Cornea transplant in Iran
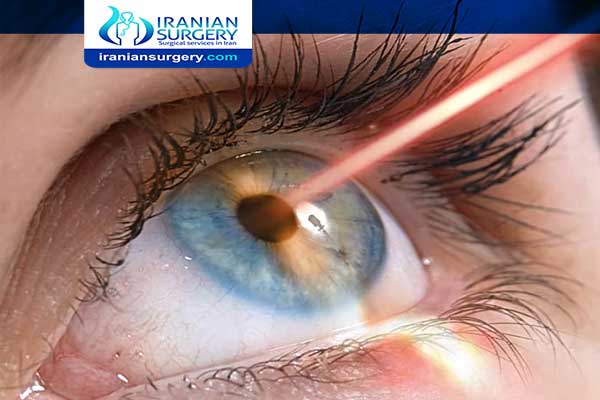
How long does a corneal transplant take?
What is a Cornea Transplant?
A cornea transplant is a surgical procedure that involves removing all or part of a damaged cornea and replacing it with healthy corneal tissue from a donor.
The type of cornea transplant a person receives will depend on which layer of the cornea is damaged, as well as the extent of the damage.
Your cornea is the transparent, dome-shaped surface of your eye that accounts for a large part of your eye's focusing power.
A cornea transplant can restore vision, reduce pain and improve the appearance of a damaged or diseased cornea.
Most cornea transplant procedures are successful. But cornea transplant carries a small risk of complications, such as rejection of the donor cornea.
Read more about : Iranian eye surgeons restored vision to the eyes of an Omani child.
General information about Cornea Transplant Procedure
The following table describes general information about Cornea Transplant Procedure including Cornea Transplant cost in Iran, recovery time, and to name but a few.
General Information |
|
Cost | $ 3000-3500 |
Anesthesia | Local/General |
Hospital Stay | The Same Day |
Back to Work | 2-3 Weeks |
Duration of Operation | 1-2 Hours |
Minimum Stay in Iran | 2 Weeks |
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best eye surgeons in Iran. The price of a Cornea Transplant Procedure in Iran can vary according to each individual’s case and will be determined based on an in-person assessment with the doctor and the type surgery you undergo. So if you are looking for the cost of Cornea Transplant Procedure in Iran, you can contact us and get free consultation from Iranian surgery.
Read more about : What to Expect after Corneal Transplant?
Read more about : What should I expect after my cornea transplant?
Before Cornea Transplant Procedure
Why it's done
A cornea transplant is most often used to restore vision to a person who has a damaged cornea. A cornea transplant may also relieve pain or other signs and symptoms associated with diseases of the cornea.
A number of conditions can be treated with a cornea transplant, including:
. A cornea that bulges outward (keratoconus)
. Fuchs' dystrophy
. Thinning of the cornea
. Cornea scarring, caused by infection or injury
. Clouding of the cornea
. Swelling of the cornea
. Corneal ulcers, including those caused by infection
. Complications caused by previous eye surgery
What does the cornea do?
The clear, dome-shaped cornea protects the eyes against dirt, germs, other particles, and damaging UV light. The cornea, working together with the lens of the eye, focus light that enters the eye so that vision can be clear.
The cornea consists of five layers:
. The epithelium: This is the outermost layer of the cornea. It helps to protect the cornea and focus light.
. Bowman’s layer: A very thin layer that sits between the epithelium and the stroma.
. Stroma: This layer helps to strengthen the cornea.
. Descemet’s membrane: A very thin layer that separates the stroma from the endothelium.
. Endothelium: The innermost layer of the cornea. Cells in this layer work as a pump to drain fluid out of the stroma.
What symptoms may indicate I need a cornea transplant?
If you have a damaged cornea, you may experience symptoms including:
. Eye pain
. Blurred vision
. Cloudy vision
Your ophthalmologist will determine the cause and other possible treatments that may resolve these symptoms. If your cornea cannot be repaired using other methods, your surgeon may recommend a cornea transplant.
Risks and Complications
Cornea transplant is a relatively safe procedure. Still, it does carry a small risk of serious complications, such as:
. Eye infection
. Increased risk of clouding of the eye's lens (cataract)
. Pressure increase within the eyeball (glaucoma)
. Problems with the stitches used to secure the donor cornea
. Rejection of the donor cornea
. Swelling of the cornea
. Bleeding from the eye
. Fluid leakage from your cornea
. Detached retina (tissue lining the back of the eye pulls away from the eye).
