Lobectomy surgery
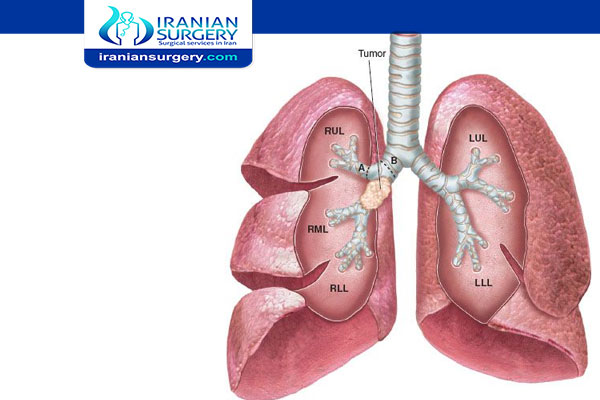
Lobectomy
What is a Lobectomy?
A lobectomy is the surgical removal of a lobe of an organ. It most often refers to the removal of a section of the lung, but it can also refer the liver, brain, thyroid gland, or other organs.
Every organ is made up of many sections that perform different, specific tasks. In the case of the lungs, the sections are called lobes. The right lung has three lobes, which are the upper, middle, and lower lobes. The left lung has two lobes, the upper and lower lobes.
In most cases, surgeons perform a lobectomy to remove a cancerous portion of an organ and to prevent the cancer from spreading. This may not entirely get rid of the disease, but it can eliminate the primary source of it.
A lobectomy is the most common way to treat lung cancer.
Surgeons may also perform lobectomies to treat:
. Fungal infections
. Benign tumors
. Emphysema
. Lung abscesses
. Tuberculosis
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best surgeons in Iran. The price of lobectomy in Iran can vary according to each individual’s case and will be determined by an in-person assessment with the doctor.
For more information about the cost of lobectomy in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number 0098 901 929 0946. This service is completely free.
Before lobectomy
Purpose of a Lobectomy
A lobectomy is done to remove a diseased or damaged portion of the lung, most often due to lung cancer. Specifically, lobectomy is most commonly performed for non-small cell lung cancers (NSCLC) in which the tumor is confined to a single lobe.
This procedure is less invasive and conserves more lung function that a pneumonectomy, a surgery that involves removing an entire lung. In contrast, it is somewhat more extensive than a wedge resection, a surgery that removes the tumor and a small amount of surrounding tissue.
What are the risks of a lobectomy?
The risks of a lobectomy include:
. An infection
. Bleeding
. An empyema, which is a collection of pus in the chest cavity
. A bronchopleural fistula, which is a tube-like track that causes air or fluid to leak out at the surgical site
. A tension pneumothorax occurs when air gets trapped between the lung and chest wall
A tension pneumothorax can potentially cause the lungs to collapse.
Specific medical conditions may lead to complications if you have a lobectomy. Discuss the risks with your doctor before any surgical procedure.
What are the benefits of a lobectomy?
Having a lobectomy can stop or slow the spread of cancer, infections, and diseases. Performing this surgery may also allow your doctor to remove a portion of an organ that affects the function of other organs. For example, a benign tumor may not be cancerous but may press against blood vessels, preventing adequate blood flow to other parts of the body. By removing the lobe with the tumor, your surgeon can effectively solve the problem.
How should you prepare for a lobectomy?
You’ll need to fast for at least eight hours before a lobectomy. This usually means not eating or drinking after midnight. Smokers need to stop smoking before having this surgery. This will improve your chance of a successful recovery.
Most people will receive a sedative before the surgery to help them relax. You may also receive antibiotics, and any other preparatory measures your doctor recommends.
During lobectomy
Types of Lobectomy
A lobe of your lung can be removed using a few different methods.
. Open Lobectomy
A lobe of the lungs is removed through a long incision on the side of the chest (thoracotomy). This involves spreading the ribs apart to get access to the lungs.
This type of surgery is usually performed if your healthcare provider needs to remove larger stage 2 and stage 3 tumors from the lungs and lymph nodes.
. Video-Assisted Thoracoscopic Surgery (VATS)
A lobe of the lung is removed through a few small incisions in the chest with the assistance of instruments and a camera.
This procedure is becoming the preferred technique. A VATS lobectomy may be considered for stage 1 or stage 2 non-small cell lung cancer (NSCLC).
When a VATS lobectomy is possible, it may result in fewer complications than an open lobectomy.
