Stages of Cervical Cancer
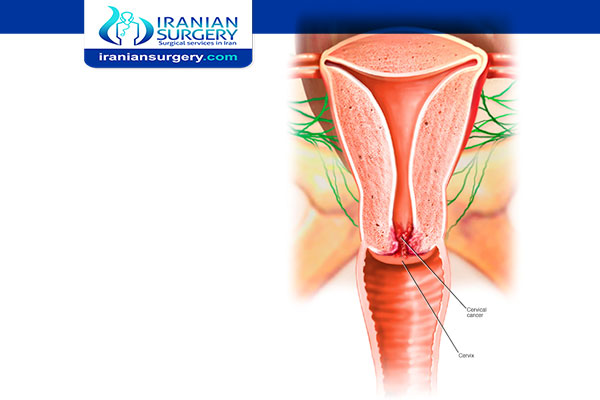
How long do you have to live if you have cervical cancer?
Staging is a way of describing where the cancer is located, if or where it has spread, and whether it is affecting other parts of the body.
Doctors use diagnostic tests to find out the cancer's stage, so staging may not be complete until all of the tests are finished. Knowing the stage helps the doctor to decide what kind of treatment is best and can help predict a patient's prognosis, which is the chance of recovery. There are different stage descriptions for different types of cancer. For cervical cancer, the staging system developed by the International Federation of Obstetrics and Gynecology (Federation Internationale de Gynecologie et d'Obstetrique, or FIGO) is used.
Read more about : Cervical cancer treatment
Read more about : Risk factors of cervical cancer
Read more about : Early symptoms of Cervical cancer
FIGO stages for cervical cancer
Doctors assign the stage of the cancer by evaluating the tumor and whether the cancer has spread to other parts of the body.
Staging is based on the results of a physical exam, imaging scans, and biopsies.
Stage I: The cancer has spread from the cervix lining into the deeper tissue but is still just found in the uterus. It has not spread to other parts of the body. This stage may be divided into smaller groups to describe the cancer in more detail (see below).
. Stage IA: The cancer is diagnosed only by viewing cervical tissue or cells under a microscope. Imaging tests or evaluation of tissue samples can also be used to determine tumor size.
. Stage IA1: There is a cancerous area of less than 3 millimeters (mm) in depth.
. Stage IA2: There is a cancerous area 3 mm to less than 5 mm in depth.
. Stage IB: In this stage, the tumor is larger but still only confined to the cervix. There is no distant spread.
. Stage IB1: The tumor 5 mm or more in depth and less than 2 centimeters (cm) wide. A centimeter is roughly equal to the width of a standard pen or pencil.
. Stage IB2: The tumor is 2 cm or more in depth and less than 4 cm wide.
. Stage IB3: The tumor is 4 cm or more in width.
Stage II: The cancer has spread beyond the uterus to nearby areas, such as the vagina or tissue near the cervix, but it is still inside the pelvic area. It has not spread to other parts of the body. This stage may be divided into smaller groups to describe the cancer in more detail (see below).
. Stage IIA: The tumor is limited to the upper two-thirds of the vagina. It has not spread to the tissue next to the cervix, which is called the parametrial area.
. Stage IIA1: The tumor is less than 4 cm wide.
. Stage IIA2: The tumor is 4 cm or more in width.
. Stage IIB: The tumor has spread to the parametrial area. The tumor does not reach the pelvic wall.
Stage III: The tumor involves the lower third of the vagina, and/or has spread to the pelvic wall, and/or causes swelling of the kidney, called hydronephrosis, or stops a kidney from functioning, and/or involves regional lymph nodes. There is no distant spread.
. Stage IIIA: The tumor involves the lower third of the vagina, but it has not grown into the pelvic wall.
. Stage IIIB: The tumor has grown into the pelvic wall and/or affects a kidney.
. Stage IIIC: The tumor involves regional lymph nodes. This can be detected using imaging tests or pathology. Adding a lowercase "r" indicates imaging tests were used to confirm lymph node involvement. A lowercase "p" indicates pathology results were used to determine the stage.
. Stage IIIC1: The cancer has spread to lymph nodes in the pelvis.
. Stage IIIC2: The cancer has spread to para-aortic lymph nodes. These lymph nodes are found in the abdomen near the base of the spine and near the aorta, a major artery that runs from the heart to the abdomen.
Stage IV
. Stage IVA: The cancer has spread to the bladder or rectum, but it has not spread to other parts of the body.
. Stage IVB: The cancer has spread to other parts of the body.
Read more about: Ovarian cyst size chart
Read more about: Ovarian Cancer Treatment
Read more about : How to burst a bartholin cyst at home?
Read more about : Colorectal cancer surgery
Read more about : Anal Cancer Treatment
Read more about : Bone cancer stage
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Surgeons to treat your cervical cancer in Iran. The price of treating a cervical cancer in Iran can vary according to each individual’s case and will be determined by the type of treatment you have and an in-person assessment with the doctor. So if you are looking for the cost of cervical cancer treatment in Iran, you can contact us and get free consultation from Iranian surgery.

Read more about: Radiation Therapy Procedure
Read more about: Chemotherapy Procedure
Read more about: Ovarian Cyst Removal Surgery
Read more about: Bartholin Cyst Surgery
Read more about: Vaginoplasty Surgery

