Cancer treatment in Iran
If you decide to have a Cancer treatment in Iran, reading this article can improve your knowledge to a great extent and help you to choose the best city and hospital to treat your Cancer in Iran.
________________________________________________________________________________________
Plan your Cancer treatment in Iran with the Best oncologist surgeon.
Iranian Surgery is a medical tourism company in Iran that cooperates with the best oncologist surgeons, specialists and Hospital in Iran and offers world-class treatments at an affordable cost.
_________________________________________________________________________________________

Read more about : Cancer treatment success story in Iran
Read more about : Leg lengthening surgery success story in Iran
Read more about : Metastatic myxofibrosarcoma treatment with the best Iranian oncologist surgeon
What is Cancer Treatment?
Cancer treatment is the use of surgery, radiation, medications and other therapies to cure a cancer, shrink a cancer or stop the progression of a cancer.
Why it's done
The goal of cancer treatment is to achieve a cure for your cancer, allowing you to live a normal life span. This may or may not be possible, depending on your specific situation. If a cure isn't possible, your treatments may be used to shrink your cancer or slow the growth of your cancer to allow you to live symptom free for as long as possible.
Read more about : Colorectal cancer surgery
Read more about : Anal Cancer Treatment
Read more about : Bone cancer stage
Cancer treatments may be used as:
. Primary treatment. The goal of a primary treatment is to completely remove the cancer from your body or kill all the cancer cells.
Any cancer treatment can be used as a primary treatment, but the most common primary cancer treatment for the most common types of cancer is surgery. If your cancer is particularly sensitive to radiation therapy or chemotherapy, you may receive one of those therapies as your primary treatment.
. Adjuvant treatment. The goal of adjuvant therapy is to kill any cancer cells that may remain after primary treatment in order to reduce the chance that the cancer will recur.
Any cancer treatment can be used as an adjuvant therapy. Common adjuvant therapies include chemotherapy, radiation therapy and hormone therapy.
Neoadjuvant therapy is similar, but treatments are used before the primary treatment in order to make the primary treatment easier or more effective.
. Palliative treatment. Palliative treatments may help relieve side effects of treatment or signs and symptoms caused by cancer itself. Surgery, radiation, chemotherapy and hormone therapy can all be used to relieve symptoms. Other medications may relieve symptoms such as pain and shortness of breath.
Palliative treatment can be used at the same time as other treatments intended to cure your cancer.
Types of Cancer Treatment
There are many types of cancer treatment. The types of treatment that you receive will depend on the type of cancer you have and how advanced it is.
Some people with cancer will have only one treatment. But most people have a combination of treatments, such as surgery with chemotherapy and/or radiation therapy.
Many cancer treatments are available. Your treatment options will also depend on your general health, and your preferences. Together you and your doctor can weigh the benefits and risks of each cancer treatment to determine which is best for you.
Read more about : Brain Cancer Treatment
Read more about : Oral Cancer Treatment
Cancer treatment options include:
- Surgery. The goal of surgery is to remove the cancer or as much of the cancer as possible.
What is surgery?
Surgery is one of the main treatments for many cancers and involves cutting body tissue. The type of surgery you have will depend on the type of cancer you have. The preparation, side effects and possible complications will also depend on the type of surgery you have.
 Why am I having surgery?
Why am I having surgery?
There are different reasons why your cancer doctor may suggest you have surgery.
You may have surgery for one of the following reasons:
. Surgery to diagnose cancer
. Surgery to treat cancer
. Surgery to find out the stage of the cancer
. Reconstruction surgery
. Surgery to control the symptoms of cancer
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Surgeons and hospital to treat your cancer in Iran. The price of treating a cancer in Iran can vary according to each individual’s case and will be determined by the type of cancer you have and an in-person assessment with the doctor. So if you are looking for the cost of cancer treatment in Iran, you can contact us and get free consultation from Iranian surgery.
Can surgery cure the cancer?
Many cancers can be cured with surgery. However, it is not always possible to know at the time of the surgery whether any cancer cells have broken away and spread to tissues around the main tumor. To try and make sure all the cancer cells are removed, the surgeon will remove the tumor and surrounding area (margin) of normal tissue. A pathologist will examine this tissue and check the margin to see if it is clear of cancer cells.
Removing all the cancer cells helps reduce the risk of the cancer coming back. If the margin of tissue is not clear, your cancer specialist may suggest you have a further operation to take more tissue from the surrounding area.
For some people, there is a risk that cancer cells may have spread from the main tumor to another part of the body. These are known as micrometastases. Micrometastases are too small to be seen on scans. If there is a risk of micrometastases, your cancer specialists may recommend that you have other treatments, such as chemotherapy and radiotherapy as part of your treatment.
Occasionally, scans taken before surgery do not show the true extent of the cancer. During the operation, the surgeon may find that it is not possible to remove the cancer completely. If this is the case, your cancer specialists will discuss with you the best treatment possible for your situation.
Read more about : What are the signs of a transplanted kidney being rejected?
Read more about : Heart transplant in Iran
Types of surgery
There are different types of surgery that can be used to treat cancer.
Open surgery
Open surgery means the surgeon makes one large cut (incision).
Keyhole surgery
Some people may be able to have keyhole surgery (sometimes called laparoscopic surgery) to remove some or all of a tumor.
In this type of surgery, several small cuts are made instead of one large cut (incision). The surgeon uses a laparoscope to work inside the body and remove the tumor through a small cut in the skin.
The main advantage of keyhole surgery is that it leaves a much smaller wound in the chest or tummy wall. This means that recovery time is shorter. Sometimes people who are not fit enough to have an open operation may be able to have keyhole surgery.
The results from keyhole surgery can be as good as conventional surgery. However, it needs to be done by surgeons with specialist training and experience in using laparoscopic techniques. If it is suitable for you and you choose to have this type of surgery, you may need to travel to another
hospital to have it.
 Preparing for an operation
Preparing for an operation
Before any operation, you will be asked not to eat or drink anything for a few hours. This is known as being ’nil-by-mouth’.
