Craniotomy Surgery
What is Craniotomy Surgery?
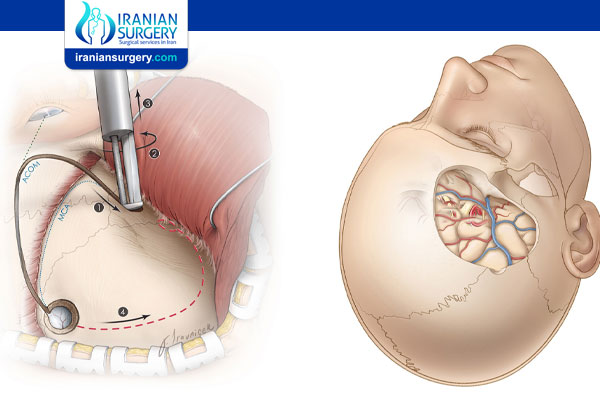
A craniotomy is type of brain surgery. It involves removing part of the skull, or cranium, to access the brain. The bone is replaced when the surgery is done.
In general, a craniotomy is done to remove brain tumors and treat aneurysms.
A neurosurgeon performs the procedure. In this article, we’ll explore the types of craniotomies, along with the possible risks and recovery process.
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Surgeons in Iran. The price of Craniotomy Surgery in Iran can vary according to each individual’s case and will be determined based on an in-person assessment with the doctor.
For more information about the cost of Craniotomy Surgery in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number +98 901 929 0946. This service is completely free.
Before Craniotomy Surgery
Reasons for a craniotomy
A craniotomy is done to treat the following conditions of the brain:
. Tumor
. Aneurysm
. Infection
. Swelling (cerebral edema)
. Bleeding inside the skull
. Blood clot
. Brain abscess
. Skull fracture
. Dura mater tear
. Arteriovenous malformation
. Arteriovenous fistula
. Intracranial pressure
. Epilepsy
The procedure is also used to implant devices for movement disorders, like Parkinson’s disease.
Craniotomy risks, side effects, and complications
Your risk of complications depends on many factors, including your specific brain surgery and medical condition.
Possible complications include:
. Head scarring
. Dent where bone flap was removed
. Injury from the head device
. Facial nerve damage
. Damage to the sinuses
. Infection of the bone flap or skin
. Seizures
. Brain swelling
. Leaking of cerebrospinal fluid
. Muscle weakness
. Stroke
Rarely, a craniotomy may lead to:
. Speech problems
. Memory problems
. Balance issues
. Paralysis
. Coma
A craniotomy can also cause general surgical side effects like:
. Bleeding
. Blood clots
. Pneumonia
. Reaction to general anesthesia
. Unstable blood pressure
If you’re worried about these complications, talk to your surgeon.
Before the procedure
To prepare for the surgery, you’ll have one or more preoperative appointments with your neurosurgeon.
They’ll use various tests to confirm you can safely undergo the procedure. This will likely include:
. Physical exam
. Blood tests
. Neurological exam
. Imaging of the brain (CT or MRI)
Your surgeon will also determine the surgical site based on your medical condition and type of craniotomy.
On the night before your surgery, you’ll fast (not eat) after midnight. You might also need to wash your hair with antiseptic shampoo.
Depending on your condition, your surgeon may have you take other steps to prepare.
During Craniotomy Surgery
Types of craniotomy
There are many types of craniotomies. Each type is named for the technique or location used in the surgery.
. Stereotactic craniotomy
If a craniotomy uses an MRI or CT scan, it’s called a stereotactic craniotomy.
In this procedure, your surgeon uses imaging tests to create three-dimensional images of your brain. It allows them to distinguish between healthy and abnormal tissue.
Stereotactic techniques also help your surgeon find the best spot for a scalp incision. This makes it easier to make smaller cuts and perform minimally invasive procedures.
. Endoscopic craniotomy
In an endoscopic craniotomy, your surgeon makes a tiny incision in your skull. They insert an endoscope, which is a small lighted device with a camera. This technique is often used with keyhole craniotomies.
. Awake craniotomy
An awake craniotomy is done while you’re awake. During the surgery, your surgeons ask you questions while monitoring your brain activity.
As you reply, they’ll indicate what parts of the brain are involved in speech, movement, and vision. This helps them avoid these areas while performing the surgery.
. Keyhole craniotomy
A keyhole craniotomy is used to remove brain tumors. It’s a minimally invasive surgery that’s associated with less scarring and a shorter recovery time.
Your surgeon makes a small cut behind your ear. They remove the brain tumor through this incision.
. Supra-orbital ‘eyebrow’ craniotomy
A supra-orbital “eyebrow” craniotomy is done to remove brain tumors in the front of your brain.