. Visual acuity problems (sharpness of the vision) caused by an irregular curve in the shape of the cornea.
. Detachment of the corneal transplant (for the endothelial transplant which is held in place by an air bubble).
Read more about : Lasik eye surgery
Signs and symptoms of cornea rejection
In some cases, your body's immune system may mistakenly attack the donor cornea. This is called rejection, and it may require medical treatment or another cornea transplant. Rejection occurs in about 10 percent of corneal transplants.
Make an appointment with your eye doctor if you notice any signs and symptoms of rejection, such as:
. Eye pain
. Sensitivity to light
. Red eyes
. Cloudy or hazy vision
Below are some factors that could increase the risk of tissue rejection.
. The donor cornea
The main factors that affect donor tissue rejection are human leukocyte antigen (HLA) incompatibilities and blood type incompatibilities.
HLAs are a set of proteins in the body that regulate the immune system.
The type of antigens and antibodies that make up a person’s blood determine their blood type.
If the donor HLA or blood type is incompatible with those of the recipient, the recipient is more likely to reject the donor tissue.
. Health of the recipient
Certain preexisting conditions can increase a person’s risk of an immune reaction. Some of these conditions include:
. Herpes keratitis, which is a viral infection of the eye
. Uveitis, or inflammation of the structures in the middle of the eye
. Atopic dermatitis, which is a chronic inflammatory skin condition
Read more about : Cataract surgery
. Age of the recipient
According to a 2017 review, younger people are more likely to reject a cornea transplant, compared to older people. This is partly due to the fact that younger people tend to have more robust immune responses.
How you prepare
Before cornea transplant surgery, you will undergo:
. A thorough eye exam. Your eye doctor looks for conditions that may cause complications after surgery.
. Measurements of your eye. Your eye doctor determines what size donor cornea you need.
. A review of all medications and supplements you're taking. You may need to stop taking certain medications or supplements before or after your cornea transplant.
. Treatment for other eye problems. Unrelated eye problems, such as infection or inflammation, may reduce your chances of a successful cornea transplant. Your eye doctor will work to treat those problems before your surgery.
Your doctor will discuss what to expect during the procedure and explain the risks of the procedure.
Finding a donor cornea
Most corneas used in cornea transplants come from deceased donors. Unlike with organs such as livers and kidneys, people needing cornea transplants generally will not need to endure long waits. That's because many people specifically request that their corneas be available for donation after they die, unless they have had certain conditions, so more corneas are available for transplantation.
Corneas may not be used from donors who had several conditions, such as certain central nervous system conditions, infections, and prior eye surgery or eye conditions, or from people who died from an unknown cause.
 During Cornea Transplant Procedure
During Cornea Transplant Procedure
How is a cornea transplant performed?
Your doctor and the anesthesia team will review your medical history, answer your questions and confirm the surgical plan. The anesthesia team will administer either sedation or general anesthesia (making you unconscious), depending on your medical condition and what you and your doctor have discussed. Numbing medication will be applied to the eye.
The surgery itself is an outpatient procedure (you will not be staying at the hospital or eye center). The surgery typically takes less than 2 hours to perform.
Your surgeon will recommend one of three surgical options for cornea transplant. The method your surgeon chooses depends on the cause of the damage to the cornea, the condition of your cornea, and your unique needs. In some cases, a corneal transplant may not improve your vision, and your surgeon may recommend against surgery.
Regardless of the type of transplant you receive, your new cornea will come from a deceased human organ donor. Every donor cornea undergoes thorough testing to make sure it is safe for transplant.
Types of procedure
The most common type of cornea transplant is a keratoplasty. There are three types of keratoplasty procedure:
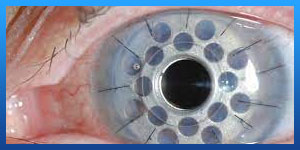
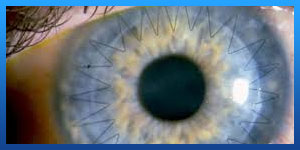
. Penetrating keratoplasty
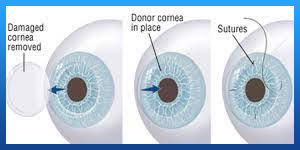
Penetrating keratoplasty is also called a full thickness cornea transplantation. Developed over 100 years ago, the modern version of this surgery continues to help thousands of people each year. In this procedure, your surgeon uses a small circular blade to remove the entire center part of the damaged cornea and replaces it with a healthy same-shaped piece of donor cornea.