You may also need to bathe and shave body hair from the area of the operation. The nurse looking after you will give you more details about this. Body hair is only shaved if it is essential. It is done using a disposable razor and the hair will begin to grow back after the operation.
Having an operation can put you at risk of getting a blood clot in the leg. Compression stockings (also known as anti-embolic stockings) help to reduce this risk. Your doctors and nurses may ask you to wear a pair of compression stockings during your operation and for a short time afterwards. A nurse will assess your individual risk and take your measurements. They will show you how to put the stockings on properly.
Read more about : Bladder Cancer treatment
Read more about : What is Bladder Cancer?
After surgery
Waking up after surgery
Knowing what will happen when you wake up after your operation can help you feel less anxious.
You will probably feel quite drowsy and may not remember much about the first few hours after you wake up.
A nurse will take your blood pressure regularly. Depending on the operation, you may have some tubes attached to you. If the operation was small, you may not have any tubes at all. Below is a list of the most common tubes you might have following an operation:
. A drip (intravenous infusion) into a vein in your arm or hand to give you fluids until you can eat and drink normally. This may be for a few hours or a few days, depending on the operation you have had.
. A tube (drain) in your wound to drain excess fluid into a small bottle. This is usually removed after a few days.
. A small tube (catheter) may be put into your bladder so that urine is drained into a collection bag. The catheter is usually removed when you start walking.
You can read about what to expect in the surgery section of the type of cancer you have.
After surgery you may experience:
. Pain
. Feeling sick (nausea) and being sick (vomiting)
Complications of surgery
Complications will depend on the type of operation you have. The most common complications after surgery are a wound infection, bleeding from the wound, a chest infection or developing a blood clot. The nurses will monitor you for these. Let them know straight away if you have any bleeding, feel unwell, have symptoms of an infection, such as a cough or discharge from your wound, or swelling and redness in a limb.
. Wound care
The wound is closed using clips or stitches. These are usually removed after you go home by a practice nurse at your GP surgery. Some surgeons use dissolving stitches that do not need to be removed. These will dissolve completely when the area is healed. You may be given antibiotics to help prevent wound infection. It is important to let your nurse or doctor know straight away if your wound becomes hot, painful or begins to bleed or leak any fluids, even after you go home.
. Scarring
Your scar may feel itchy at first. It will look like a red line, which may feel a bit lumpy. This will gradually fade over time.
Read more about : Orchiectomy surgery for prostate cancer
Read more about : Prostate Cancer Treatment
Possible long-term effects of surgery
Some people may have long-term effects after cancer surgery. Before your operation, your surgeon or specialist nurse will explain these to you and the risk of them happening.
Some examples of long term effects are listed below:
. Lymphoedema
. Infertility
. Erectile dysfunction
- Chemotherapy. Chemotherapy uses drugs to kill cancer cells.
 What is chemotherapy?
What is chemotherapy?
Chemotherapy uses anti-cancer (cytotoxic) drugs to destroy cancer cells. Cytotoxic means toxic to cells. Cytotoxic chemotherapy drugs disrupt the way cancer cells grow and divide.
Most chemotherapy drugs are carried in the blood. This means they can reach cancer cells anywhere in the body.
Chemotherapy drugs also affect some of the healthy cells in your body. These healthy cells can usually recover from damage caused by chemotherapy. But cancer cells cannot recover, and they eventually die.
Because chemotherapy drugs can affect some of the healthy cells in your body, this can cause side effects. Most side effects will go away after treatment finishes.
Read more about : Pancreatic cancer
Read more about : Prostate Cancer Treatments Pros and Cons
Why am I having chemotherapy?
Having chemotherapy depends on different factors. These include the type of cancer, the risk of it coming back, if it has spread and your general health.
You may have chemotherapy for one of the following reasons:
. As a main treatment for cancer
. To shrink a cancer before surgery or radiotherapy (neo-adjuvant chemotherapy)
. To reduce the risk of cancer coming back after surgery or radiotherapy (adjuvant chemotherapy.
. To make radiotherapy work better (chemoradiation)
. To treat locally advanced or advanced cancer (palliative chemotherapy)
Read more about : Ovarian Cancer Treatment
Which chemotherapy drug will I have?
Not all cancers are treated with the same chemotherapy drugs. Different drugs affect the cancer cells in different ways. The drugs you are given and the way they are given will depend on the type of cancer you have.
You may have one chemotherapy drug or a combination of different drugs. When a combination of drugs is used, each drug is chosen for its different effects.
There are many different chemotherapy drugs and new drugs are being developed all the time. You may be invited to take part in a research trial.
Other anti-cancer drugs are used to treat cancer, but they are not usually known as chemotherapy. For example, drugs called targeted therapies work differently to chemotherapy. These drugs can be given on their own or in combination with chemotherapy drugs.
Chemotherapy cycles
Chemotherapy is usually given as several sessions of treatment, with rest periods in between the sessions. The rest period allows your body to recover from the side effects. It also allows the number of healthy cells in your blood to go back to normal.
Chemotherapy and the rest period make up a cycle of your treatment. Your cancer doctor will explain the number of cycles you need to treat the cancer.
After your first cycle, you will have a better idea of what to expect, and how much you may or may not be able to do during your treatment.
Continuous or daily chemotherapy
Chemotherapy is sometimes given continuously by an infusion pump for several days or several weeks. If you are having chemotherapy as tablets or capsules, you may have them daily for several weeks or months before a rest period.
Read more about : Cancer Treatment
Read more about : Orchiectomy surgery for prostate cancer
Tests and scans
Your cancer doctor or specialist nurse will talk to you about any tests, scans or check-ups you need before chemotherapy begins.
. Scans and x-rays
. Height and weight
. Blood tests
. Pregnancy test
Effects on your body
The most common reason for delaying chemotherapy is a low number of white blood cells (neutrophils). This is not unusual. When your white blood cells are back to a healthy level, you can start your next cycle of chemotherapy.
Chemotherapy can also affect organs, such as the bone marrow, lungs, kidneys and liver. You will have regular tests to monitor this. Some drugs can affect the nerves in your feet and hands (known as peripheral neuropathy) and other drugs may affect your hearing.
