How long does it take to recover from brain surgery?
It can take 4 to 8 weeks to recover from surgery. Your cuts (incisions) may be sore for about 5 days after surgery. Swelling in the brain is expected after surgery, so recovery will take time and the benefits will not be immediately apparent. Returning headaches should also be reported to the care team, as it may be a sign of a recurrent edema (swelling in the brain) or a new tumor.
Your Recovery
You will probably feel very tired for several weeks after surgery. You may also have headaches or problems concentrating. It can take 4 to 8 weeks to recover from surgery. Your cuts (incisions) may be sore for about 5 days after surgery.
What Risks are associated with Endoscopic Brain Surgery?
With any surgery, there are risks involved. Rebound surgeons educate their patients on the best treatment options for their particular condition and communicate the potential risks.
Possible risks:
- Temporary or permanent interference with sensory and motor functions like speech, vision, memory, balance, coordination, etc.
- Blood clot
- Bleeding
- Swelling
- Infection
- Seizure
- Stroke
- Coma
What is endoscopic brain surgery?
Endoscopic brain surgery is a procedure used primarily to treat brain tumors. It is considered a minimally invasive brain surgery that allows neurosurgeons to identify and treat conditions that are deep within the brain.
Read more about: craniotomy surgery
Are brain surgeries dangerous?
As with any brain surgery, awake brain surgery has the potential for risks and complications. These include:
- allergic reaction to anesthesia
- bleeding in the brain
- a blood clot
- brain swelling
- coma
- impaired speech, vision, coordination, or balance
- infection in the brain or at the wound site
- memory problems
- seizures
- stroke
Do people recover from brain surgery?
Most people wake up a few hours after their brain surgery. But sometimes, your surgeon might decide to keep you asleep for a few days after surgery, to help you recover. They use sedatives to keep you asleep. While you are asleep, you might be breathing through a machine called ventilator. Some people recover well after brain surgery, but this can take some time. Other people have some problems, or long-term difficulties. The problems you may have depends on the area of the brain where the tumour was (or still is if you only had part of the tumour removed.
Read more about: Cranioplasty surgery after stroke
What is the most common brain surgery?
Surgery is one type of treatment for brain tumors. The most common types of surgery performed for brain tumors are:
- Biopsy
- Craniotomy
- Extended bifrontal craniotomy
- "Eyebrow" craniotomy (supra-orbital craniotomy)
- "Keyhole" craniotomy (retro-sigmoid craniotomy)
- Orbitozygomatic craniotomy
- Translabyrinthine craniotomy
- MRI-guided laser ablation
- Endonasal endoscopy (endonasal endoscopic surgery)
- Neuroendoscopy
What are the chances of surviving brain surgery?
Based on information collected from 2000 to 2004, for people diagnosed with a primary malignant brain and spinal cord tumor (including lymphoma and leukemia, tumors of the pituitary and pineal glands, and tumors of the nose), the five-year survival rates are 28.8 percent for males and 31.6 percent for females. The 5-year survival rate for people younger than age 15 is more than 74%. For people age 15 to 39, the 5-year survival rate is about 71%. The 5-year survival rate for people age 40 and over is about 21%. However, survival rates vary widely and depend on several factors, including the type of brain or spinal cord tumor.
Read more about: Cranioplasty surgery recovery
10 common questions about Endoscopic Brain Surgery
[kkstarratings]