Vasectomy Reversal
Vasectomy Reversal
What is a Vasectomy Reversal?
A vasectomy reversal (vasovasostomy) is a surgical procedure that reverses the results of a vasectomy.
A vasectomy is an operation in men and people assigned male at birth (AMAB) to prevent pregnancy. It involves blocking the tubes (vas deferens) through which your sperm cells pass into your semen. Sperm cells are reproductive cells in men and people AMAB. During a vasectomy, your healthcare provider cuts and blocks (occludes) your vas deferens.
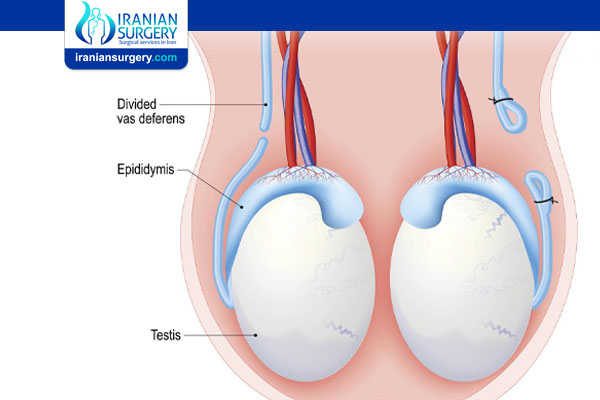
In a vasectomy reversal, your healthcare provider will remove scar tissue from both ends of your vas deferens. They’ll then align the two ends of the tube and sew them together. In some cases, this isn’t possible and your healthcare provider will sew the vas deferens to another structure called the epididymis.
Before Vasectomy Reversal
Why is a vasectomy reversal done?
If you’ve had a vasectomy, you may wish to reverse the procedure for many reasons, including:
. You changed your mind. You may want biological children after an initial decision not to have any children or not to have more children.
. You’re in a new relationship. You may remarry after a divorce or the loss of your wife or partner and wish to start a family.
. You want to restore fertility. Even if you don’t plan on having more biological children, you may feel more comfortable knowing you’re capable of having children.
. Pain relief. For a small number of people, a vasectomy causes pain in your testicles. A vasectomy reversal may relieve testicular pain.
What is the success rate of reversing a vasectomy?
Depending on how many years have passed since your vasectomy, your success rates are 60% to 95% for return of sperm in your ejaculate. Pregnancy is possible more than 50% of the time after a reversal. However, success rates start to decline 15 years after a vasectomy.
Other factors contribute to pregnancy chances even if your vasectomy reversal is successful. The age of your wife or partner is important as well as the health of your sperm.
Risks / Benefits
What are the advantages of a vasectomy reversal?
The most important advantage of a vasectomy reversal is that your chances of getting pregnant through sexual intercourse increase.
Other advantages to a vasectomy reversal include:
. Familiar recovery. Recovery after a vasectomy reversal is similar to recovery after a vasectomy.
. Permanence. You won’t need additional surgeries to increase fertility after a successful vasectomy reversal.
. Safety. A vasectomy reversal is a relatively safe procedure with a low risk of complications or side effects. Most people return home the same day of the procedure.
. Cost. A vasectomy reversal is usually more affordable than other fertility treatments, including in vitro fertilization (IVF).
What are the risks or complications of a vasectomy reversal?
Vasectomy reversals may not be successful if you have other conditions that affect your testicles. You may also develop blockages after surgery that prevent fertility. Talk to your healthcare provider if you’re still having difficulty conceiving a child after a vasectomy reversal. You may need a second vasectomy reversal or another type of surgery to collect sperm from the testicle.
All surgical procedures carry some risk. Some risks of a vasectomy reversal include:
. Anesthesia risk.
. Healing problems.
. Infection.
. Mass of clotted blood (hematoma).
. Swelling.
. Bruising.
. Unfavorable scarring.
. Pain.
What happens before a vasectomy reversal?
Before a vasectomy reversal, you should talk to your healthcare provider about the procedure. Your healthcare provider may ask you the following questions:
. Why do you want a vasectomy reversal?
. Do you have a history of excessive bleeding or blood disorders?
. Do you have any allergies to local anesthetics or antibiotics?
. Have you had any injuries or other surgeries (including hernias) on your groin, including your genitals or scrotum?
Your healthcare provider will evaluate your general health, including any pre-existing health conditions or risk factors. Tell them about any prescription or over-the-counter (OTC) medications that you’re taking, including herbal supplements. Aspirin, anti-inflammatory drugs and certain herbal supplements can increase your risk of bleeding.
How should I prepare for a vasectomy reversal?
Your healthcare provider may ask you to shave the hair from your entire scrotum or groin area the night before or the morning of your procedure.
Don’t use an electric razor on your scrotum. You should only use electric razors to shave your facial hair. They may cause cuts or irritation on your scrotum. A single-blade disposable razor is the best choice.
To reduce the risk of infection, thoroughly wash your scrotum and groin the day before and the morning of your vasectomy reversal.
During Vasectomy Reversal
Procedure Details
What happens during a vasectomy reversal?