Sometimes your doctor may need to reduce the dose of the drug or change your chemotherapy drug to a different one.
Read more about : Can you get a second kidney transplant?
Side effects of chemotherapy
Chemotherapy treatment can cause different side effects. These will depend on the chemotherapy drugs you are having. Some side effects are more common than others, but you will not have them all.
Healthy cells in certain parts of the body are more sensitive to chemotherapy drugs. This includes cells in the bone marrow, which makes blood cells, and the digestive system.
This is why certain side effects are more common, such as being at risk of infection or feeling sick.
Late effects of chemotherapy
Some people may have late effects from chemotherapy. These are side affects you still have 6 months after chemotherapy, or side effects that begin years later. Late effects are not common, and any risk is outweighed by the benefits of chemotherapy.
After chemotherapy
After your treatment has finished, you will have regular check-ups and possibly scans or x-rays. This will depend on the type of cancer and the treatments you have had.
Follow-up appointments are a good opportunity to discuss any problems or worries you have. It may help to make a list of questions beforehand so you do not forget anything important.
Recovery after chemotherapy
You may have mixed emotions when you get to the end of your chemotherapy treatment. You will probably feel relieved, but you may also feel anxious and uncertain.
You may feel ready to get on with your life after chemotherapy, but sometimes you may feel less positive.
It is important to accept that it will take you time to recover and you may feel tired for a while. You may also have new challenges to cope with, such as physical effects caused by the cancer or its treatment. It usually takes time to adjust to these and find out what is now normal for you. Complementary therapies may help you feel better and reduce any stress and anxiety.
When your treatment is over, you may want to think about making some positive changes to your lifestyle. Many people find that over time they settle back into their usual routines. But it is important to remember that support is available to help you with any physical or emotional problems you have.
- Radiation therapy. Radiation therapy uses high-powered energy beams, such as X-rays or protons, to kill cancer cells. Radiation treatment can come from a machine outside your body (external beam radiation), or it can be placed inside your body (brachytherapy).
What is radiotherapy?
Radiotherapy uses high-energy rays, such as x-rays, to treat cancer. It destroys cancer cells in the area where it is given.
Some normal cells in the area can also be damaged by radiotherapy. This can cause side effects. These normal cells can usually repair themselves, but cancer cells cannot. As the normal cells recover, the side effects usually get better.
Radiotherapy is always carefully planned by a team of experts and is continuing to become even more accurate. This means it can be used to treat the cancer more effectively, while doing as little harm as possible to normal cells.
Chemoradiation
Some people may have chemotherapy at the same time as radiotherapy. This is called chemoradiation or chemoradiotherapy. Chemotherapy uses anti-cancer (cytotoxic) drugs to destroy cancer cells. The chemotherapy drugs can make cancer cells more sensitive to radiotherapy. This can help the radiotherapy work well. This is only helpful for certain types of cancer, so it is not suitable for everyone.
Having chemotherapy and radiotherapy together can make the side effects of treatment worse. Your doctor, radiographer or specialist nurse can give you more information about chemoradiation and the possible side effects.
Read more about : Breast Implant Surgery
Why am I having radiotherapy?
You may have radiotherapy for different reasons:
. Radiotherapy to destroy a tumor and cure the cancer (sometimes called radical treatment).
. Radiotherapy to treat symptoms (palliative radiotherapy)
Before you have radiotherapy
Before you start your treatment, it needs to be planned carefully by your radiotherapy team. This is to make sure the radiotherapy is aimed precisely at the cancer, causing as little damage as possible to surrounding tissue.
Your team will explain what the treatment involves and will ask you to sign a consent form. This gives your team permission to give you treatment.
There are some things you should consider before having radiotherapy:
. Avoiding pregnancy or making someone pregnant
. Tell your doctor if you have a pacemaker, implantable cardiac device (ICD) or cochlea implant.
. Skin care
. Arranging help at home and getting to appointments
. Stopping smoking
Read more about : open heart surgery in Iran
Read more about : Stages of fissure healing
Read more about : Rectal abscess burst
Side effects of radiotherapy
Your team plans your treatment carefully to reduce your risk of side effects. However, most people have a few side effects during or after radiotherapy.
The side affects you have will depend on:
. The area of your body being treated - you may find it helpful to read information about the cancer type you have.
. The type of radiotherapy you have
. Other treatments you are also having, such as chemotherapy.
Late and long-term side effects of radiotherapy
After having radiotherapy, there is a small risk you will have side effects that:
. Do not get better after treatment – these are called long‑term side effects
. Only start months or years later – these are called late side effects.
This risk may be higher if you are also having other treatments, such as chemotherapy.
Before you decide to have cancer treatment, your team will explain your risk of developing these side effects. Even if it is not very likely, it is important that you understand and think about these long-term risks.
Recovery from radiotherapy
You may have mixed emotions when you get to the end of your radiotherapy and begin to recover. You will probably feel relieved, but you may also feel anxious and uncertain.
You may feel ready to get on with your life after radiotherapy, but sometimes you may feel less positive.
It can take time to recover and you may feel tired for a while. You may also have new challenges to cope with, such as physical effects caused by the cancer or its treatment. It usually takes time to adjust to these and find out what is now normal for you. Complementary therapies may help you feel better and reduce any stress and anxiety.
When your treatment is over, you may want to think about making some positive changes to your lifestyle. Many people find that over time they settle back into their usual routines. But it is important to remember that support is available to help you with any physical or emotional problems you have.
- Hormone therapy. Some types of cancer are fueled by your body's hormones. Examples include breast cancer and prostate cancer. Removing those hormones from the body or blocking their effects may cause the cancer cells to stop growing.
What are hormones?
Hormones are substances produced naturally in the body. They act as chemical messengers and influence the growth and activity of cells.
Hormones are produced by a number of different organs and glands, which together are known as the endocrine system.
What is hormonal therapy?
Hormonal therapies work by altering the production or activity of particular hormones in the body. They are most commonly used to treat breast cancer and prostate cancer. The type of hormone therapy given depends on the type of cancer being treated.
