Skin cancer
Skin cancer diagnosis
Skin cancer prevention
What do the early stages of skin cancer look like?
Skin cancer is a cancer that originates from the skin. They are due to the development of abnormal cells that have the ability to invade or spread to other parts of the body.
There are three major types of skin cancers: basal-cell skin cancer (BCC), squamous-cell skin cancer (SCC), and melanoma. The first two, along with a number of less common skin cancers, are known as nonmelanoma skin cancer (NMSC). Basal-cell cancer grows slowly and can damage the tissue around it but is unlikely to spread to distant areas or result in death. It often appears as a painless raised area of the skin, which may be shiny with small blood vessels running over it or may present as a raised area with an ulcer. Squamous-cell skin cancer is more likely to spread. It usually presents as a hard lump with a scaly top but may also form an ulcer. Melanomas are the most aggressive. Signs include a mole that has changed in size, shape, color, has irregular edges, has more than one color, is itchy or bleeding.
Greater than 90% of the cases are caused by exposure to ultraviolet radiation from the Sun. This exposure increases the risk of all three major types of skin cancer. Exposure has increased partially due to a thinner ozone layer. Tanning beds are becoming another common source of ultraviolet radiation. For melanoma and basal-cell cancer exposure during childhood is particularly harmful. For squamous-cell skin cancers, total exposure, irrespective of when it occurs, is more important. Between 20% and 30% of melanomas develop from moles. People with light skin are at higher risk as are those with poor immune function such as from drugs or HIV / AIDS. Diagnosis is by biopsy.
Read more about: Chemotherapy
Decreasing exposure to ultraviolet radiation and using sunscreen appear to be effective methods for preventing melanoma and squamous cell skin cancer. It is not clear if sunscreen affects the risk of basal cell cancer. Non-melanoma skin cancer is usually curable. Treatment is usually by surgical removal but may be less common in radiation therapy or topical medications such as fluorouracil. Treatment of melanoma may involve some combination of surgery, chemotherapy, radiation therapy, and targeted therapy. In those people whose disease has spread to other areas of their bodies, palliative care may be used to improve the quality of life. Melanoma has one of the highest survival rates among cancers, with over 86% of people in the UK and more than 90% in the United States surviving more than 5 years.
Skin cancer is the most common form of cancer, globally accounting for at least 40% of cases. The most common type is nonmelanoma skin cancer, which occurs in at least 2-3 million people a year. This is a rough estimate, however, as good statistics are not kept. Of nonmelanoma skin cancers, about 80% are basal cell cancers and 20% squamous cell skin cancers. Basal-cell and squamous-cell skin cancers rarely result in death.
Read more about: Cancer treatment
Read more about: Skin grafting
Skin cancer classification
There are three main types of skin cancer: basal-cell skin cancer (basal-cell carcinoma) (BCC), squamous-cell skin cancer (squamous-cell carcinoma) (SCC) and malignant melanoma.
| Cancer | Description | Illustration |
|---|---|---|
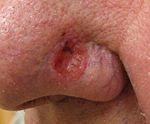
| Basal-cell carcinoma | Note the pearly translucency to fleshy color, tiny blood vessels on the surface, and sometime ulceration which can be characteristics. The key term is translucency. | |
| Squamous-cell skin carcinoma | Commonly presents as a red, crusted, or scaly patch or bump. Often a very rapid growing tumor. | |
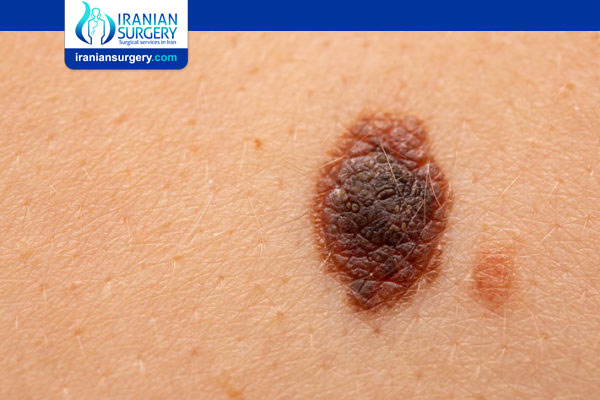
| Malignant melanoma | The common appearance is an asymmetrical area, with an irregular border, color variation, and often greater than 6 mm diameter. |
Basal-cell carcinomas are present on sun-exposed areas of the skin, especially the face. They rarely metastasize and rarely cause death. They are easily treated with surgery or radiation. Squamous-cell skin cancer are common, but much less common than basal-cell cancers. They metastasize more frequently than BCCs. Even then, the metastasis rate is quite low, with the exception of SCC of the lip, ear, and in people who are immunosuppressed. Melanoma are the least frequent of the 3 common skin cancers. They frequently metastasize, and could potentially cause death once they spread.
