Femoral Hernia vs. Inguinal Hernia
What is the difference between an inguinal hernia and a femoral hernia?
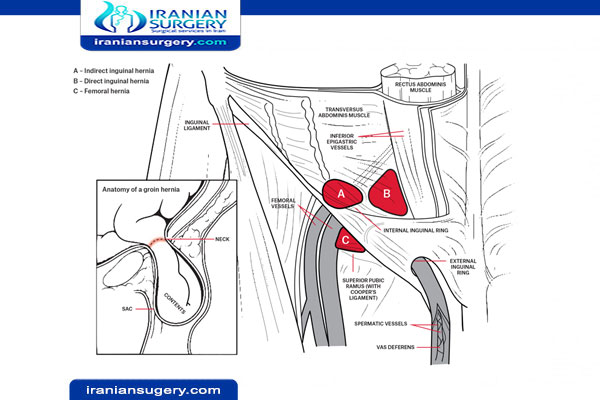
Although a femoral and inguinal hernia both develop in the groin area. An inguinal hernia involves a portion of intestine bulging into or through the inguinal canal. A femoral hernia involves a portion of intestine bulging through the femoral canal, which houses the femoral artery as it runs from the abdomen to the groin and upper thigh. Femoral hernias have a higher risk of incarceration due to the narrowness of the femoral canal. Femoral hernias are also more common in women than men.
What is a femoral hernia?
Your muscles are usually strong enough to keep your intestines and organs in their proper place. Sometimes, however, your intra-abdominal tissues can be pushed through a weakened spot in your muscle when you overstrain. If a portion of tissue pushes through the wall of the femoral canal, it’s called a femoral hernia. A femoral hernia will appear as a bulge near the groin or thigh. The femoral canal houses the femoral artery, smaller veins, and nerves. It’s located just below the inguinal ligament in the groin. A femoral hernia can also be called a femorocele.
Women are more likely than men to suffer from a femoral hernia. Overall, femoral hernias are not common. Most hernias that affect the groin are inguinal hernias, and fewer than 3 percent of all hernias are femoral. Most femoral hernias do not cause symptoms. However, they can occasionally lead to severe problems if the hernia obstructs and blocks blood flow to your intestines. This is called a strangulated hernia — it’s a medical emergency and requires immediate surgery.
Read more about : How to burst a bartholin cyst at home?
Read more about : Does urine kill sperm in male urethra?
What is an inguinal hernia?
An inguinal hernia occurs in the abdomen near the groin area. They develop when fatty or intestinal tissues push through a weakness in the abdominal wall near the right or left inguinal canal. Each inguinal canal resides at the base of the abdomen.
Both men and woman have inguinal canals. In men, the testes usually descend through their canal by around a few weeks before birth. In women, each canal is the location of passage for the round ligament of the uterus. If you have a hernia in or near this passageway, it results in a protruding bulge. It may be painful during movement.
Many people don’t seek treatment for this type of hernia because it may be small or not cause any symptoms. Prompt medical treatment can help prevent further protrusion and discomfort.
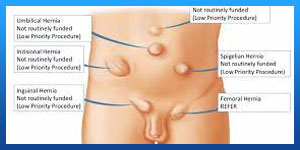
Causes
Causes of femoral hernia
The exact cause of femoral and other hernias are unknown most of the time. You may be born with a weakened area of the femoral canal, or the area may become weak over time.
Straining can contribute to the weakening of the muscle walls. Factors that can lead to overstraining include:
. Childbirth
. Chronic constipation
. Heavy lifting
. Being overweight
. Difficult urination due to an enlarged prostate
. Chronic coughing
Read more about : Ovarian cyst size chart in mm
Read more about : Femoral hernia pain down leg
Causes of inguinal hernia
There isn’t one cause for this type of hernia. However, weak spots within the abdominal and groin muscles are thought to be a major contributor. Extra pressure on this area of the body can eventually cause a hernia.
Some risk factors can increase your chances of this condition. These include:
. Heredity
. Having a prior inguinal hernia
. Being male
. Premature birth
. Being overweight or obese
. Pregnancy
. Cystic fibrosis
. Chronic cough
. Chronic constipation
Read more about : What is Lactate Dehydrogenase (LDH)?
Signs and Symptoms
Signs and symptoms of a femoral hernia
. A bulge in the upper thigh next to the groin
. Most femoral hernias cause no symptoms. Groin discomfort may worsen when standing, lifting heavy objects, or straining.
. In severe cases, abdominal pain, nausea, and vomiting
Signs and Symptoms of a inguinal hernia
Inguinal hernias are most noticeable by their appearance. They cause bulges along the pubic or groin area that can appear to increase in size when you stand up or cough. This type of hernia may be painful or sensitive to the touch.