There are several different types of hormonal therapy. They are usually given as either tablets or injections.
How Hormone Therapy Works against Cancer
Hormone therapy is used to:
. Treat cancer. Hormone therapy can lessen the chance that cancer will return or stop or slow its growth.
. Ease cancer symptoms. Hormone therapy may be used to reduce or prevent symptoms in men with prostate cancer who are not able to have surgery or radiation therapy.
Types of Hormone Therapy
Hormone therapy falls into two broad groups, those that block the body’s ability to produce hormones and those that interfere with how hormones behave in the body.
Hormone therapy does not work for all cancers. Cancers that can be hormone sensitive include:
. Breast cancer
. Prostate cancer
. Ovarian cancer
. Womb cancer (also called uterine or endometrial cancer)
Read more about: Bladder Cancer Staging
Read more about: bladder stone
Who Receives Hormone Therapy
Hormone therapy is used to treat prostate and breast cancers that use hormones to grow. Hormone therapy is most often used along with other cancer treatments. The types of treatment that you need depend on the type of cancer, if it has spread and how far, if it uses hormones to grow, and if you have other health problems.
How Hormone Therapy is used with other Cancer Treatments
When used with other treatments, hormone therapy can:
. Make a tumor smaller before surgery or radiation therapy. This is called neo-adjuvant therapy.
. Lower the risk that cancer will come back after the main treatment. This is called adjuvant therapy.
. Destroy cancer cells that have returned or spread to other parts of your body.
Hormone Therapy Side Effects
Because hormone therapy blocks your body’s ability to produce hormones or interferes with how hormones behave, it can cause unwanted side effects. The side effects you have will depend on the type of hormone therapy you receive and how your body responds to it. People respond differently to the same treatment, so not everyone gets the same side effects. Some side effects also differ if you are a man or a woman.
Some common side effects for men who receive hormone therapy for prostate cancer include:
. Hot flashes
. Loss of interest in or ability to have sex
. Weakened bones
. Diarrhea
. Nausea
. Enlarged and tender breasts
. Fatigue
Some common side effects for women who receive hormone therapy for breast cancer include:
. Hot flashes
. Vaginal dryness
. Changes in your periods if you have not yet reached menopause
. Loss of interest in sex
. Nausea
. Mood changes
. Fatigue
What to expect when receiving Hormone Therapy
How Hormone Therapy is given
Hormone therapy may be given in many ways. Some common ways include:
. Oral. Hormone therapy comes in pills that you swallow.
. Injection. The hormone therapy is given by a shot in a muscle in your arm, thigh, or hip, or right under the skin in the fatty part of your arm, leg, or belly.
. Surgery. You may have surgery to remove organs that produce hormones. In women, the ovaries are removed. In men, the testicles are removed.
- Targeted drug therapy. Targeted drug treatment focuses on specific abnormalities within cancer cells that allow them to survive.
What is targeted therapy?
Targeted therapy uses drugs to find and attack cancer cells. There are many different types of targeted therapy. Each type targets something in or around the cancer cell that is helping it grow and survive. In fact, Targeted therapy is the foundation of precision medicine. It is a type of cancer treatment that targets the changes in cancer cells that help them grow, divide, and spread. As researchers learn more about the cell changes that drive cancer, they are better able to design promising therapies that target these changes or block their effects.
A targeted therapy can belong to more than one of these groups. For example, a monoclonal antibody may also block cancer cell growth. So it may also be called a cancer growth inhibitor. Some types of targeted therapy are also an immunotherapy.
Read more about: Common side effects of thyroid cancer treatment
Read more about: What happens during radical prostatectomy?
Types of targeted therapy
. Angiogenesis inhibitors
Tumors need a blood supply to survive. Without a good blood supply, the tumor does not get the oxygen and nutrients it needs. This may slow the tumor’s growth, or sometimes cause it to shrink.
Angiogenesis inhibitors block the chemical signals that cells use to make blood vessels grow. This makes it difficult for a tumor to develop the network of blood vessels it needs to get a blood supply.
. Cancer growth inhibitors
Chemical signals tell cells in the body how and when to develop and divide. Cancer growth inhibitors make it difficult for cancer cells to receive these signals. By blocking the signals, these drugs may stop cancer cells from developing or dividing. This may slow the growth of a cancer.
. Monoclonal antibodies
All cells have receptors on their surface. Receptors help cells send or receive signals. A receptor is a bit like a lock. Only the right key fits the lock. Another cell or substance can only connect to the receptor if it is the right fit.
Monoclonal antibodies are made so they can only connect to one type of receptor. Most monoclonal antibodies target receptors that are mainly found on cancer cells. Some target receptors that are found on other cells in the body.
By connecting to the cell’s receptor, a monoclonal antibody could:
. Block signals that tell cancer cells to grow and divide (also called a cancer growth inhibitor)
. Block signals that help cancer cells develop a blood supply (also called an angiogenesis inhibitor)
. Block signals that stop white blood cells attacking cancer cells (also called a checkpoint inhibitor)
. Help the immune system recognize cancer cells (also called an immunotherapy)
. Block signals to protect the bones from damage causes by some types of cancer or cancer treatments.
. Carry a chemotherapy drug straight to the cancer cell.
Who is treated with targeted therapy?
For some types of cancer, most patients with that cancer will have a target for a certain drug, so they can be treated with that drug. But, most of the time, your tumor will need to be tested to see if it contains targets for which we have drugs.
To have your tumor tested for targets, you may need to have a biopsy. A biopsy is a procedure in which your doctor removes a piece of the tumor for testing. There are some risks to having a biopsy. These risks vary depending on the size of the tumor and where it is located. Your doctor will explain the risks of having a biopsy for your type of tumor.
How does targeted therapy work against cancer?
Most types of targeted therapy help treat cancer by interfering with specific proteins that help tumors grow and spread throughout the body. They treat cancer in many different ways. They can:
. Help the immune system destroy cancer cells. One reason that cancer cells thrive is because they are able to hide from your immune system. Certain targeted therapies can mark cancer cells so it is easier for the immune system to find and destroy them. Other targeted therapies help boost your immune system to work better against cancer.