Less common skin cancers include: dermatofibrosarcoma protuberans, Merkel cell carcinoma, Kaposi’s sarcoma, keratoacanthoma, spindle cell tumors, sebaceous carcinomas, microcystic adnexal carcinoma, Paget’s disease of the breast, atypical fibroxanthoma, leiomyosarcoma, and angiosarcoma.
BCC and SCC often carry a UV-signature mutation indicating that these cancers are caused by UVB radiation via direct DNA damage. However malignant melanoma is predominantly caused by UVA radiation via indirect DNA damage. The indirect DNA damage is caused by free radicals and reactive oxygen species. Research indicates that the absorption of three sunscreen ingredients into the skin, combined with a 60-minute exposure to UV, leads to an increase of free radicals in the skin, if applied in too little quantities and too infrequently. However, the researchers add that newer creams often do not contain these specific compounds, and that the combination of other ingredients tends to retain the compounds on the surface of the skin. They also add the frequent re-application reduces the risk of radical formation.
Read more about : Bone cancer stage
Read more about: Skin Treatments in Iran

Signs and symptoms
There are a variety of different skin cancer symptoms. These include changes in the skin that do not heal, ulcering in the skin, discolored skin, and changes in existing moles, such as jagged edges to the mole and enlargement of the mole.
- Basal-cell skin cancer
Basal-cell skin cancer (BCC) usually presents as a raised, smooth, pearly bump on the sun-exposed skin of the head, neck or shoulders. Sometimes small blood vessels (called telangiectasia) can be seen within the tumor. Crusting and bleeding in the center of the tumor frequently develops. It is often mistaken for a sore that does not heal. This form of skin cancer is the least deadly and with proper treatment can be completely eliminated, often without scarring.
- Squamous-cell skin cancer
Squamous-cell skin cancer (SCC) is commonly a red, scaling, thickened patch on sun-exposed skin. Some are firm hard nodules and dome shaped like keratoacanthomas. Ulceration and bleeding may occur. When SCC is not treated, it may develop into a large mass. Squamous-cell is the second most common skin cancer. It is dangerous, but not nearly as dangerous as a melanoma.
- Melanoma
Most melanoma consist of various colours from shades of brown to black. A small number of melanoma are pink, red or fleshy in colour; these are called amelanotic melanoma and tend to be more aggressive. Warning signs of malignant melanoma include change in the size, shape, color or elevation of a mole. Other signs are the appearance of a new mole during adulthood or pain, itching, ulceration, redness around the site, or bleeding at the site. An often-used mnemonic is “ABCDE”, where A is for “asymmetrical”, B for “borders” (irregular: “Coast of Maine sign”), C for “color” (variegated), D for “diameter” (larger than 6 mm – the size of a pencil eraser) and E for “evolving.”
- Other
Merkel cell carcinomas are most often rapidly growing, non-tender red, purple or skin colored bumps that are not painful or itchy. They may be mistaken for a cyst or another type of cancer.
Read more about: Skin tightening in Iran
Skin cancer diagnosis
A diagnosis of non-melanoma skin cancer will usually begin with a visit to a GP, who will examine your skin and decide whether you need further assessment by a specialist.
Some GPs take digital photographs of suspected tumors so they can email them to a specialist for assessment.
- Biopsy
If skin cancer is suspected, you may be referred to a skin specialist (dermatologist) or specialist plastic surgeon. The specialist should be able to confirm the diagnosis by doing a physical examination.
However, they'll probably also do a biopsy, which is a minor surgical procedure where either part or all of the tumor is removed so it can be studied under a microscope.
This is usually done after a local anesthetic is given, which means you'll be conscious but the affected area will be numb, so you will not feel any pain.
A biopsy allows the dermatologist or plastic surgeon to determine the type of skin cancer you have and whether there's any chance of it spreading to other parts of your body.
Skin cancer can sometimes be diagnosed and treated at the same time. The tumor can be removed and tested, and you may not need further treatment because the cancer is unlikely to spread.
It's usually several weeks before you receive the results of a biopsy.
- Further tests
If you have basal cell carcinoma, further tests are not usually required as it's very unlikely that the cancer will spread.
However, you may have a second basal cell carcinoma on a different area of skin, so it makes sense to have all of your skin examined by the skin expert.
In rare cases of squamous cell carcinoma, further tests may be needed to make sure the cancer has not spread to your lymph nodes or another part of your body.
These tests may include a physical examination of your lymph nodes. If cancer has spread, it may cause your glands to swell.
If the dermatologist or plastic surgeon thinks there's a significant risk of the cancer spreading, it may be necessary to do a biopsy on a lymph node. This is called a fine-needle aspiration (FNA).
During FNA, cells are removed using a needle and syringe so they can be examined.