Other symptoms may include:
. Pain when coughing, exercising, or bending over
. Burning sensations
. Sharp pain
. A heavy or full sensation in the groin
. Swelling of the scrotum in men
Diagnosis
Diagnosing a femoral hernia
Your doctor will perform a physical examination by gently palpating, or touching, the area to determine if you have a femoral hernia. If the hernia is large, the bulging will most likely be felt.
Ultrasound of the abdominal and groin area can confirm the diagnosis or establish a diagnosis if suspicion of a femoral hernia is high but no bulge is evident on physical examination. Imaging technology can show the defect in the muscle wall, as well as the protruding tissue.
Diagnosing an inguinal hernia
Your doctor can usually diagnose an inguinal hernia during a physical exam. During the exam, your doctor will ask you to cough while standing so they can check the hernia when it’s most noticeable.
When it’s reducible, you or your doctor should be able to easily push an inguinal hernia back into your abdomen when you’re lying down on your back. However, if this is unsuccessful, you may have an incarcerated or strangulated inguinal hernia.
Treatment
Treatment for femoral hernias
Femoral hernias that are small and asymptomatic may not require specific treatment. Your doctor might monitor your condition to see if symptoms progress. Moderate to large femoral hernias require surgical repair, especially if they’re causing any level of discomfort.
Surgical hernia repair is performed under general anesthesia. This means you will be asleep for the procedure and unable to feel pain. Femoral hernia repair can be done as either an open or laparoscopic surgery. An open procedure requires a larger incision and a longer recovery period. Laparoscopic surgery uses three to four keyhole-sized incisions that minimize loss of blood. The type of surgery chosen depends on a few factors, including:
. The surgeon’s expertise
. The size of the hernia and any anticipated complications
. Anticipated recovery time
. Cost
Laparoscopic surgery, for instance, involves less pain and scarring than open surgery, as well as a shorter time required for healing. However, it’s a more expensive procedure than open surgery.
In both surgeries, your surgeon will make incisions in your groin area to access the hernia. The intestine or other tissue protruding from the femoral area is returned to its proper position. The surgeon will sew the hole back together and may reinforce it with a piece of mesh. The mesh strengthens the wall of the canal. Some procedures called “tension-free repairs” are minimally invasive and don’t require the use of general anesthesia.
Treatment for inguinal hernias
Surgery is the primary treatment for inguinal hernias. It’s a very common operation and a highly successful procedure when done by a well-trained surgeon.
Options include either an open inguinal herniorrhaphy or laparoscopic inguinal herniorrhaphy. In open inguinal herniorrhaphy, one larger incision is made over the abdomen near the groin. In laparoscopic inguinal herniorrhaphy, multiple smaller abdominal incisions are made. A long, thin tube with a lighted camera on the end helps the surgeon see inside your body to perform the surgery.
The goal of either surgical approach is returning the internal abdominal tissue(s) back into the abdominal cavity and repairing the abdominal wall defect. Mesh is commonly placed to reinforce the abdominal wall. Once structures are put into their proper place, your surgeon will close the opening with sutures, staples, or adhesive glue.
There are potential pros and cons to open inguinal hernia repair versus laparoscopic. For instance, laparoscopic herniorrhaphy may be preferable if you want a shorter recovery time. But your risk of hernia recurrence may be greater with laparoscopic repair.
Risks and Complications
What are the risks of inguinal hernia surgery?
Surgery to repair an inguinal hernia is quite safe. However, possible complications of hernia surgery include:
. Urinary retention
. Infection
. Swelling in the area you had surgery due to a buildup of blood, called a hematoma, or a buildup of blood plasma, called a seroma
. Chronic or severe pain
. Return of the hernia, which may require another surgery
. Serious complications, such as damage to blood vessels or organs, are rare.
Talk with your doctor about the risks of hernia surgery and symptoms you should watch for after surgery. For example, you should call your doctor right away if you have
. Bleeding, drainage, or redness in the area where you had surgery
. Fever or chills
. Nausea or vomiting
. Pain or swelling in your abdomen
. Pain or swelling in your groin that gets worse
. Pain that is severe or doesn’t get better when you take pain medicines
. Problems breathing
. Problems urinating
What are the risks of femoral hernia surgery?
Femoral hernia repair is a routine operation with very few risks, although in a small number of cases, the hernia returns after the operation.
Other uncommon complications of femoral hernia repair include:
. Developing a lump under the wound
. Difficulty passing urine
. Injury or narrowing of the femoral vein (which passes through the femoral canal)
. Injury to the bowel
. Temporary weakness of the leg
. Injury to the nerves, causing pain or numbness in the groin area
Complications are more likely in older people or those with other conditions.