. Stop cancer cells from growing. Healthy cells in your body usually divide to make new cells only when they receive strong signals to do so. These signals bind to proteins on the cell surface, telling the cells to divide. This process helps new cells form only as your body needs them. But, some cancer cells have changes in the proteins on their surface that tell them to divide whether or not signals are present. Some targeted therapies interfere with these proteins, preventing them from telling the cells to divide. This process helps slow cancer’s uncontrolled growth.
. Stop signals that help form blood vessels. Tumors need to form new blood vessels to grow beyond a certain size. In a process called angiogenesis, these new blood vessels form in response to signals from the tumor. Some targeted therapies called angiogenesis inhibitors are designed to interfere with these signals to prevent a blood supply from forming. Without a blood supply, tumors stay small. Or, if a tumor already has a blood supply, these treatments can cause blood vessels to die, which causes the tumor to shrink. Learn more about Angiogenesis Inhibitors.
. Deliver cell-killing substances to cancer cells. Some monoclonal antibodies are combined with toxins, chemotherapy drugs, and radiation. Once these monoclonal antibodies attach to targets on the surface of cancer cells, the cells take up the cell-killing substances, causing them to die. Cells that don’t have the target will not be harmed.
. Cause cancer cell death. Healthy cells die in an orderly manner when they become damaged or are no longer needed. But, cancer cells have ways of avoiding this dying process. Some targeted therapies can cause cancer cells to go through this process of cell death.
. Starve cancer of the hormones it needs to grow. Some breast and prostate cancers require certain hormones to grow. Hormone therapies are a type of targeted therapy that can work in two ways. Some hormone therapies prevent your body from making specific hormones. Others prevent the hormones from acting on your cells, including cancer cells.
Are there drawbacks to targeted therapy?
Targeted therapy does have some drawbacks. These include:
. Cancer cells can become resistant to targeted therapy. For this reason, they may work best when used with other types of targeted therapy or with other cancer treatments, such as chemotherapy and radiation.
. Drugs for some targets are hard to develop. Reasons include the target’s structure, the target’s function in the cell, or both.
What are the side effects of targeted therapy?
Targeted therapy can cause side effects. The side effects you may have depend on the type of targeted therapy you receive and how your body reacts to the therapy.
The most common side effects of targeted therapy include diarrhea and liver problems. Other side effects might include problems with blood clotting and wound healing, high blood pressure, fatigue, mouth sores, nail changes, the loss of hair color, and skin problems. Skin problems might include rash or dry skin. Very rarely, a hole might form through the wall of the esophagus, stomach, small intestine, large bowel, rectum, or gallbladder.
There are medicines for many of these side effects. These medicines may prevent the side effects from happening or treat them once they occur.
Most side effects of targeted therapy go away after treatment ends.
Read more about Colorectal cancer treatments
Read more about Stages of fissure healing
How often will I receive targeted therapy?
How often and how long you receive targeted therapy depends on:
. Your type of cancer and how advanced it is
. The type of targeted therapy
. How your body reacts to treatment
You may have treatment every day, every week, or every month. Some targeted therapies are given in cycles. A cycle is a period of treatment followed by a period of rest. The rest period gives your body a chance to recover and build new healthy cells.
- Immunotherapy. Immunotherapy, also known as biological therapy, uses your body's immune system to fight cancer. Cancer can survive unchecked in your body because your immune system doesn't recognize it as an intruder. Immunotherapy can help your immune system "see" the cancer and attack it.
What is immunotherapy?
The immune system protects the body against illness and infection. Immunotherapy is a type of cancer treatment that helps your immune system fight cancer. The immune system helps your body fight infections and other diseases. It is made up of white blood cells and organs and tissues of the lymph system.
Immunotherapy is a type of biological therapy. Biological therapy is a type of treatment that uses substances made from living organisms to treat cancer.
How does immunotherapy work against cancer?
As part of its normal function, the immune system detects and destroys abnormal cells and most likely prevents or curbs the growth of many cancers. For instance, immune cells are sometimes found in and around tumors. These cells, called tumor-infiltrating lymphocytes or TILs, are a sign that the immune system is responding to the tumor. People whose tumors contain TILs often do better than people whose tumors don’t contain them.
Even though the immune system can prevent or slow cancer growth, cancer cells have ways to avoid destruction by the immune system. For example, cancer cells may:
. Have genetic changes that make them less visible to the immune system.
. Have proteins on their surface that turn off immune cells.
. Change the normal cells around the tumor so they interfere with how the immune system responds to the cancer cells.
Immunotherapy helps the immune system to better act against cancer.
Read more about Femoral vs inguinal hernia
Read more about Femoral hernia
What are the types of immunotherapy?
Several types of immunotherapy are used to treat cancer. These include:
. Immune checkpoint inhibitors, which are drugs that block immune checkpoints. These checkpoints are a normal part of the immune system and keep immune responses from being too strong. By blocking them, these drugs allow immune cells to respond more strongly to cancer.
. T-cell transfer therapy, which is a treatment that boosts the natural ability of your T cells to fight cancer. In this treatment, immune cells are taken from your tumor. Those that are most active against your cancer are selected or changed in the lab to better attack your cancer cells, grown in large batches, and put back into your body through a needle in a vein.
T-cell transfer therapy may also be called adoptive cell therapy, adoptive immunotherapy, or immune cell therapy.
. Monoclonal antibodies, which are immune system proteins created in the lab that are designed to bind to specific targets on cancer cells. Some monoclonal antibodies mark cancer cells so that they will be better seen and destroyed by the immune system. Such monoclonal antibodies are a type of immunotherapy.
Monoclonal antibodies may also be called therapeutic antibodies.
. Treatment vaccines, which work against cancer by boosting your immune system’s response to cancer cells. Treatment vaccines are different from the ones that help prevent disease.
. Immune system modulators, which enhance the body’s immune response against cancer. Some of these agents affect specific parts of the immune system, whereas others affect the immune system in a more general way.
