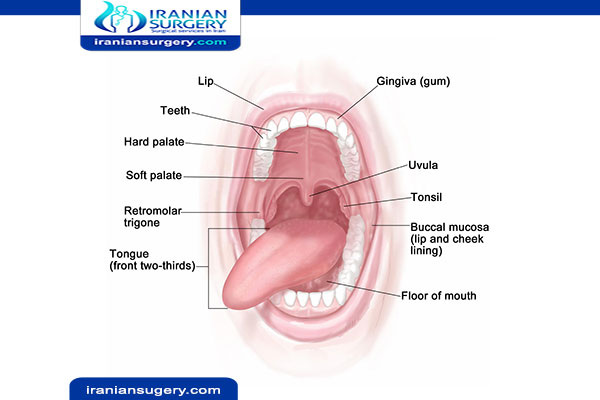
What is Oral Cancer?
Oral cancer is cancer that develops in the tissues of the mouth or throat. It belongs to a larger group of cancers called head and neck cancers.
Oral cancer is divided into two categories – those occurring in the oral cavity (your lips, the inside of your lips and cheeks, teeth, gums, the front two-thirds of your tongue and the floor and roof of your mouth) and those occurring in the oropharynx (middle region of the throat, including the tonsils and base of the tongue).
Read more about : Oral Cancer Screening
Before Oral Cancer Treatment
Where Can Oral Cancer Appear?
The oral cavity includes your lips, cheek lining, gums, front part of your tongue, floor of the mouth beneath the tongue and the hard palate that makes up the roof of your mouth. The throat (pharynx) starts at the soft part of the roof of your mouth and continues back into your throat. It includes the back section of your tongue, as well as the base where the tongue attaches to the floor of your mouth.
Read more about : Skin cancer treatment
Oral Cancer Symptoms
Symptoms of oral cancer include:
. Swellings/thickenings, lumps or bumps, rough spots/crusts/or eroded areas on the lips, gums, or other areas inside the mouth.
. The development of velvety white, red, or speckled (white and red) patches in the mouth.
. Unexplained bleeding in the mouth
. Unexplained numbness, loss of feeling, or pain/tenderness in any area of the face, mouth, or neck.
. Persistent sores on the face, neck, or mouth that bleed easily and do not heal within 2 weeks.
. A soreness or feeling that something is caught in the back of the throat
. Difficulty chewing or swallowing, speaking, or moving the jaw or tongue
. Hoarseness, chronic sore throat, or change in voice
. Dramatic weight loss
. Ear pain
. A change in the way your teeth or dentures fit together
Risk factors
One of the biggest risk factors for oral cancer is tobacco use. This includes smoking cigarettes, cigars, and pipes, as well as chewing tobacco.
People who consume large amounts of alcohol and tobacco are at an even greater risk, especially when both products are used on a regular basis.
Other risk factors include:
. Human papillomavirus (HPV) infection
. Chronic facial sun exposure
. A previous diagnosis of oral cancer
. A family history of oral or other types of cancer
. A weakened immune system
. Poor nutrition
. Genetic syndromes
. Being male
Men are twice as likely to get oral cancer as women are.
Read more about : Brain cancer treatment
Oral cancer Diagnosis
How is oral cancer diagnosed?
First, your doctor or dentist will perform a physical exam. This includes closely examining the roof and floor of your mouth, the back of your throat, tongue, and cheeks, and the lymph nodes in your neck. If your doctor cannot determine why you’re having your symptoms, you may be referred to an ear, nose, and throat (ENT) specialist.
If your doctor finds any tumors, growths, or suspicious lesions, they’ll perform a brush biopsy or a tissue biopsy. A brush biopsy is a painless test that collects cells from the tumor by brushing them onto a slide. A tissue biopsy involves removing a piece of the tissue so it can be examined under a microscope for cancerous cells.
In addition, your doctor may perform one or more of the following tests:
. X-rays to see if cancer cells have spread to the jaw, chest, or lungs
. A CT scan to reveal any tumors in your mouth, throat, neck, lungs, or elsewhere in your body.
. A PET scan to determine if the cancer has traveled to lymph nodes or other organs.
. A MRI scan to show a more accurate image of the head and neck, and determine the extent or stage of the cancer.
. An endoscopy to examine the nasal passages, sinuses, inner throat, windpipe, and trachea.
Oral Cancer Screening
Oral cancer screening is an examination performed by a dentist or doctor to look for signs of cancer or precancerous conditions in your mouth.
The goal of oral cancer screening is to identify mouth cancer early, when there is a greater chance for a cure.
Most dentists perform an examination of your mouth during a routine dental visit to screen for oral cancer. Some dentists may use additional tests to aid in identifying areas of abnormal cells in your mouth.
Preparing for the treatment
Radiotherapy makes the teeth more sensitive and vulnerable to infection, so you'll be given a full dental examination and any necessary work will be carried out before you begin your treatment.
If you smoke or drink, stopping will increase the chances of your treatment being successful.