. Deep anterior lamellar keratoplasty
If the innermost layer of your cornea is healthy, but the middle and outer layers are damaged, your surgeon may perform a partial thickness cornea transplant. This procedure is also known as deep anterior lamellar keratoplasty. During this surgery, your surgeon removes the middle and outer layers of your cornea and replaces them with healthy corneal tissue.
. Endothelial keratoplasty
This procedure may help if the innermost layer of your cornea, the endothelium, is damaged. This thin layer of endothelial tissue is called Descemet’s membrane. Surgeons perform two types of endothelial keratoplasty surgeries:
. Descemet stripping automated endothelial keratoplasty (DSAEK)
. Descemet membrane endothelial keratoplasty (DMEK)
Each procedure removes damaged endothelial tissue and replaces it with healthy donor tissue. Unlike the other keratoplasty procedures, fewer or no stitches are needed with the endothelial keratoplasty procedures. Instead, an air bubble is used to keep the donor cornea in position. To increase the chance of success, you will need to position yourself face-up for a few days after the surgery so the bubble can keep the corneal tissue in place. The difference between DSAEK and DMEK is the thickness of the donor cornea – DSAEK is thicker, while DMEK is thinner. Your surgeon will decide which type of transplant is best suited for your specific eye condition.
After Cornea Transplant Procedure
What should I expect after my cornea transplant?
For the first few days after surgery, expect your eye to be red, irritated, and sensitive to light. Typically, pain can be controlled with over-the-counter pain relievers that your surgeon can recommend.
Your eye will be covered with an eye patch after your surgery. The eye patch must be worn when you shower and sleep. Your surgeon will also talk about activities you will need to avoid, especially any activities that could result in a direct hit to your eye. For endothelial transplants, you will need to position with your face up (on your back) for a few days after surgery.
You will have a follow-up visit with your surgeon, usually within 24 to 48 hours of your surgery. He or she will remove your eye patch and check on how well your eye is healing. Also, eye drops and ointments will be prescribed to help your eye heal. Eye drops and ointments usually prescribed are both antibiotics (to prevent infection) and corticosteroids (to reduce swelling, inflammation, and to prevent rejection).
Stitches may need to be removed depending on the type of stitches and surgical technique used. If stitches do need to be removed, they may not be removed for several months.
Your surgeon will recommend that you wear glasses or other protective eyewear for a period of time to help protect your eyes. While recovering, you should not rub or press on your eyes. Rubbing can cause damage and interfere with healing.
Once your cornea transplant is completed, you can expect to:
. Receive several medications. Eyedrops and, sometimes, oral medications immediately after cornea transplant and during recovery will help control infection, swelling and pain.
. Wear an eye patch. An eye patch may protect your eye as it heals after your surgery.
. Protect your eye from injury. Plan to take it easy after your cornea transplant, and slowly work your way up to your normal activities, including exercise. For the rest of your life, you'll need to take extra precautions to avoid harming your eye.
. Return for frequent follow-up exams. Expect frequent eye exams in which your doctor looks for complications in the first year after surgery.
What is the prognosis (outlook) for people who have a cornea transplant?
The degree of long-term success depends on a number of factors including the underlying cause of the cornea damage, surgical technique used, expertise of the surgeon, patient’s immune system acceptance of the donor transplant (organ rejection) and other factors. Because the rates vary so greatly, you should ask your doctor about the rate of success in your eye. It is important to keep in mind that vision is usually blurred after surgery and will gradually improve over time. The length of time it takes to return to good vision depends on several factors, including the type of surgery performed. It may take up to 12 months for full vision to be achieved in patients who undergo full thickness tissue transplant. For endothelial transplants (DMEK and DSAEK), good vision is typically achieved within 3 months.
Will I need to wear glasses or contacts after cornea transplant?
An irregular cornea surface is expected following full thickness corneal transplant surgery. This imperfection in the curve of the cornea, called astigmatism, results in distorted vision. Correction with glasses, contact lenses, or additional surgery is often needed. Special types of contact lenses (rigid gas permeable or scleral lenses [a larger lens that lays on the white part of the eye]) are not typically needed following endothelial transplants, but may be needed after penetrating keratoplasty or deep anterior lamellar keratoplasty surgery. Your surgeon will discuss the best options to meet your vision needs.
