Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery
Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery
If you decide to have a Biliopancreatic Diversion with Duodenal Switch Surgery in Iran, reading this article can improve your knowledge about cost of Biliopancreatic Diversion with Duodenal Switch Surgery in Iran to a great extent and help you to choose the best doctor and hospital to undergo Biliopancreatic Diversion with Duodenal Switch Surgery in Iran.
In this article we provide you with a comprehensive description of Biliopancreatic Diversion with Duodenal Switch Surgeries in Iran and the cost of Biliopancreatic Diversion with Duodenal Switch Surgery in Iran.
Read more about : Mini gastric bypass side effects
Read more about : Gastric bypass surgery cost
Read more about : Gastric Plication Surgery In Iran
General Information |
|
Cost | $ 3200 - 3700 |
Anesthesia | General |
Hospital Stay | 2-3 Days |
Back to Work | 1 to 3 Weeks |
Duration of Operation | 3-4 Hours |
Minimum Stay in Iran | 7-10 Days |
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Bariatric Surgeons in Iran. The price of a Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery in Iran can vary according to each individual’s case and will be determined based on photos and an in-person assessment with the doctor. So if you are looking for the cost of Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery in Iran, you can contact us and get free consultation from Iranian surgery.

Read more about : Gastric balloon side effects
Read more about : Skin problem after bariatric surgery
Read more about: Bariatric surgery in Iran
Read more about: Lipomatic
Read more about: Bariatric surgery diet
What is Biliopancreatic Diversion with Duodenal Switch (BPD/DS)?
The Biliopancreatic Diversion with Duodenal Switch – abbreviated as BPD/DS – is a procedure with two components. First, a smaller, tubular stomach pouch is created by removing a portion of the stomach, very similar to the sleeve gastrectomy. Next, a large portion of the small intestine is bypassed.
BPD/DS is generally performed as a single procedure however, in select circumstances, the procedure may be performed as two separate operations — sleeve gastrectomy followed by intestinal bypass once weight loss has begun.
Why it's done
Healthcare providers may recommend the BPD/DS to people who are severely obese. These people usually have a body mass index (BMI) of 50 or greater or a BMI of 40 or greater with serious type 2 diabetes and other serious health problems. These health problems include:
. Type 2 diabetes
. Sleep apnea
. Heart disease
. Lung disease
. High blood pressure
. High cholesterol
. Nonalcoholic fatty liver disease
A BPD/DS is typically done only after you've tried to lose weight by improving your diet and exercise habits.
Before Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery
How you prepare
If you qualify for a BPD/DS, your health care team gives you instructions on how to prepare for surgery. You may need to have various lab tests and exams before surgery.
Food and medications
Before your surgery, give your surgeon and any other health care providers a list of all medicines, vitamins, minerals, and herbal or dietary supplements you take. You may have restrictions on eating and drinking and which medications you can take.
If you take blood-thinning medications, talk with your doctor before your surgery. Because these medications affect clotting and bleeding, your blood-thinning medication routine may need to be changed.
If you have diabetes, talk with the doctor who manages your insulin or other diabetes medications for specific instructions on taking or adjusting them after surgery.
Other precautions
You may be required to start a physical activity program and to stop any tobacco use.
You may also need to prepare by planning ahead for your recovery after surgery. For instance, arrange for help at home if you think you'll need it.
What you can expect
BPD/DS is done in the hospital. The length of your hospital stay will depend on your recovery and which procedure you're having done. When performed laparoscopically, your hospital stay may last around two days.
Before the procedure
Before you go to the operating room, you will change into a gown and will be asked several questions by both doctors and nurses. In the operating room, you are given general anesthesia before your surgery begins. Anesthesia is medicine that keeps you asleep and comfortable during surgery.
Read more about : Gastric bypass vs duodenal switch
Read more about : Gastric sleeve vs gastric bypass
The Advantages and Disadvantages
What are the Advantages and Disadvantages of Duodenal Switch?
Advantages:
. You will lose up to 70% of your excess weight within a year
. Allows patients to eventually eat near “normal” meals
. Causes favorable changes in gut hormones to reduce appetite and improve satiety.
. Duodenal switch surgery will cure or improve your diabetes, sleep apnea, hypertension, and at least 12 other conditions.
. You will feel full sooner while eating
. Your body will absorb fewer calories from the food you eat.
Disadvantages:
. Requires a longer hospital stay than the AGB or LSG
. Has a greater potential to cause protein deficiencies and long-term deficiencies in a number of vitamin and minerals, i.e. iron, calcium, zinc, fat-soluble vitamins such as vitamin D.
. Compliance with follow-up visits and care and strict adherence to dietary and vitamin supplementation guidelines are critical to avoid serious complications from protein and certain vitamin deficiencies.
. More frequent bowel movements.
Risks and Complications:
As with any major surgery, a BPD/DS poses potential health risks, both in the short term and long term.
Risks associated with BPD/DS are similar to any abdominal surgery and can include:
. Excessive bleeding
. Infection
. Adverse reactions to anesthesia
. Blood clots
. Lung or breathing problems
. Leaks in your gastrointestinal system
Longer term risks and complications of a BPD/DS may include:
. Bowel obstruction
. Dumping syndrome, causing diarrhea, nausea or vomiting
. Gallstones
. Hernias
. Low blood sugar (hypoglycemia)
. Vitamin deficiency/ Malnutrition
. Stomach perforation
. Ulcers
. Digestion issues
. Sagging skin
. Weight Regain
Is a Duodenal Switch right for me?