Immunotherapy Side Effects
Immunotherapy can cause side effects, many of which happen when the immune system that has been revved-up to act against the cancer also acts against healthy cells and tissues in the body. Different people have different side effects. The ones you have and how they make you feel will depend on how healthy you are before treatment, your type of cancer, how advanced it is, the type of immunotherapy you are getting, and the dose.
You might be on immunotherapy for a long time, and side effects can occur at any point during and after treatment. Doctors and nurses cannot know for certain when or if side effects will occur or how serious they will be. So, it is important to know what signs to look for and what to do if you start to have problems.
Some side effects are common with all types of immunotherapy. For instance, you might have skin reactions at the needle site, which include:
. Pain
. Swelling
. Soreness
. Redness
. Itchiness
. Rash
You may have flu-like symptoms, which include:
. Fever
. Chills
. Weakness
. Dizziness
. Nausea or vomiting
. Muscle or joint aches
. Fatigue
. Headache
. Trouble breathing
. Low or high blood pressure
Other side effects might include:
. Swelling and weight gain from retaining fluid
. Heart palpitations
. Sinus congestion
. Diarrhea
. Risk of infection
. Organ inflammation
Some types of immunotherapy may cause severe or even fatal allergic and inflammation-related reactions. However, these reactions are rare.
Read more about : Pancreatic cancer
Read more about : Prostate Cancer Treatments Pros and Cons
How often do you receive immunotherapy?
How often and how long you receive immunotherapy depends on:
. Your type of cancer and how advanced it is
. The type of immunotherapy you get
. How your body reacts to treatment
You may have treatment every day, week, or month. Some types of immunotherapy given in cycles. A cycle is a period of treatment followed by a period of rest. The rest period gives your body a chance to recover, respond to the immunotherapy, and build new healthy cells.
- Stem cell and Bone marrow transplant. Your bone marrow is the material inside your bones that makes blood cells from blood stem cells. A bone marrow transplant, also knowns as a stem cell transplant, can use your own bone marrow stem cells or those from a donor.
A bone marrow transplant allows your doctor to use higher doses of chemotherapy to treat your cancer. It may also be used to replace diseased bone marrow.
What are Stem Cell Transplants?
Stem cell transplants are procedures that restore blood-forming stem cells in people who have had theirs destroyed by the very high doses of chemotherapy or radiation therapy that are used to treat certain cancers.
Blood-forming stem cells are important because they grow into different types of blood cells. The main types of blood cells are:
. White blood cells, which are part of your immune system and help your body fight infection
. Red blood cells, which carry oxygen throughout your body
. Platelets, which help the blood clot
You need all three types of blood cells to be healthy.
Types of Stem Cell Transplants
In a stem cell transplant, you receive healthy blood-forming stem cells through a needle in your vein. Once they enter your bloodstream, the stem cells travel to the bone marrow, where they take the place of the cells that were destroyed by treatment. The blood-forming stem cells that are used in transplants can come from the bone marrow, bloodstream, or umbilical cord. Transplants can be:
. Autologous, which means the stem cells come from you, the patient
. Allogeneic, which means the stem cells come from someone else. The donor may be a blood relative but can also be someone who is not related.
. Syngeneic, which means the stem cells come from your identical twin, if you have one.
To reduce possible side effects and improve the chances that an allogeneic transplant will work, the donor’s blood-forming stem cells must match yours in certain ways.
How Stem Cell Transplants work against cancer
Stem cell transplants do not usually work against cancer directly. Instead, they help you recover your ability to produce stem cells after treatment with very high doses of radiation therapy, chemotherapy, or both.
However, in multiple myeloma and some types of leukemia, the stem cell transplant may work against cancer directly. This happens because of an effect called graft-versus-tumor that can occur after allogeneic transplants. Graft-versus-tumor occurs when white blood cells from your donor (the graft) attack any cancer cells that remain in your body (the tumor) after high-dose treatments. This effect improves the success of the treatments.
Who receives Stem Cell Transplants
Stem cell transplants are most often used to help people with leukemia and lymphoma. They may also be used for neuroblastoma and multiple myeloma.
Stem Cell Transplants Side Effects
The high doses of cancer treatment that you have before a stem cell transplant can cause problems such as bleeding and an increased risk of infection. Talk with your doctor or nurse about other side effects that you might have and how serious they might be.
If you have an allogeneic transplant, you might develop a serious problem called graft-versus-host disease. Graft-versus-host disease can occur when white blood cells from your donor (the graft) recognize cells in your body (the host) as foreign and attack them. This problem can cause damage to your skin, liver, intestines, and many other organs. It can occur a few weeks after the transplant or much later. Graft-versus-host disease can be treated with steroids or other drugs that suppress your immune system.
The closer your donor’s blood-forming stem cells match yours, the less likely you are to have graft-versus-host disease. Your doctor may also try to prevent it by giving you drugs to suppress your immune system.
How long it takes to have a Stem Cell Transplant
A stem cell transplant can take a few months to complete. The process begins with treatment of high doses of chemotherapy, radiation therapy, or a combination of the two. This treatment goes on for a week or two. Once you have finished, you will have a few days to rest.
Next, you will receive the blood-forming stem cells. The stem cells will be given to you through an IV catheter. This process is like receiving a blood transfusion. It takes 1 to 5 hours to receive all the stem cells.
After receiving the stem cells, you begin the recovery phase. During this time, you wait for the blood cells you received to start making new blood cells.
Even after your blood counts return to normal, it takes much longer for your immune system to fully recover—several months for autologous transplants and 1 to 2 years for allogeneic or syngeneic transplants.
Special diet needs before a stem cell transplant
The high-dose treatments that you have before a stem cell transplant can cause side effects that make it hard to eat, such as mouth sores and nausea. Tell your doctor or nurse if you have trouble eating while you are receiving treatment. You might also find it helpful to speak with a dietitian.
8. Supportive and other treatments. Other treatments which can be used as part of the main cancer treatment and to treat side effects are as follows:
. Blood transfusion, Blood transfusions are a simple way of treating anaemia, which is a low number of red blood cells. When you have a blood transfusion you are given blood from carefully screened donors. The transfusion increases the number of red blood cells in your blood. This means that more oxygen can be carried around the body to your tissues and organs. This will increase your energy levels and reduce your breathlessness.
