Virgin Tightening Surgery Before and After Pictures
How much does virgin tightening surgery cost?
How much does VAG rejuvenation cost?
virgin tightening surgery cost in Iran in best Hospital is around $2000.
If you decide to have a Vaginal Tightening Surgery in Iran, reading this article can improve your knowledge about cost of vaginoplasty in Iran to a great extent and help you to choose the best city and hospital to undergo vaginoplasty in Iran.In this article we provide you with a comprehensive description of Vaginal Tightening Surgery in Iran, the cost of vaginoplasty in Iran and the best Iranian gynecologists.
Read more about : Rhinoplasty in Iran
Read more about : BBL surgery in Iran
Read more about : Clitoromegaly surgery pictures
What is vaginal tightening surgery?
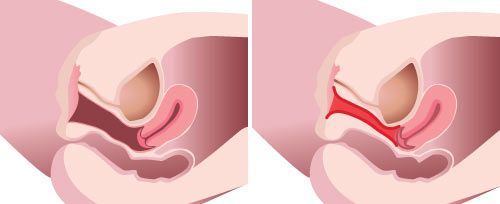
Vaginal tightening surgery, often called vaginoplasty, is a reconstructive procedure that aims to “tighten up” a vagina that has become slack.It can be undertaken to rebuild the pelvic floor when the vagina tissue and muscle has been severely stretched. Stretching typically occurs during childbirth, when the muscles of the vagina loosen and stretch during a natural delivery. you may have lost muscle tone as you’ve got older. In either case, surgery can bring back more tone, strength and control to your vaginal muscles, and may enhance sensitivity and sexual experience for you and your partner.
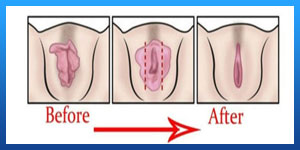
Before Vaginoplasty surgert
How should I prepare for the vaginoplasty surgery?
During your consultation your surgeon will advise you to stop smoking, drinking and/or taking aspirin or certain other medications prior to your surgery as this can affect or slow down the healing process. Your surgeon will discuss this with you at length and guide you as to when would be suggested to resume taking these.
Am I a suitable candidate for vaginoplasty surgery?
It is incredibly common for a woman to have concerns about this area as often women may find that their vaginal muscles lose tone as part of the ageing process, or after childbirth for example – this can cause much embarrassment, discomfort, the loss of sensitivity or friction experienced during sexual intercourse can also affect sexual satisfaction and cause frustration for both yourself and your partner.
What are the potential benefits of Vaginoplasty?
After Vaginoplasty, many women find it is easier to reach orgasm and experience a greater intensity of pleasure. This is often the case for their male partners too and as a result women may feel more confident in being intimate.
Risks and potential Complications
General Risks
As with any other surgical procedure, vaginoplasty techniques carry general risks, such as hemorrhage, infection, and anesthetic accidents. Severe scars may form as a result of vaginoplasty, making future corrective surgeries impossible, and also making the individual sensitive about the unsightliness of the perineum and vulva. Blood clots may form in the deep veins following surgery, called deep vein thrombosis. Surgical risks such as these are less common if the patient is in good health prior to the operation.
Specific Risks
Specific risks to vaginoplasty include vaginal fistula, uterovaginal or vault prolapse depending on whether or not the individual has a uterus, and colitis in the neovagina as well as diversion colitis in the closed-off end. Peritonitis may occur whenever the peritoneal cavity is breached.
During Vaginoplasty
The vaginoplasty operation usually takes about 1 – 2 hours. Vaginal surgery is usually performed under a general anaesthetic. In some cases an alternative using a local anaesthetic and sedation can also be performed. If you go under a general anesthesia, you may need to stay overnight in the hospital.The surgery is designed to tighten the vagina and is done by joining together the stretched muscle at the back of the vagina and therefore shortening it, using dissolvable stitches, and then removing excess vaginal lining (vaginal mucosa) and tightening the surrounding soft tissues. This procedure may also be done using a laser. The resulting decrease in the size of the vaginal cavity creates more friction during sexual intercourse, often described as giving a woman back the vagina she had before she had children. The G-spot is not affected by this procedure.
After Vaginoplasty
Recovery
Following vaginoplasty you should expect some slight bleeding for the first 24 hours and to feel sore and swollen for several days, disappearing after about 2 – 3 weeks. Bed rest is advisable post-surgery as you will not be able to walk comfortably for a few days. Depending on the extent of surgery you can expect to be off work for 7 – 10 days. Full healing takes approximately 6 weeks.You’ll have a post-op check to ensure that everything is healing properly, and your surgeon will advise when you’re able to resume sexual activity.