Finding cancerous cells in a nearby lymph node would suggest the squamous cell carcinoma has started to spread to other parts of your body.
- Staging skin cancer
Staging is used to describe how far a tumor has spread. The stage of the cancer will help determine your recommended treatment.
For non-melanoma skin cancer, this only applies to squamous cell carcinoma, as there's no staging system for basal cell carcinoma.
Read more about: Bladder Cancer Staging
Skin cancer stages
To determine a skin cancer’s stage or severity, your doctor will factor in how large the tumor is, if it has spread to your lymph nodes, and if it has spread to other parts of the body.
Skin cancers are divided into two primary groups for staging purposes: nonmelanoma skin cancer and melanoma.
Nonmelanoma skin cancers include basal cell and squamous cell cancers.
- Stage 0: The abnormal cells have not spread beyond the outermost layer of skin, the epidermis.
- Stage I: The cancer may have spread to the next layer of skin, the dermis, but it is no longer than two centimeters.
- Stage II: The tumor is larger than two centimeters, but it has not spread to nearby sites or lymph nodes.
- Stage III: The cancer has spread from the primary tumor to nearby tissue or bone, and it is larger than three centimeters.
- Stage IV: The cancer has spread beyond the primary tumor site to lymph nodes and bone or tissue. The tumor is also larger than three centimeters.
Melanoma stages include:
- Stage 0: This noninvasive type of skin cancer has not penetrated below the epidermis.
- Stage I: The cancer may have spread to the second layer of skin, the dermis, but it remains small.
- Stage II: The cancer has not spread beyond the original tumor site, but it is larger, thicker, and may have other signs or symptoms. These include scaling, bleeding, or flaking.
- Stage III: The cancer has spread or metastasized to your lymph nodes or to nearby skin or tissue.
- Stage IV: The most advanced stage of melanoma. Stage IV is an indication the cancer has spread beyond the primary tumor and is showing up in lymph nodes, organs, or tissue distant from the original site.
When cancer comes back after treatment, it’s called recurrent skin cancer. Anyone who has been diagnosed with and treated for skin cancer is at risk for a recurrence of the cancer.
Read more about: Dry skin
Skin cancer causes
Skin cancer occurs when errors (mutations) occur in the DNA of skin cells. The mutations cause the cells to grow out of control and form a mass of cancer cells.
Cells involved in skin cancer
Skin cancer begins in your skin's top layer the epidermis. The epidermis is a thin layer that provides a protective cover of skin cells that your body continually sheds. The epidermis contains three main types of cells:
- Squamous cellslie just below the outer surface and function as the skin's inner lining.
- Basal cells,which produce new skin cells, sit beneath the squamous cells.
- Melanocytes, which produce melanin, the pigment that gives skin its normal color are located in the lower part of your epidermis. Melanocytes produce more melanin when you're in the sun to help protect the deeper layers of your skin.
Where your skin cancer begins determines its type and your treatment options.
Ultraviolet light and other potential causes
Much of the damage to DNA in skin cells results from ultraviolet (UV) radiation found in sunlight and in the lights used in tanning beds. But sun exposure doesn't explain skin cancers that develop on skin not ordinarily exposed to sunlight. This indicates that other factors may contribute to your risk of skin cancer, such as being exposed to toxic substances or having a condition that weakens your immune system.
Read more about: Cervical cancer symptoms
Risk factors
Factors that may increase your risk of skin cancer include:
- Fair skin. Anyone, regardless of skin color, can get skin cancer. However, having less pigment (melanin) in your skin provides less protection from damaging UV radiation. If you have blond or red hair and light-colored eyes, and you freckle or sunburn easily, you're much more likely to develop skin cancer than is a person with darker skin.
- A history of sunburns. Having had one or more blistering sunburns as a child or teenager increases your risk of developing skin cancer as an adult. Sunburns in adulthood also are a risk factor.
- Excessive sun exposure. Anyone who spends considerable time in the sun may develop skin cancer, especially if the skin isn't protected by sunscreen or clothing. Tanning, including exposure to tanning lamps and beds, also puts you at risk. A tan is your skin's injury response to excessive UV radiation.
- Sunny or high-altitude climates. People who live in sunny, warm climates are exposed to more sunlight than are people who live in colder climates. Living at higher elevations, where the sunlight is strongest, also exposes you to more radiation.
- Moles. People who have many moles or abnormal moles called dysplastic nevi are at increased risk of skin cancer. These abnormal moles — which look irregular and are generally larger than normal moles — are more likely than others to become cancerous. If you have a history of abnormal moles, watch them regularly for changes.
- Precancerous skin lesions. Having skin lesions known as actinic keratoses can increase your risk of developing skin cancer. These precancerous skin growths typically appear as rough, scaly patches that range in color from brown to dark pink. They're most common on the face, head and hands of fair-skinned people whose skin has been sun damaged.