You may be eligible for Duodenal Switch surgery if:
. You have a body mass index (BMI) of 40 or more, OR
. Your BMI is between 35 and 39.9 and you have a serious obesity-related health problem.
Read more about: Virgin tightening surgery before and after
Read more about: Stages of fissure healing
Read more about: Sleeve Gastrectomy Surgery
During Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery
The Procedure
How Duodenal Switch is performed
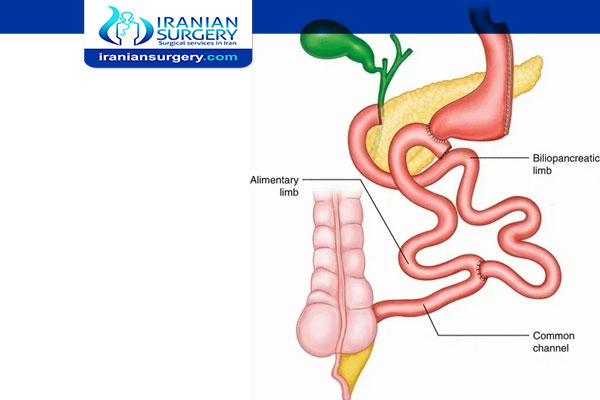
The first step is sleeve gastrectomy in which about 80 percent of the stomach is removed, leaving a smaller tube-shaped stomach, similar to a banana. However, the valve that releases food to the small intestine (the pyloric valve) remains, along with a limited portion of the small intestine that normally connects to the stomach (duodenum).
The second step bypasses the majority of the intestine by connecting the end portion of the intestine to the duodenum near the stomach. A BPD/DS both limits how much you can eat and reduces the absorption of nutrients, including proteins and fats.
The operation can take between two and three hours, but this may vary between surgeons.
Read more about: How much weight can I lose with a gastric balloon??
Read more about: How to tone up after gastric bypass?
After Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery
What happens after BPD/DS weight-loss surgery?
You will wake up in a recovery room. You will be given medicine to control pain. You will be moved to a hospital room. You will be asked to get out of bed to move around within the next day. This helps prevent blood clots in your legs. You will have liquid nutrition. Your team will tell you when you're ready to go home.
At first, you may have stomach or bowel cramping, or nausea. Tell your healthcare provider if pain or nausea is severe or doesn’t improve with time. Take pain medicines as prescribed.
Call your healthcare provider if you have any of the following:
. A fever of 100.4°F (38°C) or higher, or as directed by your healthcare provider
. A red, bleeding, or draining incision
. Frequent or persistent nausea or vomiting
. Increased pain at an incision
. Pain or swelling in your legs
. Trouble breathing or chest pain
You will get instructions about how to adapt to your new diet after your surgery. You will likely be on liquid nutrition for a few weeks after surgery. Over time, you’ll start to eat soft foods and then solid foods. If you eat too much or too fast, you will likely have stomach pain or vomiting. You’ll learn how to know when your new stomach is full.
Your healthcare provider or nutritionist will give you more instructions about your diet. You’ll need to learn good habits like choosing healthy foods and not skipping meals. Your healthcare provider or nutritionist will also need to screen you for low levels of nutrients.
You will need to take daily supplements after BPD/DS surgery. These include:
. Vitamins A, D, and K
. Multivitamin
. Iron supplements
. Calcium supplements
. Vitamin B-12 supplements or injections
Work with your healthcare team after surgery to stay healthy. Make sure to:
. Follow the nutrition plan set up by your dietitian
. Get regular physical activity. Start slowly and build up to more activity.
. Talk with a counselor or weight-loss surgery support group to help you adjust.
Recovery
. Hospital Stay: You will be in the hospital for 2 to 3 days
. Time off Work: You will need to take 1 to 3 weeks off of work
. Full Recovery: You will be “fully recovered” in 4 to 6 weeks
. Pain: The pain is manageable – it’s the same as any laparoscopic surgery and managed with medication.
. Diet & Activity: There will be a slow transition from clear liquids to solid foods and back to regular activity and exercise.
Read more about: Mini gastric bypass surgery vs gastric bypass
Read more about: High BMI for liposuction
How can I find the best Biliopancreatic Diversion with Duodenal Switch surgeon in Iran?
Bariatric surgeons in Iran can make your body more appealing. It is important that you seek the assistance of experienced and skilled Biliopancreatic Diversion with Duodenal Switch surgeons in Iran who have provided a suitable condition for people with limited budgets to undergo Biliopancreatic Diversion with Duodenal Switch in Iran easily. It is worth explaining that the quality provided by Iranian surgeons is far higher than other countries including Turkey and India.
Bariatric surgeons in Iran, have performed numerous procedures annually which make them more experienced than other countries’ plastic surgeons, due to high demand and low cost of Duodenal Switch in Iran, thousands of people travel to Iran every year to undergo Duodenal Switch in Iran with the best Bariatric surgeons at an affordable and reasonable price.
Read more about: Gastric balloon side effects
Read more about: Liposuction Surgery In Iran
Iranian Surgery is an online medical tourism platform that helps you to do Biliopancreatic Diversion with Duodenal Switch (BPD/DS) Surgery with the best bariatric surgeons in Iran at the most affordable price.
For more information and to schedule an appointment, contact our consultants via WhatsApp number +98 901 929 0946.
This service is completely free
10 Commom question about duodenal switch surgery
[kkstarratings]