. Erythropoietin (EPO), Erythropoietin (EPO) is a type of protein called a growth factor. It is used to treat anaemia due to cancer or its treatment.
. G-CSF (Granulocyte-colony stimulating factor), Granulocyte-colony stimulating factor (G-CSF) is a type of drug called a growth factor. This helps your body make more white blood cells. In fact, it increases the number of some types of blood cells in the blood. It can be used with chemotherapy. It can also be used before and after a stem cell transplant.
. Hyperbaric oxygen (HBO) treatment, Hyperbaric oxygen (HBO) treatment increases the amount of oxygen in the blood. It is used to help with some side effects of cancer treatment. Hyperbaric oxygen treatment (HBO) involves giving the body extra oxygen. 'Hyper' means increased and 'baric' relates to pressure. Oxygen is one of the gases in the air, and it is essential for life.
. Nephrostomy, A nephrostomy is a tube that drains urine from the kidney if there is a blockage in the urinary system. People with cancer may need a nephrostomy if there is a blockage in the urinary system. A nephrostomy is a thin, plastic tube (catheter) that is inserted through the skin on your back and into your kidney. Some people may have a catheter into each kidney.
The nephrostomy drains urine from one or both kidneys into a collecting bag outside your body. The bag has a tap so you can empty it. You may still pass some urine in a normal way even when you have a nephrostomy tube in one, or both, of your kidneys.
. Photodynamic therapy (PDT), PDT uses light sources and a light-sensitive drug to destroy cancer cells. It’s used for some cancers and some pre-cancerous conditions. In fact, Photodynamic therapy (PDT) is a treatment that uses a light-sensitive drug and a laser or light source to destroy cancer cells.
The drug is attracted to the cancer cells. But it does not become active in these cells until a light is shone on it. Using a certain light or laser will activate the drug to release a type of oxygen that kills the nearby cancer cells.
Some healthy, normal cells in the body will also be affected by PDT, but these cells usually recover after treatment.
. Plasma exchange, Plasma exchange (plasmapheresis) is a procedure which separates your blood into its different parts: red cells, white cells, platelets and plasma. The plasma is removed from the blood and replaced by a plasma substitute.
. Platelet transfusion, Platelets are tiny cells in your blood that help to stop bleeding. Some cancers or cancer treatments can lead to low platelets. When you have a platelet transfusion you are given platelets from carefully screened donors.
. Radiofrequency ablation (RFA), RFA is a treatment that uses heat to destroy cancer cells. It is mainly used for cancer of the liver, lung, or kidney. It may sometimes be used to treat other cancers.
. Steroids, Steroids can be used as part of cancer treatment, or to help with the side effects of treatment. Steroids are substances that are naturally produced in the body. Steroids help to control many different functions in our bodies.
. Bisphosphonates, Bisphosphonates are drugs that help to strengthen bones and reduce the risk of a bone breaking (fracture). They can help relieve bone pain and may be used to treat high levels of calcium in the blood (hypercalcaemia).
- Clinical trials. Many people are offered a trial as part of treatment. Find out more to help you decide if a trial is right for you.
Read more about : Femoral Hernia vs. Inguinal Hernia
Read more about : Anal fissure surgery
What are clinical trials?
Clinical trials are medical research studies involving people. Doctors may use cancer clinical trials to:
. Test new treatments to see if they work better than current treatments
. Find which treatments have fewer side effects
. Find new ways to combine treatments to see if they work better
. Test new cancer drugs to find out more about them and their side effects
. Improve the way treatments are given to try to reduce side effects.
Results from clinical trials can improve cancer treatments and help people live longer. Trials can also look at improving things like diagnosis and symptom management.
- Alternative therapies. Many alternative therapies claim to treat or even cure cancer. But no alternative therapies have ever been proven to cure cancer or slow its growth.
What are alternative therapies?
Alternative therapies are different from complementary therapies. They are used instead of conventional medical treatments. They may claim to actively treat or even cure cancer. But there is no scientific proof to support these claims.
No alternative therapies have ever been proven to cure cancer or slow its growth. We do not advocate alternative therapies.
There have been cases where false claims about alternative therapies have led some people to refuse conventional treatments that could have helped them. No reputable alternative therapist will claim to be able to cure cancer.
There are many types of alternative therapy. The alternative therapies most well-known by people with cancer are as bellows:
. Amygdalin (Laetrile®, vitamin B17)
Amygdalin is a compound found in bitter almonds, peach stones and apricot stones. When amygdalin is processed by the body, it can be changed to cyanide, a type of poison.
A man-made form of amygdalin is called laetrile. It is also called vitamin B17, although it is not a vitamin. If you are thinking of taking laetrile, talk to your cancer doctor.
Read more about : Sleeping position for fissure
Read more about : Foods that cure fissures
Why some people use laetrile?
Many websites that sell laetrile claim it can slow or stop the growth of cancer. They also claim it can poison cancer cells, without damaging normal cells and tissues. But there is no medical evidence to support this.
A review of studies looking at the outcomes for people with cancer taking Laetrile found no evidence that it can control or cure cancer.
Possible side effects of laetrile
Laetrile can have serious side effects. Some people have had cyanide poisoning while taking it and several people have died as a result.
The sale of laetrile has been banned by the European Commission and by the Food and Drugs Administration (FDA) in the USA. If you buy laetrile, there is no way of knowing what it contains, or if it is contaminated with other substances.
. Essiac® (Vitaltea®, Flor-essence®)
Essiac is taken as a drink and sold as a nutritional supplement. It is important to talk to your cancer doctor before you take Essiac during cancer treatment, or with any other medicines.
Why some people use Essiac
Some websites claim Essiac can slow down the growth of cancer, or even cure it. But there is no medical evidence that taking Essiac helps treat cancer or improve your quality of life.
Possible side effects of Essiac
Essiac interferes with an enzyme in the body that regulates hormones and vitamin D. It also has an effect on how the body deals with toxins. This may mean taking Essiac with other treatments could make them less effective or increase side effects.