- A family history of skin cancer. If one of your parents or a sibling has had skin cancer, you may have an increased risk of the disease.
- A personal history of skin cancer. If you developed skin cancer once, you're at risk of developing it again.
- A weakened immune system. People with weakened immune systems have a greater risk of developing skin cancer. This includes people living with HIV/AIDS and those taking immunosuppressant drugs after an organ transplant.
- Exposure to radiation. People who received radiation treatment for skin conditions such as eczema and acne may have an increased risk of skin cancer, particularly basal cell carcinoma.
- Exposure to certain substances. Exposure to certain substances, such as arsenic, may increase your risk of skin cancer.
Skin cancer prevention
Most skin cancers are preventable. To protect yourself, follow these skin cancer prevention tips:
- Avoid the sun during the middle of the day.For many people in North America, the sun's rays are strongest between about 10 a.m. and 4 p.m. Schedule outdoor activities for other times of the day, even in winter or when the sky is cloudy.
You absorb UV radiation year-round, and clouds offer little protection from damaging rays. Avoiding the sun at its strongest helps you avoid the sunburns and suntans that cause skin damage and increase your risk of developing skin cancer. Sun exposure accumulated over time also may cause skin cancer.
- Wear sunscreen year-round.Sunscreens don't filter out all harmful UV radiation, especially the radiation that can lead to melanoma. But they play a major role in an overall sun protection program.
Use a broad-spectrum sunscreen with an SPF of at least 30, even on cloudy days. Apply sunscreen generously, and reapply every two hours — or more often if you're swimming or perspiring. Use a generous amount of sunscreen on all exposed skin, including your lips, the tips of your ears, and the backs of your hands and neck.
- Wear protective clothing.Sunscreens don't provide complete protection from UV rays. So cover your skin with dark, tightly woven clothing that covers your arms and legs, and a broad-brimmed hat, which provides more protection than a baseball cap or visor does.
Some companies also sell photoprotective clothing. A dermatologist can recommend an appropriate brand.
Don't forget sunglasses. Look for those that block both types of UV radiation UVA and UVB rays.
- Avoid tanning beds.Lights used in tanning beds emit UV rays and can increase your risk of skin cancer.
- Be aware of sun-sensitizing medications.Some common prescription and over-the-counter drugs, including antibiotics, can make your skin more sensitive to sunlight.
Ask your doctor or pharmacist about the side effects of any medications you take. If they increase your sensitivity to sunlight, take extra precautions to stay out of the sun in order to protect your skin.
- Check your skin regularly and report changes to your doctor.Examine your skin often for new skin growths or changes in existing moles, freckles, bumps and birthmarks.
With the help of mirrors, check your face, neck, ears and scalp. Examine your chest and trunk, and the tops and undersides of your arms and hands. Examine both the front and back of your legs, and your feet, including the soles and the spaces between your toes. Also check your genital area and between your buttocks.
Read more about: Does colorectal cancer occur in old people?
Treatments for skin cancer
Your recommended treatment plan will depend on different factors, like the size, location, type, and stage of your skin cancer. After considering these factors, your healthcare team may recommend one or more of the following treatments:
- Cryotherapy: The growth is frozen using liquid nitrogen and the tissue is destroyed as it thaws.
- Excisional surgery: The growth and some of the healthy skin surrounding it are cut out.
- Mohs surgery: The growth is removed layer by layer, and each layer is examined under a microscope until no abnormal cells are visible.
- Curettage and electrodessication: A long spoon-shaped blade is used to scrape away the cancer cells, and the remaining cancer cells are burned using an electric needle.
- Chemotherapy: Drugs are taken orally, applied topically, or injected with a needle or IV line to kill the cancer cells.
- Photodynamic therapy: A laser light and drugs are used to destroy the cancer cells.
- Radiation: High-powered energy beams are used to kill the cancer cells.
- Biological therapy: Biological treatments are used to stimulate your immune system to fight the cancer cells.
- Immunotherapy: A cream is applied to your skin to stimulate your immune system to kill the cancer cells.
Read more about: Loose skin after liposuction thighs
After skin cancer treatment
If you have completed treatment, your doctors will still want to watch you closely. Along with the risk of the cancer returning, people who have had skin cancer are also at high risk for developing other skin cancers in different locations, so close follow-up is important.
Your doctor will probably recommend that you examine your own skin at least once a month. This includes looking for any changes where the cancer was treated, as well as looking for any new areas of concern in other places. You can also ask someone close to you to watch for new suspicious areas in places that are hard to see.
It’s also very important to protect yourself from getting too much sun, which can increase your risk of new skin cancers.
Read more about: skin problems after bariatric surgery