Your surgeon makes a small cut in your eyebrow. It’s a minimally invasive approach that causes minimal scarring.
. Pteronial (frontotemporal) craniotomy
In the skull, the pterion is where the frontal, temporal, sphenoid, and parietal bones meet. It’s found on the side of your skull near your temple.
A pteronial craniotomy, or frontotemporal craniotomy, involves removing part of the pterion. Your surgeon makes an incision behind your hairline, letting them access numerous parts of the brain.
. Orbitozygomatic craniotomy
Difficult tumors and aneurysms may be treated with an orbitozygomatic craniotomy.
It involves a small scalp incision behind your hairline. Your surgeon temporarily removes part of the bone that creates the curve of your orbit, or eye socket, and cheek.
This lets your surgeon reach deeper regions of your brain while reducing the risk of brain damage.
. Posterior fossa craniotomy
The posterior fossa is the lower part of the skull. It’s near the brainstem and cerebellum, which controls balance and coordination.
If there’s a tumor in the posterior fossa, it can place pressure on the cerebellum, brainstem, and spinal cord.
A posterior fossa craniotomy can remove the tumor and alleviate this pressure. This is done through an incision at the base of your skull.
. Translabyrinthine craniotomy
In a translabyrinthine craniotomy, your surgeon makes a cut behind your ear. They remove part of the mastoid bone and the semicircular canals, which help you balance.
It’s used to remove an acoustic neuroma, also called a vestibular schwannoma. An acoustic neuroma is a noncancerous tumor that forms on the nerve that connects your inner ear and brain. It causes hearing loss and balance issues.
Removing the semicircular canals results in hearing loss. However, the surgery decreases the risk of facial nerve damage.
. Bifrontal craniotomy
A bifrontal craniotomy, or extended bifrontal craniotomy, is done to remove difficult tumors in front of the brain. It’s often used if the tumor is too complex for minimally invasive surgery.
Your surgeon makes a cut behind your front hairline. They remove a piece of the bone that forms the curve of your forehead, letting them access the front of your brain.
During the procedure
When you arrive for the surgery, you’ll remove all of your clothing and jewelry. You’ll wear a hospital gown.
You’ll sit or lie down on the operating table. The position depends on the part of your brain being operated on. A head device will hold your head in place.
Next, your healthcare team will:
. Insert an intravenous line into your arm or hand
. Insert a urinary catheter into your bladder
. Give you general anesthesia
Once the anesthesia makes you fall asleep, your surgeon will shave the hair on the surgical site. They’ll also clean the area to reduce the risk of infection.
Your surgeon will make an incision on your scalp. They’ll use a medical drill and saw to remove a piece of bone called a bone flap.
Next, your surgeon will cut the dura mater to access the brain. The dura mater is the brain’s outermost membrane.
Your surgeon will perform the procedure and remove tissue samples, if necessary.
When the procedure is done, they’ll stitch the tissue back together. They’ll replace the bone flap with wires, stitches, or plates.
Finally, your surgeon will stitch or staple the skin incision, then apply a sterile bandage.
The procedure can take approximately 2 1/2 hours.
After Craniotomy Surgery
Recovery following craniotomy
Recovery depends on the type of surgery. Here’s what it usually looks like:
Immediately after surgery
You’ll be taken to the recovery unit or intensive care unit when the procedure is complete. Nurses will monitor your vitals as you wake up.
You’ll be taken to your hospital room once your vitals are stable. You can expect to stay at the hospital for about 1 week.
During your stay, your healthcare providers will likely:
. Elevate your head to manage swelling
. Give you oxygen for several days
. Teach you deep-breathing exercises to prevent pneumonia
. Place compression devices on your legs to prevent blood clots
The urinary catheter will stay in your bladder for several days.
Your healthcare team will frequently do neurological checkups to ensure your brain and body are functioning properly.
Before you go home, your surgeon will provide home care instructions.
At home
After a craniotomy, follow your doctor’s orders for bathing and incision care. Take your prescription medication as directed.
You can expect to be out of work for at least 6 weeks.
During this time, you might have issues with:
. Walking
. Talking
. Strength
. Balance
To regain these functions, you may need physiotherapy, occupational therapy, or speech therapy. You’ll also need to get lots of rest.
Attend your follow-up appointments so your doctor can see how you’re healing. They’ll let you know when you can resume certain activities.
Life after craniotomy
After you’ve fully recovered, it’s still important to take care of yourself. This will help manage future complications and improve your long-term outlook.
Continue seeing your doctor for follow-up appointments. It’s also wise to:
. Exercise regularly
. Eat a healthy diet
. Limit or avoid alcohol
. Quit smoking (this can be a difficult, but a doctor can help create a plan that works for you)
. Get enough sleep
Source:
10 common questions about craniotomy surgery in Iran
[kkstarratings]