What should you do after Vaginal Tightening Surgery?
It is very important that you follow the advice of your surgeon carefully after vaginal tightening surgery.Post-surgery advice may include:. Using recommended painkillers as required.. Contacting your surgeon immediately if you notice any signs of infection or if you experience prolonged bleeding or a sudden increase in pain.. Avoiding baths and only taking showers for the first few days following surgery. Showering permitted 24 hours after surgery.. Avoiding vigorous exercise for 2 – 4 weeks.. Avoiding sexual intercourse (vaginal penetration) for a period of 4 to 6 weeks, depending on the type and extent of surgery.. Avoiding tight underwear such as thongs or G-strings for 1 – 2 weeks, choose loose fitting knickers.. Wearing a pad, similar to a sanitary pad for 2 – 3 days post-surgery; this acts as a surgical dressing for the collection of any blood or bodily fluids which come from the wounds.. Avoiding using tampons, only sanitary towels and panty liners are to be used in the first 4 – 6 weeks following surgery.
Vaginal Tightening Surgeons
How can I find the best Gynecologists in Iran?
Gynecologists in Iran can make your body more appealing. It is important that you seek the assistance of experienced and skilled gynecologists in Iran who have provided a suitable condition for people with limited budgets to undergo vaginoplasty in Iran easily. It is worth explaining that the quality provided by Iranian surgeons is far higher than other countries including Turkey and India.Gynecologists in Iran, have performed numerous procedures annually which make them more experienced than other countries’ plastic surgeons, due to high demand and low cost of vaginoplasty in Iran, thousands of people travel to Iran every year so that they can undergo vaginoplasty in Iran with the best gynecologists at an affordable and reasonable price.
Vaginal Tightening Surgery Cost
There are several factors that determine the overall cost of vaginoplasty, including:The surgeon’s skill: The most skilled and best Gynecologists are in high demand.Geographical location: the cost vaginoplasty is varied according to geographical location.The average cost of vaginoplasty in Iran is between $ 700-900.



22 Comments
Interested in vaginoplasty
hello Tanna, what kind of information do you need about vaginoplasty in iran? let me know please. thank you
Im looking for the best surgeon for vagainal tightening surgery.
I am from the USA and need to get vaginoplasty done? What do I have to do to get started?
hello dear laura.
at the first step, please message us in whatsapp, our female specialist connect with you.
00989019290946
Hi. I would like to have vaginal reconstructive surgery done. Where can I find a clinic please as I would like to assess cost of transport & accommodation too please. Thank you
hello dear Jenny, there are many clinics and hospitals where you can undergo vaginal reconstructive surgery in Iran. first I should know which city do you prefer to undergo your surgery, so please contact me on whatsApp to provide you with enough information. this is my whatsApp number +989019290946. thank you.
would like to get more information
hello dear Anat, please send your article we can review it and may publish it on our website. thank you
Trying to find a doctor for my Vaginoplasty in Iran I’m from the USA
hello dear Chiquita, please contact me on whatsApp to provide you with enough information regarding virgin tightening surgery in Iran. this is my whatsApp number +989019290946. thank you
Hello I’m looking for a best surgeon tighten my vigiana
hello. vaginoplasty is an important procedure as it effects daily life of the person. we would suggest Doctor Afshan shah in Tehran and Doctor Mohammadi In Shiraz are the Best and most experienced doctors in this area.
Please give me more information thanks
Hi, in desperate need of vaginoplasty. Is it 700 ,- 900 Australian dollars ? How long would it take to book this in?
hello dear holly, the cost of vaginoplasty varies city to city so we need more information to provide you with accurate information. please contact us on whatsApp number +989019290946. thank you
Can I get surgery on my tummy and muffin top as well
Hello dear,of course you can
if you are planning to have surgery in Iran,you can contact us via what’sapp:00989019290946
gmail:[email protected]
I love the improvement in my girlfriends vagina. I’m well below average endowment and this procedure has really improved our sex life.
yes. Tighter vaginal muscles can enhance sexual pleasure and restore moisture, reduce incontinence and bladder control issues, and also improve the appearance of the vagina. These benefits can greatly improve the quality of a woman’s physical, emotional, and sexual health.
Read more about : Treatment of enlarged clitorious
Dr Afshan shah
Tighter vaginal muscles pls and how much is it
Hello Sarah the Vaginoplasty operation costs around 1000 usd and it will depend on if you need fat transfer, injection or not.
if you need any more information you Can contact our Medical Team via what’s app on this number +989019290946.