ICSI procedure step by step

ICSI Procedure Step by Step
Steps of ICSI Treatment – Guide of ICSI Treatment
Intracytoplasmic sperm injection (ICSI) is performed as part of your in vitro fertilization (IVF) procedure. It is a process in which an embryologist injects a single sperm into the cytoplasm (centre) of each egg. After the embryologist fertilizes the egg with the sperm, he or she will observe the egg over the next day or so. If fertilization occurs and the embryo matures properly, a doctor can transfer it into your uterus. Your doctor may recommend ICSI as part of your IVF procedure to treat many causes of infertility, especially when there is a problem with the sperm, such as low motility (movement) or a low sperm count. ICSI is especially useful in cases where the sperm cannot penetrate the egg or if the sperm is abnormally shaped. This treatment has been revolutionary in treating male factor infertility cases.
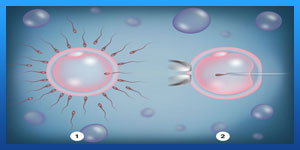
Read more about : Ivf process start to finish step by step
ICSI Procedure Step by Step
Here is a detailed description of the ICSI procedure step by step to give you a better idea of what exactly happens-
. Step one: Stimulation of the ovaries
In the stimulation phase of an ICSI cycle, you will use injectable medications for approximately 8 to 14 days to stimulate the ovaries to produce eggs. Follicle-stimulating hormone (FSH) and luteinizing hormone (LH), both produced naturally within the body, comprise the medications. During this phase, you will come into the clinic approximately 7 to 8 times for morning monitoring, which allows the team to track the progress of your cycle and adjust medication dosages as needed.
The trigger injection is the final step in the stimulation phase of treatment. Depending on your individual protocol, you will either have a human chorionic gonadotropin (HCG) or a buserelin trigger. This injection helps the developing eggs complete the maturation process and sets ovulation in motion. Timing is very important here, as the doctor must perform the egg retrieval prior to the expected time of ovulation.
Read more about : How many days after period is frozen embryo transfer?
. Step two: Egg retrieval
On the morning of your egg retrieval, a doctor will meet with you before the procedure to review your protocol. You will also meet with an anesthetist, who will review your medical history and will administer the intravenous fluid you will receive prior to the start of the procedure to induce sleep.
Obtaining the sperm: If you are using a fresh sperm sample, a member of the embryology team will come to accept the sample. If you are using a frozen sperm sample or donor sperm collected previously, the embryologist will verify those details with you. Our andrology laboratory will wash and prepare the sperm, so that the healthiest sperm are brought together with the eggs for fertilization (after the doctor performs the egg retrieval).
Obtaining the eggs: The egg retrieval itself takes about 20 to 30 minutes. During the procedure, the doctor will guide a needle into each ovary to remove the egg-containing fluid in each follicle. The doctor utilises an ultrasound during the procedure to see where to guide the needle. Recovery will take about 30 minutes and you will be able to walk out on your own. It's important that a responsible adult drive you home after the procedure, as it is unsafe to drive after receiving anaesthesia. The person who is driving you will not need to stay at our clinic during your procedure—he or she should anticipate coming back to the clinic after approximately 3 hours.
Read more about: Can you have twins with ICSI?
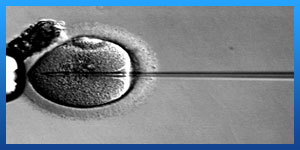
. Step three: Fertilisation
After the egg retrieval, the embryologist will prepare the eggs and sperm. For PGD the embryologist will inject one single sperm into each mature egg under a microscope. PGD is therefore possible with very few sperm.
. Step four: Embryo development
Embryo development begins after fertilization. After initial fertilisation the embryos will be placed within our Embryoscopes which enables them to continue to develop completely undisturbed. An embryologist examines each developing embryo over the course of the following 5 to 6 days. The goal is to see progressive development, with a two- to four-cell embryo on day 2 and a six- to eight-cell embryo on day 3. After the eight-cell stage, rapid cell division continues and the embryo enters into what is called the blastocyst stage at day 5 or 6. It is your doctor’s goal to transfer the highest-quality embryo(s) to give you the greatest chance of success.
Read more about : Ivf process start to finish
. Step five: Embryo transfer
The embryo transfer is a simple procedure that only takes about 5 minutes to complete. There is no anaesthesia or recovery time needed. When your nurse arranges your transfer, she will notify you and provide instructions on when to arrive and how to prepare. You need to have a full bladder for the procedure as a full bladder ensures good visualization of the lining of the uterus and proper placement of the embryos. It's important to drink the specific amount of liquid recommended 30 to 40 minutes ahead of time.
You will review your cycle with the doctor and the number of embryos recommended for transfer. Upon entering your procedure room, the embryologist will again confirm your last name and the number of embryos for transfer. The embryologist will load the transfer catheter in the embryology lab with the embryo(s) and then the doctor will insert the catheter into the uterus and push the embryo through with a small amount of fluid.
An external abdominal ultrasound provides visual guidance via a monitor to the doctor throughout the procedure. Once the doctor transfers the embryo, he or she will slowly remove the catheter. Since the embryo is invisible to the naked eye, the embryologist will then examine the catheter under a microscope in the lab to ensure that the catheter did indeed release the embryo. The nurse will give you instructions for the following 2 weeks until it's time for the pregnancy test.
. Step six: The pregnancy test
Two weeks after the embryo transfer, you will perform a pregnancy test. This test is frequently called a "beta" because it measures the beta chain portion of the HCG hormone emitted by the developing embryo. We let you do this test in the privacy of your own home using a urinary pregnancy test and you then let us know the outcome so we can plan the next steps.
Read more about : Can i bend down after embryo transfer?


1 Comment
Hi,
Wow, a Very Nice blog post! Your site has given the best information From Your Articles. They are amazing and Useful to all people. Thank you for sharing this post and Impressive site. The IVF advanced is one of the most excellent centers in Asia Pacific, with Techniques, genuine Treatment, Research & Training. The IVF advanced is the leading Test Tube Centre in the country with modern world-class scientific technologies.