Your GP and specialist nurse can give you help and support if you're finding it difficult to quit smoking and give up drinking.
Read more about : Cancer Treatment
Oral Cancer Prevention
To prevent oral cancer:
. Don't smoke or use any tobacco products and drink alcohol in moderation (and refrain from binge drinking).
. Eat a well-balanced diet.
. Limit your exposure to the sun. Repeated exposure increases the risk of cancer on the lip, especially the lower lip. When in the sun, use UV-A/B-blocking sun protective lotions on your skin, as well as your lips.
You can take an active role in detecting oral cancer early, should it occur, by doing the following:
. Conduct a self-exam at least once a month. Using a bright light and a mirror, look and feel your lips and front of your gums. Tilt your head back and look at and feel the roof of your mouth. Pull your checks out to view the inside of your mouth, the lining of your cheeks, and the back gums. Pull out your tongue and look at all surfaces; examine the floor of your mouth. Look at the back of your throat. Feel for lumps or enlarged lymph nodes in both sides of your neck and under your lower jaw. Call your dentist's office immediately if you notice any changes in the appearance of your mouth or any of the signs and symptoms mentioned above.
. See your dentist on a regular schedule. Even though you may be conducting frequent self-exams, sometimes dangerous spots or sores in the mouth can be very tiny and difficult to see on your own. The American Cancer Society recommends oral cancer screening exams every 3 years for persons over age 20 and annually for those over age 40. During your next dental appointment, ask your dentist to perform an oral exam. Early detection can improve the chance of successful treatment.
During Oral Cancer Treatment
Oral Cancer Types
. Squamous cell carcinoma: More than 90 percent of cancers that occur in the oral cavity are squamous cell carcinomas. Normally, the throat and mouth are lined with so-called squamous cells, which are flat and look like fish scales on a microscopic level. Squamous cell carcinoma develops when some squamous cells mutate and become abnormal.
. Verrucous carcinoma: About 5 percent of all oral cavity tumors are verrucous carcinoma, a type of very slow-growing cancer made up of squamous cells. This type of oral cancer rarely spreads to other parts of the body, but it may invade nearby tissue.
. Minor salivary gland carcinomas: This disease includes several types of oral cancer that may develop on the minor salivary glands, which are located throughout the lining of the mouth and throat. These include adenoid cystic carcinoma, mucoepidermoid carcinoma and polymorphous low-grade adenocarcinoma.
. Lymphoma: Oral cancers that develop in lymph tissue, which is part of the immune system, are known as lymphomas. The tonsils and base of the tongue both contain lymphoid tissue.
. Benign oral cavity tumors: Several types of non-cancerous tumors and tumor-like conditions may develop in the oral cavity and oropharynx. Sometimes, these conditions may develop into cancer. For this reason, benign tumors are often surgically removed. The types of benign lesions include:
. Eosinophilic granuloma
. Fibroma
. Granular cell tumor
. Keratoacanthoma
. Leiomyoma
. Osteochondroma
. Lipoma
. Schwannoma
. Neurofibroma
. Papilloma
. Condyloma acuminatum
. Verruciform xanthoma
. Pyogenic granuloma
. Rhabdomyoma
. Odontogenic tumors (lesions that begin in tooth-forming tissues)
. Leukoplakia and erythroplakia: These non-cancerous conditions develop when certain types of abnormal cells form in the mouth or throat. When leukoplakia develops, a white area is visible, while erythroplakia is marked by a red area, which may be flat or slightly raised and often bleeds when scraped. Both conditions may be precancerous, meaning they may develop into various types of cancer. When these conditions occur, a biopsy or other test is performed to determine whether the cells are cancerous. About 25 percent of leukoplakias are either cancerous when first discovered or become precancerous. Erythroplakia is usually more serious, with about 70 percent of cases deemed to be cancerous, either at the time of diagnosis or later.
Oral cancer Stages
There are four stages of oral cancer.
. Stage 1: The tumor is 2 centimeters (cm) or smaller, and the cancer hasn’t spread to the lymph nodes.
. Stage 2: The tumor is between 2-4 cm, and cancer cells haven’t spread to the lymph nodes.
. Stage 3: The tumor is either larger than 4 cm and hasn’t spread to the lymph nodes, or is any size and has spread to one lymph node, but not to other parts of the body.
. Stage 4: Tumors are any size and the cancer cells have spread to nearby tissues, the lymph nodes, or other parts of the body.
According to the National Cancer Institute, the five-year survival rates for oral cavity and pharynx cancers are as follows:
. 83 percent, for localized cancer (that hasn’t spread)
. 64 percent, for cancer that’s spread to nearby lymph nodes
. 38 percent, for cancer that’s spread to other parts of the body
Overall, 60 percent of all people with oral cancer will survive for five years or more. The earlier the stage at diagnosis, the higher the chance of survival after treatment. In fact, the five-year overall survival rate in those with stage 1 and 2 oral cancers is typically 70 to 90 percent. This makes timely diagnosis and treatment all the more important.