. Metabolic therapy
Metabolic treatments vary from one therapist to another. One of the most well-known is called Gerson therapy. This may include:
. A diet of raw fruit and vegetables
. No processed foods or salt
. Vitamins and minerals
. Enzymes or chemicals
. Coffee enemas.
If you have any questions about alternative diets or are thinking of following one, get advice from your doctor, specialist nurse or dietitian.
Why some people use metabolic therapies
Metabolic therapists claim they can treat cancer by removing toxins and strengthening the immune system. No medical evidence has shown that either of these claims are true.
One study compared the results of using a metabolic therapy with chemotherapy. It found that the patients who had the chemotherapy survived three times longer and had better quality of life than those who chose metabolic therapy.
Possible side effects of metabolic therapy
Possible side effects of metabolic or Gerson therapy include nausea, vomiting, stomach cramps, a high temperature and headaches. The high levels of hormones and extracts used can sometimes make people feel unwell. Risks of using coffee enemas include infections. They can also cause serious damage to the large bowel.
. Diets that claim to treat cancer
There are a number of diets, as well as the Gerson diet (above), that claim to treat cancer. Talk to your cancer doctor, nurse or dietitian before cutting out any food group from your diet.
Why some people use diets to treat cancer?
Some diets claim to rid the body of toxins. Many of these diets are vegetarian or vegan. They involve eating food that is raw, sugar-free and low in salt. Sometimes vegetable or fruit juices, and high doses of vitamins, minerals or enzymes are used.
Other diets are based on claims that some foods ‘feed’ cancer or affect the pH (acidity) of the body.
There is no medical evidence that these diets can cure cancer or help people with advanced cancer live longer.
Possible side effects of diets that claim to treat cancer
If you choose to follow a diet that cuts out particular types of food, it is important to make sure you aren’t missing out on important nutrients.
Diets that are high in fibre and low in calories and protein are not appropriate for people who have problems maintaining their weight because of cancer or its treatment.
. Megavitamin therapy
This type of alternative therapy involves taking very large doses of vitamins. High-dose vitamin C is one of the most common types of megavitamin therapy.
However, there is no evidence that taking large doses of vitamins is helpful in treating cancer.
It is important to tell your cancer doctor before having high doses of vitamin C during, or within a few weeks of, cancer treatment.
Possible side effects of megavitamin therapy
High-dose vitamin C can make many cancer treatment drugs less effective. These include cisplatin, doxorubicin, imatinib and vincristine. It may also interfere with how radiotherapy works.
High-dose vitamin C may also interact with some complementary and alternative therapies.
High-dose vitamin C is not suitable for people who have kidney problems, iron overload (haemachromatosis) or a lack of G6PDH (an enzyme which helps red blood cells work properly).
Cancer Treatment Surgeons
How can I find the best Cancer Treatment surgeon in Iran?
It is important that you seek the assistance of experienced and skilled Cancer Treatment surgeons in Iran who have provided a suitable condition for patients with limited budgets to treat their cancers in Iran easily. It is worth explaining that the quality provided by Iranian surgeons is far higher than other countries including Turkey and India.
Oncology Hospitals & Clinics in Iran
Tehran hospitals
- Imam Khomeini Hospital
- Pars Hospital
- Pasteurno Hospital
- Erfan Hospital
- Nikan Hospital
- Jam Hospital
- Roshana Cancer Center
Shiraz hospitals
- Shiraz Central Hospital
- Dena Hospital
- Amir Hospital
- Pardis Clinic
Mashhad Hospitals
- Razavi Hospital
- Reza Radiotherapy Oncology Center (RROC)
Cost of Cancer Treatment in Iran
The cost of treating a cancer in Iran can vary according to each individual’s case and will be determined by the type of cancer you have and an in-person assessment with the doctor.




12 Comments
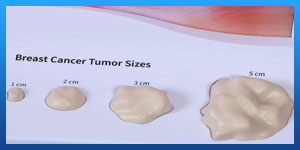
I read somewhere about Inflammatory breast cancer, What is inflammation in breast cancer if I right?
Considered a rare disease, inflammatory breast cancer (IBC) typically forms in the soft tissues, blocking lymph vessels in the breast skin. That’s why the breast often becomes firm, tender, itchy, red and warm, from the increase in blood flow and a build-up of white blood cells. IBC differs from other forms of breast cancer, especially in symptoms, prognosis and treatment. The term “inflammatory” is not meant to reflect what’s happening inside the breast, only in how the breast appears. When an infection or injury causes the breasts to become inflamed, they often become tender, swollen, red and itchy, but the underlying cause is not inflammation.
Does sleeping with a bra cause breast cancer?
Sleeping in a bra will not make a girl’s breasts perkier or prevent them from getting saggy. And it will not cause a girl to develop cancer or stunt her breast growth. (It’s also not true that underwire bras cause breast cancer.) Some women want to wear abra to bed because they think it feels more comfortable
What average risk for breast cancer?
On average, an individual woman has a 1-in-8 chance of developing breast cancerover an 80-year lifespan. The absolute risk of developing breast cancer during a particular decade of life is lower than 1 in 8. The younger you are, the lower the risk
Can eating certain foods cause breast cancer?
To date, a link between foods and breast cancer has not been identified. A few studies have found a possible link between fat and breast cancer, but further research needs to be completed. As a general rule of thumb, the best practice is to eat a healthy diet rich in lean proteins, whole grains and fibrous fruits and vegetables. Most importantly, please talk to your doctor before beginning any diet or nutrition regiment.
Hi Dr.I have three lymph nodes involved in breast cancer that my surgeon underwent surgery and after seven sessions of chemotherapy and twenty-five radiotherapy sessions, my doctor advised me to take the Herceptin vaccine, I have heard from some people that this vaccine is not very effective, On the other hand, this drug is expensive, so I was hesitant to inject this vaccine, maybe you can guide me.
Dear friend if you have HER-2 + 3 approved, you should do Herceptin.
Hello there
Do you guys have a specialized center and personnel for sarcoma treatment, please?
Thanks
hello dear, our specialist get in touch with you as soon as possible.