Your healthcare provider will give you anesthesia so you won’t feel any pain. They may give you general anesthesia, which makes you go to sleep for the duration of the procedure. If they don’t give you general anesthesia, they’ll give you local anesthesia. Local anesthesia doesn’t make you go to sleep but numbs a small area of your body.
Once you’re asleep or numb, your healthcare provider will make a small incision (cut) in your scrotum, often in the same place as your vasectomy scar.
Your healthcare provider will locate the ends of your vas deferens and identify the blocked areas or the vasectomy site.
Then, they’ll pull both ends of your vas deferens out through the incision and remove the scar tissue or blockages, leaving two cut ends of your vas deferens. They will look at the fluid coming from the testicle to make sure sperm is present. If so, they’ll line up the two cut ends of your vas deferens and sew them together under a microscope. If there is no sperm present, they may need to do a more complicated operation where the vas deferens is attached to the epididymis (a structure on top of the testicle that stores sperm). Once either of these repairs is done, they’ll close the incision with stitches.
How long does a vasectomy reversal take?
A vasectomy reversal may take up to four hours. Most vasectomy reversals are outpatient procedures, so you can go home the same day you have your surgery.
What is a vasoepididymostomy?
A vasoepididymostomy is another type of vasectomy reversal.
In some cases, blockages occur in other sperm tubes (pathways) in your body. Your healthcare provider may discover these blockages while performing your vasectomy reversal. Your healthcare provider must avoid (bypass) the blockage to restore your fertility.
Blockages often occur in your epididymis (ep-uh-did-uh-miss). Your epididymis is a narrow, coiled tube that connects to your testicles. As years go by after your vasectomy, you’re more likely to develop this blockage in your epididymis.
After a vasectomy, your testicles still make sperm cells, but your body absorbs them. Over time, your testicles may produce more sperm than your body can absorb, creating pressure in your vas deferens and epididymis. This pressure may cause a tear (rupture), which your healthcare provider may only discover during surgery.
Your healthcare provider will perform a vasoepididymostomy to bypass the blockage. It’s sometimes a more challenging procedure than a standard vasectomy reversal, but it’ll increase the likelihood of fertility.
After Vasectomy Reversal
Recovery and Outlook
What happens after a vasectomy reversal?
After your vasectomy reversal is complete, your healthcare provider will cover your stitches with bandages. They’ll stop putting anesthesia into your body to keep you asleep.
Healthcare providers will move you to a recovery room, where they’ll wait for you to wake up and monitor your overall health.
Once your healthcare providers determine that you no longer need monitoring, they’ll let you go home (discharge you).
You should apply ice packs to the area intermittently for at least 24 hours after a vasectomy reversal.
OTC nonsteroidal anti-inflammatory drugs (NSAIDs) help provide relief for mild pain. The most common NSAIDs include aspirin (Bayer®), ibuprofen (Advil®) and naproxen (Aleve®). Not everyone can take NSAIDs, so it’s a good idea to check with your provider before use. If you have a lot of pain, your surgeon may prescribe a stronger pain reliever.
What is the recovery time after a vasectomy reversal?
Most people can resume normal activities about two days after a vasectomy reversal. It’s a good idea to wear an athletic supporter for at least one week.
Avoid strenuous activities for at least one week and sexual activity — including masturbation — for two to three weeks after the procedure. You may have potentially serious complications if you don’t take time to recover fully. Complications may include ripping your stitches, infection and increased pain.
Showering is OK, but you should avoid bathing until your affected area has healed. Keep the area as clean and dry as possible to help prevent infections.
It’s important to remember that your body is unique, so recovery times vary. Follow your healthcare provider’s instructions on managing any pain and discomfort.
When can I go back to work or school?
Your affected areas need time to heal. It’s a good idea to take between five and seven days off work or school.
If you have a physically demanding job, you may need up to two weeks to recover before returning to work.
What results can I expect from a vasectomy reversal?
Vasectomy reversals are generally more successful the sooner they occur after a vasectomy. Success rates often decline over time.
Your success rate for a vasectomy reversal depends on several factors, including the experience of your healthcare provider, your partner’s age and the location of your blockages.
Sperm cells should appear in your semen within a few weeks after a vasectomy reversal. If you have a vasoepididymostomy, it’ll take longer — up to 15 months — for sperm to appear in your semen.
What can I expect if I have a vasectomy reversal because of pain after a vasectomy?
Pain goes away in more than 80% of people who have a successful vasectomy reversal because of pain after a vasectomy.
When to Call the Doctor
When should I see my healthcare provider?
Schedule a follow-up appointment with your healthcare provider. They’ll want to check your incision and take your stitches out after about a week.
You should then schedule a semen analysis six to eight weeks after your vasectomy reversal. Your healthcare provider will examine your semen sample under a microscope to evaluate your sperm count, sperm activity (motility) and the shape of your sperm (morphology). It’s best to collect a semen sample between 48 and 72 hours after your last sexual activity (masturbation or intercourse) to have the greatest sperm cell level.
Source:
. https://my.clevelandclinic.org/health/treatments/15459-vasectomy-reversal