. Robot-Assisted Thoracoscopic Surgery (RATS)
Similar to VATS but performed with robots, RATS also appears to result in fewer complications and shorter hospitalizations after a lobectomy. It has been used successfully with stage 3 NSCLC, but controversy remains over whether it provides a better outcome.
What happens during the surgery?
During the Procedure
A lobectomy is performed in the operating room under a general anesthetic, so you will sleep through the procedure. You may be given antibiotics intravenously before or after the surgery.
You will be placed on a ventilator with a breathing tube inserted into your throat, and a catheter may be placed to drain urine during and after the procedure.
Your heart rate, blood pressure, and breathing will be monitored throughout the operation.
. If you are undergoing an open lobectomy, an incision will be made on the side of the body where the tissue is being removed. The cut will likely start at the front of the chest around the nipple and wrap around your back to the area under the shoulder blade.
An instrument will be used to spread the ribs apart. The healthcare provider will remove the tissue and close up the incision with stitches or staples.
. If you are undergoing a VATS or RATS procedure, three or four small cuts will be made around the area of the lobe. A thoracoscope, a small tube with a light and a tiny camera, can then be inserted into the chest cavity. It sends images to a computer screen to help the surgeon visualize the area.
Surgical instruments are then inserted through the other incisions and used to remove the problematic tissue.
After either surgery, a chest tube will be placed into the surgical area to allow excess fluid and air to drain outside of the chest for a period of time. The surgeon will close the incision(s) with stitches or staples.
After lobectomy
What to expect after a lobectomy
After surgery, you’ll be taught deep breathing and coughing exercises so your lungs can learn to expand and contract again. This will also improve your breathing and help to prevent pneumonia and other infections. Moving around and getting out of bed will help you heal faster. Slowly increase your physical activity and avoid lifting heavy objects for a while.
Be sure to avoid the following while healing:
. Tobacco smoke
. Chemical fumes and harmful vapors in the air
. Environmental pollution
. Exposure to people with upper respiratory infections, such as colds and the flu
Be sure to tell your doctor if you have any of the following side effects after surgery:
. Shortness of breath
. Trouble breathing
. Pain when breathing
. Redness, swelling, or pain around the incision
. A high fever
. Any changes in your mental state
What is the outlook?
For some people, having a lobectomy eliminates the medical problem, and for others, it slows their disease’s progression or eases symptoms. If you have lung cancer, the cancer may go into remission after a lobectomy or you may need other treatments to destroy remaining cancer cells. Other conditions may require additional medical attention.
Most people spend two to seven days in the hospital after a lobectomy, but how long you’re in the hospital will depend on a number of factors including the type of surgery you’ve had. Some people can go back to work or resume other activities shortly after that, but most people need to stay home for four to six weeks until they’ve fully recovered. You should avoid heavy lifting for six to twelve weeks after surgery or until your doctor determines you’re well enough.
After the surgery, your doctor will recommend a diet and regimen of physical activity to help you heal. You’ll likely have a follow-up appointment a week after the lobectomy. During that appointment, your doctor will check the incisions and they may take an X-ray to make sure you’re healing properly. If everything goes well, you can expect to have a full recovery in less than three months.
Sources:
. https://www.healthline.com/health/lobectomy
. https://www.verywellhealth.com/lobectomy-as-a-treatment-for-lung-cancer-2249328


3 Comments
Four years ago I experienced a severe breathing and wheezing problem that my doctor diagnosed as chronic bronchitis with dust allergy. A year later, it worsened and I was diagnosed of COPD.
I came across Herbal HealthPoint (ww w. herbalhealthpoint. c om) December, 2018 and learnt about their successful herbal therapy for COPD. I immediately started on the COPD treatment; few weeks into the treatment, i began to notice a reduction in symptoms till it all vanished. I feel better and breath better. I Just wanted to share for people suffering from this horrible lungs disease.
thx for your comment.
Hello iranian surgery
I was diagnosed of Chronic Obstructive Pulmonary Disease (COPD) in 2012 at the age of 63. I had been a heavy smoker, my symptoms started out with dry cough and shortness of breath, i ended up in the hospital, on a ventilator. I should have known it was coming, but like most smokers, thought it would never happen to me. My COPD got significantly worse and unbearable because of my difficulty catching breath. Last year, i started on a natural COPD Herbal therapy from Rich Herbal Gardens, i read a lot of positive reviews from patients who used the treatment and i immediately started on it. I had great relief with this herbal treatment. I breath very much better now, no case of shortness of breath or chest tightness since treatment. This COPD treatment is a miracle, I feel better and breath better!!