Rectal Cancer Staging Radiology
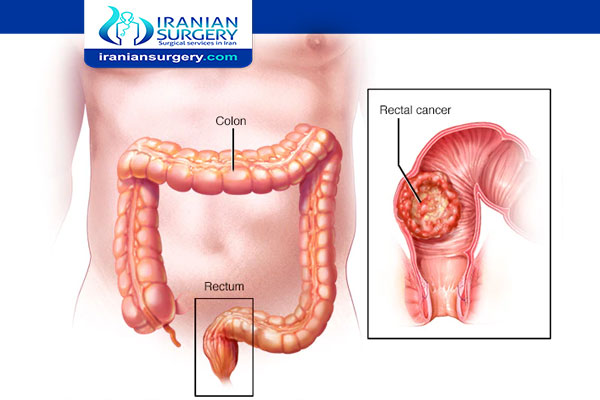
How do they determine stages of rectal cancer?
What is the survival rate of rectal cancer?
What stage is t3 rectal cancer?
How is a rectal tumor removed?
Rectal Cancer Staging Radiology
MRI is the modality of choice for rectal cancer staging. The high soft-tissue contrast of MRI accurately assesses the extramural tumor spread and relation to mesorectal fascia and the sphincter complex. This article reviews the role of MRI in the staging and treatment of rectal cancer. The relevant anatomy, MRI techniques, preoperative staging, post–chemoradiation therapy (CRT) imaging, and tumor recurrence are discussed with special attention to recent advances in knowledge.
Additional specific MRI imaging staging subsets of rectal tumor, special consideration should be given to low rectal tumors as these carry a different prognosis from higher lesions. This is predominantly due to anatomical considerations including waist-like tapering of the mesorectum
Early rectal cancer and significant polyps may also be subclassified, necessitating the use of good quality, high-resolution T2-weighted MR images. This relies on the recognition that most rectal tumors (apart from mucinous tumors) have intermediate T2 signal compared to hyperintense submucosa and hypointense muscularis layers. Such staging may be helpful in selecting less extensive surgical resection options.
Read more about : Stages of fissure healing
Read more about : Hemorrhoidectomy Surgery
Read more about : Anal Fissure Surgery
Read more about : What is colorectal cancer?
Read more about : Rectal Cancer Staging
- Low rectal tumor staging
- Stage 1: tumor confined to bowel wall with intact outer muscularis propria
- Stage 2: tumor replaces muscularis propria but does not extend into intersphincteric plane
- Stage 3: tumor invades intersphincteric plane or lies within 1 mm of levator muscles
- Stage 4: tumor invades external anal sphincter and is within 1 mm and beyond levators with or without invading adjacent organs
- Early rectal tumor staging
- T0/early T1sm1:no submucosa (sm) disruption evident with entire thickness of submucosal stripe preserved
- T1sm2:at least 1 mm of submucosa preserved
- T1sm3/early T2: less than 1 mm of submucosa preserved but full thickness of muscularis propria preserved
- T2 early:more than 1 mm muscularis propria preserved
- T2/T3a:0 mm muscularis propria preserved / less than 1 mm microscopic invasion beyond muscularis propria (prognosis identical)
- T3b:1-5 mm invasion beyond muscularis propria (still carries good prognosis)
Read more about: rectal abscess cause
Read more about: rectal cancer causes
Read more about: rectal cancer prognosis
How do they determine stages of rectal cancer?
After someone is diagnosed with colorectal cancer, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer's stage when talking about survival statistics. The stages of rectal cancer are indicated by Roman numerals that range from 0 to IV. The lowest stage indicates cancer that is limited to the lining of the inside of the rectum. By stage IV, the cancer is considered advanced and has spread (metastasized) to other areas of the body.
Read more about: Colorectal cancer risk factors
Read more about: Rectal cancer stage 3
Read more about: rectal cancer symptoms
What is the survival rate of rectal cancer?
For rectal cancer, the overall 5-year survival rate for people is 67%. If the cancer is diagnosed at a localized stage, the survival rate is 89%. If the cancer has spread to surrounding tissues or organs and/or the regional lymph nodes, the 5-year survival rate is 71%. If the cancer has spread to distant parts of the body, the 5-year survival rate is 15%.
What stage is T3 rectal cancer?
Patients with T3 rectal cancer have tumors that have spread through the bowel muscle, but have not invaded adjacent organs. Patients with T3 tumors and negative lymph nodes are considered to have stage II rectal cancer. If lymph nodes are involved (but the cancer has not spread to distant parts of the body), the cancer is stage III.
The prognosis of patients with T3 rectal cancer depends on whether or not the lymph nodes are involved, but may also depend on the extent to which the tumor invades the area known as the mesorectum. The mesorectum is fatty tissue that surrounds the rectum; it contains blood vessels and lymph nodes. The extent of mesorectal invasion varies among patients with T3 tumors, but is not taken into account when assigning cancer stage.
Read more about: How you can Prevented from Colorectal Cancer?
Read more about: Rectal bleeding
Read more about: Colorectal Cancer treatment
How is a rectal tumor removed?
The type of surgery recommended for patients with rectal cancer depends on the stage of their cancer and the location of their cancer inside the rectum. The part of the rectum closest to the colon is called the upper rectum, while the part of the rectum closest to the anus is called the lower rectum.
- Local transanal resection or excision: This surgery is used to remove early stage rectal cancers in the lower rectum. It is performed by instruments inserted through the rectum. The surgeon removes the cancer from the rectal wall and may remove some of the surrounding rectal tissue.
- Transanal endoscopic surgery: This surgery is used to remove larger cancers that may be higher in the rectum and difficult to remove through local transanal resection. For this procedure, surgeons use special equipment that is inserted through the anus and into the rectum.
- Transanal minimally invasive surgery (TAMIS): TAMIS is performed by using standard laparoscopic equipment instead of the specialized equipment required for transanal endoscopic surgery. The laparoscope and other instruments are inserted through a special port placed in the anus to remove early stage cancer from the rectum.
- Low anterior resection: This surgery, for some stage 1, stage 2 and stage 3 cancers in the upper rectum, removes the part of the rectum containing the tumor and then reattaches the colon to the remaining part of the rectum. The incisions for this surgery are made through the abdomen.
- Proctectomy: This surgery, for some stage 1 and many stage 2 and stage 3 cancers in the middle and lower rectum, removes the entire rectum through abdominal incisions. The colon is then attached to the anus, in a procedure called a colo-anal anastomosis. During anastomosis surgery, the surgeon may create a small pouch in the colon to replace the rectum for collecting fecal matter.
- Abdominoperineal resection (APR): This surgery, usually performed for stage 2 and stage 3 cancers in the lower to middle rectum, removes the rectum through abdominal incisions as well as the anus and sphincter muscles through incisions around the anus.
- Total mesorectal excision (TME): In procedures where the total rectum is removed, TME surgery is recommended to remove the tissue next to the rectum that contains lymph nodes and blood vessels. Studies show that removing this tissue can reduce the five to 10-year recurrence rate of rectal cancer to between 5 and 10 percent.
Read more about: Rectal Cancer Symptoms
Read more about: Does colorectal cancer occur in old people?
Read more about: Rectal Cancer Staging Radiology