How soon can I drive after a cornea transplant?
You must not drive on the day of your cornea transplant. Someone must drive you home after surgery and bring you back for your follow-up visit.
If you have good vision in the non-transplant eye, you can legally drive 24 hours after surgery. However, your surgeon may recommend waiting longer before driving.
When can I return to work after a cornea transplant?
It may take a few days to a few weeks before you can return to work. It depends on your level of discomfort, your vision and what activities you perform at work. Jobs that require strenuous activity such as lifting may need more time off from work.
When should I call my surgeon?
Contact your surgeon immediately if you experience any signs of cornea rejection, including:
. Eye pain
. Eye redness
. Hazy or cloudy vision
. Sensitivity to light
If you notice any other problems in your vision after cornea transplant, or you experience symptoms of infection, such as fever, eye drainage, or pain, contact your surgeon.
Cornea Transplant Cost
The cost of Cornea Transplant procedure in Iran is between from $1400_$1600


19 Comments
hello iranian surgery ,
How soon can I drive after a corneal transplant?can I drive after one day?
You must not drive on the day of your cornea transplant. Someone must drive you home after surgery and bring you back for your follow-up visit. If you have good vision in the non-transplant eye, you can legally drive 24 hours after surgery. However, your surgeon may recommend waiting longer before driving.
May ask about Vision After A Cornea Transplant?
Your eyesight should gradually improve a few weeks after a corneal graft, but it could take anywhere from a couple of months up to a year to have stable vision in the eye that receives the donor tissue.
Do I get rid of corneal problems with corneal transplants forever?
Some corneas do last forever, but some need to be replaced due to transplantrejection (which can occur even 20 years later) or due to simple failure of thetransplant’s new cells over time (depending on the age and health of the donor tissue, the “warranty” may just run out)
How much does corneal transplant surgery cost in iran and why is the surgery different every where according to cost?
the average corneal transplant cost in iran is vary and depends on your eye surgeon and your eye hospital in iran According to the Agency for Healthcare Research and Quality , a corneal transplant costs in iran starts from $1400 .
Is it possible to help someone who is completely blind?
People who are completely blind and cannot see light cannot benefit from any type of corneal transplantation
I have diabetes, does it prevent someone from being a eye donor?
is there any possibilities for rejection of corneal transplant iran?
Rejection is unusual after corneal transplantation surgery in iran because the cornea usually does not have blood vessels. Without blood vessels the body’s immune system is less likely to recognise and reject the “foreign” graft. … Corneal grafts in such cases are at risk of rejection but steps can be taken to reduce this risk
I have heard that success rate of corneal surgery is 50-50,What is the success rate of a corneal transplant?
it is 90% .the overall success rate of a corneal transplant is very high utilizing modern eye banking and surgical techniques. However, there are many factors influencing the final result. For example, keratoconus is one of the best prognoses for good vision with more than 90% chance of a clear graft.
What Happens During Cross-Linking (CCL)?
CXL is one of the surgeries performed without the admission and supervision of an ophthalmologist with the presence of a senior eye nurse. While the operation lasts only 30 minutes, the patient should be present at the hospital a couple of hours before procedure. After the operation, the patient must stay in the center for a while in order to fully evaluate the condition. After ensuring the stability of the situation, the patient is discharged. This way, the entire duration before, during, and after the operation can lasts about half a day. Thus, you should be prepared to spend this amount of time in the hospital.
You will be asked to lie down gently on the bed. A local anesthetic drip is inserted into the eye to make the surface of the eye numb. And then a small clamp fixes the eyelid and keeps the eye open. The superficial layer of the eye (epithelium) is completely cleaned and the riboflavin drops are drip into the eye every 10 minutes. Now everything is ready for the UV light to shine for 8 minutes. After finishing, a soft dressing lens is put on the eye.
How successful is corneal transplant?
The corneal transplant operation is more successful than other transplants and is unlikely to be reversed. In cases where things are going well, the likelihood of a return is estimated at 10 to 20 percent. Also, the patient’s expectation of postoperative vision should be reasonable and should not be thought of as complete vision after surgery.