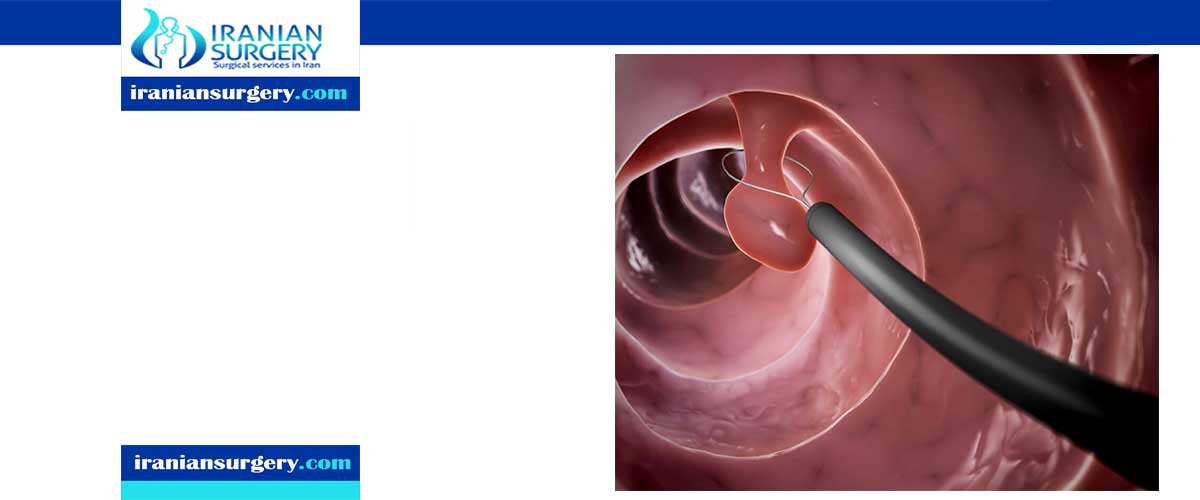
Polypectomy
What is a Polypectomy?
A polypectomy is a procedure used to remove polyps from the inside of the colon, also called the large intestine. A polyp is an abnormal collection of tissue. The procedure is relatively noninvasive and is usually carried out at the same time as a colonoscopy.
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Surgeons in Iran. The price of Polypectomy in Iran can vary according to each individual’s case and will be determined based on photos and an in-person assessment with the doctor.
For more information about the cost of Polypectomy in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number +98 901 929 0946. This service is completely free.
Before Polypectomy
What’s the purpose of a polypectomy?
Many tumors of the colon develop as a benign (noncancerous) growth before becoming malignant (cancerous).
A colonoscopy is first done to detect the presence of any polyps. If any are detected, a polypectomy is performed and the tissue is removed. The tissue will be examined to determine if the growths are cancerous, precancerous, or benign. This can prevent colon cancer.
Polyps aren’t often associated with any symptoms at all. However, larger polyps may cause:
. Rectal bleeding
. Abdominal pain
. Bowel irregularities
A polypectomy would help relieve these symptoms as well. This procedure is required any time when polyps are discovered during a colonoscopy.
How to prepare for a polypectomy
In order to perform a colonoscopy, your doctors need your large intestine to be entirely clear and free from any visual obstruction. For this reason, you’ll be asked to thoroughly empty your bowels for one or two days prior to your procedure. This might involve using laxatives, having an enema, and eating a clear food diet.
Just before the polypectomy, you’ll be seen by an anesthetist, who’ll administer anesthetic for the procedure. They’ll ask you if you’ve had any bad reactions to anesthetic before. Once you’re ready and in your hospital gown, you’ll be asked to lie on your side with your knees pulled up to your chest.
The procedure can be done relatively quickly. It usually only takes between 20 minutes to 1 hour, depending on any necessary interventions.
What are the complications and side effects?
The risks of a polypectomy can include perforation of the bowel or rectal bleeding. These risks are the same for a colonoscopy. Complications are rare, but contact your doctor immediately if you have any of the following symptoms:
. Fever or chills, as these could indicate an infection
. Heavy bleeding
. Severe pain or bloating in your abdomen
. Vomiting
. Irregular heartbeat
During Polypectomy
What’s the procedure?
A polypectomy is usually carried out at the same time as a colonoscopy. During a colonoscopy, a colonoscope will be inserted into your rectum so your doctor can see all segments of your colon. A colonoscope is a long, thin, flexible tube with a camera and a light at the end of it.
A colonoscopy is offered routinely for people who are over 50 years old to check for any growths that could be indicative of cancer. If your doctor discovers polyps during your colonoscopy, they’ll usually perform a polypectomy at the same time.
There are several ways in which a polypectomy can be performed. Which way your doctor chooses will depend on what kind of polyps are in the colon.
Polyps can be small, large, sessile, or pedunculated. Sessile polyps are flat and don’t have a stalk. Pedunculated polyps grow on stalks like mushrooms. For small polyps (less than 5 millimeters in diameter), biopsy forceps can be used for removal. Larger polyps (up to 2 centimeters in diameter) can be removed using a snare.
In snare polypectomy, your doctor will loop a thin wire around the bottom of the polyp and use heat to cut the growth off. Any remaining tissue or stalk is then cauterized.
Some polyps, due to a large size, location, or configuration, are considered more technically challenging or are associated with an increased risk of complications. In these cases, endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD) techniques can be used.
In EMR, the polyp is lifted from the underlying tissue using a fluid injection before resection is performed. This fluid injection is often made of saline. The polyp is removed one piece at a time, called piecemeal resection. In ESD, fluid is injected deep in the lesion and the polyp is removed in one piece.
For some larger polyps that can’t be removed endoscopically, bowel surgery may be needed.
Once a polyp has been removed, it’ll be sent to a pathology lab to test if the polyp is cancerous. The results usually take one week to come back, but sometimes can take longer.
After Polypectomy
How long does it take to recover?
You shouldn’t drive for 24 hours following a polypectomy.
Recovery is generally quick. Minor side effects such as gassiness, bloating, and cramps usually resolve within 24 hours. With a more involved procedure, a full recovery can take up to two weeks.
Your doctor will give you some instructions on how to care for yourself. They may ask you to avoid certain drinks and foods that can irritate your digestive system for two to three days after the procedure. These can include:
. Tea
. Coffee
. Soda
. Alcohol
. Spicy foods
Your doctor will also schedule you for a follow-up colonoscopy. It’s important to check that the polypectomy was successful and that no further polyps have developed.
What’s the outlook?
Your outlook following a polypectomy itself is good. The procedure is noninvasive, causes only mild discomfort, and you should be fully recovered in two weeks.
However, your overall outlook will be determined by what’s discovered as a result of the polypectomy. The course of any further treatment will be determined by whether or not your polyps are benign, precancerous, or cancerous.
. If they’re benign, then it’s entirely probable that no further treatment will be needed.
. If they’re precancerous, then there’s a good chance that colon cancer can be prevented.
. If they’re cancerous, colon cancer is treatable.
Cancer treatment and its success will be dependent upon many factors, including what stage the cancer is at. Your doctor will work with you to form a treatment plan.
Source:
10 common questions about Polypectomy in Iran
[kkstarratings]