Treatment
How is oral cancer treated?
Treatment for oral cancer will vary depending on the type, location, and stage of the cancer at diagnosis.
Surgery
Treatment for early stages usually involves surgery to remove the tumor and cancerous lymph nodes. In addition, other tissue around the mouth and neck may be taken out.
Radiation therapy
Radiation therapy is another option. This involves a doctor aiming radiation beams at the tumor once or twice a day, five days a week, for two to eight weeks. Treatment for advanced stages will usually involve a combination of chemotherapy and radiation therapy.
Chemotherapy
Chemotherapy is a treatment with drugs that kill cancer cells. The medicine is given to you either orally or through an intravenous (IV) line. Most people get chemotherapy on an outpatient basis, although some require hospitalization.
Targeted therapy
Targeted therapy is another form of treatment. It can be effective in both early and advanced stages of cancer. Targeted therapy drugs will bind to specific proteins on cancer cells and interfere with their growth.
Nutrition
Nutrition is also an important part of your oral cancer treatment. Many treatments make it difficult or painful to eat and swallow, and poor appetite and weight loss are common. Make sure you discuss your diet with your doctor.
Getting the advice of a nutritionist can help you plan a food menu that will be gentle on your mouth and throat, and will provide your body with the calories, vitamins, and minerals it needs to heal.
Keeping your mouth healthy
Finally, keeping your mouth healthy during cancer treatments is a crucial part of treatment. Make sure to keep your mouth moist and your teeth and gums clean.
After Oral Cancer Treatment
Recovering from oral cancer treatment
The recovery from each type of treatment will vary. Post-surgery symptoms can include pain and swelling, but removing small tumors usually has no associated long-term problems.
The removal of larger tumors could possibly affect your ability to chew, swallow, or talk as well as you did before the surgery. You might also need reconstructive surgery to rebuild the bones and tissues in your face removed during surgery.
Radiation therapy can have a negative effect on the body. Some of the side effects of radiation include:
. A sore throat or mouth
. Dry mouth and loss of salivary gland function
. Tooth decay
. Nausea and vomiting
. Sore or bleeding gums
. Skin and mouth infections
. Jaw stiffness and pain
. Problems wearing dentures
. Fatigue
. A change in your ability to taste and smell
. Changes in your skin, including dryness and burning
. Weight loss
. Thyroid changes
Chemotherapy drugs can be toxic to rapidly growing noncancerous cells. This can cause side effects such as:
. Hair loss
. Painful mouth and gums
. Bleeding in the mouth
. Severe anemia
. Weakness
. Poor appetite
. Nausea
. Vomiting
. Diarrhea
. Mouth and lip sores
. Numbness in the hands and feet
Recovering from targeted therapies is usually minimal. The side effects of this treatment can include:
. Fever
. Headache
. Vomiting
. Diarrhea
. An allergic reaction
. Skin rashes
Although these treatments do have side effects, they’re often necessary in beating the cancer. Your doctor will discuss the side effects and help you weigh the pros and cons of your treatment options.
Reconstruction and rehabilitation after oral cancer treatment
People who are diagnosed with advanced oral cancer will likely need reconstructive surgery and some rehabilitation to assist with eating and speaking during recovery.
Reconstruction can involve dental implants or grafts to repair the missing bones and tissues in the mouth or face. Artificial palates are used to replace any missing tissue or teeth.
Rehabilitation is also necessary for cases of advanced cancer. Speech therapy can be provided from the time you get out of surgery until you reach the maximum level of improvement.
Lifestyle and home remedies
. Quit using tobacco
Mouth cancers are closely linked to tobacco use, including cigarettes, cigars, pipes, chewing tobacco and snuff, among others. Not everyone who is diagnosed with mouth cancer uses tobacco. But if you do, now is the time to stop because:
Tobacco use makes treatment less effective.
Tobacco use makes it harder for your body to heal after surgery.
Tobacco use increases your risk of a cancer recurrence and of getting another cancer in the future.
Quitting smoking or chewing can be very difficult. And it's that much harder when you're trying to cope with a stressful situation, such as a cancer diagnosis and treatment. Your doctor can discuss all of your options, including medications, nicotine replacement products and counseling.
. Quit drinking alcohol
Alcohol, particularly when combined with tobacco use, greatly increases the risk of mouth cancer. If you drink alcohol, stop drinking all types of alcohol. This may help reduce your risk of a second cancer.
Outlook
The outlook for oral cancers depends on the specific type and stage of cancer at diagnosis. It also depends on your general health, your age, and your tolerance and response to treatment. Early diagnosis is critical because treating stage 1 and stage 2 cancers may be less involved and have a higher chance of successful treatment.
After treatment, your doctor will want you to get frequent checkups to make sure that you’re recovering. Your checkups will usually consist of physical exams, blood tests, X-rays, and CT scans. Make sure to follow up with your dentist or oncologist if you notice anything out of the ordinary.