Myomectomy Surgery
What is Myomectomy?
Type of myomectomy surgery
Good candidate for Myomectomy
What can one expect from Myomectomy?
Myomectomy
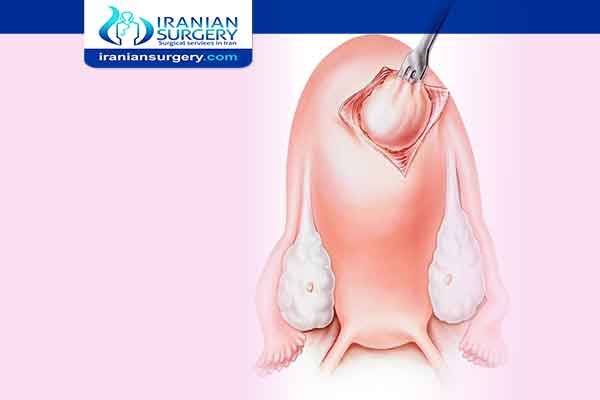
Myomectomy (my-o-MEK-tuh-me) is a surgical procedure to remove uterine fibroids — also called leiomyomas (lie-o-my-O-muhs). These common noncancerous growths appear in the uterus. Uterine fibroids usually develop during childbearing years, but they can occur at any age.
The surgeon's goal during myomectomy is to take out symptom-causing fibroids and reconstruct the uterus. Unlike a hysterectomy, which removes your entire uterus, a myomectomy removes only the fibroids and leaves your uterus.
Women who undergo myomectomy report improvement in fibroid symptoms, including decreased heavy menstrual bleeding and pelvic pressure.
Read more about: Endometriosis treatment
Type of myomectomy surgery
A myomectomy can be performed several different ways. Depending on the size, number and location of your fibroids, you may be eligible for an abdominal myomectomy, a laparoscopic myomectomy or a hysteroscopic myomectomy.
- Abdominal Myomectomy
Also known as an "open" myomectomy, an abdominal myomectomy is a major surgical procedure. It involves making an incision through the skin on the lower abdomen, known as a "bikini cut," and removing the fibroids from the wall of the uterus. The uterine muscle is then sewn back together using several layers of stitches. You will be asleep during the procedure.
Blood loss during the surgery may require a blood transfusion. Some women store their blood before the operation in order to receive their own blood rather than blood from the blood bank.
Most women spend two nights in the hospital and four to six weeks recovering at home. After the procedure, you will have a four-inch horizontal scar near your pubic hair or "bikini" line.
After a myomectomy, your doctor may recommend a Caesarean section (C-section) for the delivery of future pregnancies. This is to reduce the chance that your uterus could open apart during labor. The need for C-section will depend on how deeply the fibroids were embedded in the wall of the uterus at the time of surgical removal.
It is also important to note that new fibroids may develop, resulting in recurrent symptoms and additional procedures.
- Laparoscopic Myomectomy
Only certain fibroids can be removed by a laparoscopic myomectomy. If the fibroids are large, numerous or deeply embedded in the uterus, then an abdominal myomectomy may be necessary. Also, sometimes during the operation it is necessary to switch from a laparoscopic myomectomy to an abdominal myomectomy.
You will be asleep during the procedure, which is performed in the operating room. First, four one-centimeter incisions are made in the lower abdomen: one at the navel (belly button), one below the bikini line (near the pubic hair) and one near each hip. The abdominal cavity is then filled with carbon dioxide gas. A thin, lighted telescope, called a laparoscope, is placed through an incision, allowing doctors to see the ovaries, fallopian tubes and uterus. Long instruments, inserted through the other incisions, are used to remove the fibroids. The uterine muscle is sewn back together. At the end of the procedure, the gas is released and the skin incisions are closed.
Most women spend one night in the hospital and two to four weeks recovering at home. After the procedure, you will have small scars on your skin where the incisions were made.
Read more about: Tubal Ligation Reversal

- Hysteroscopic Myomectomy
Only women with submucosal fibroids are eligible for a hysteroscopic myomectomy. Fibroids located within the uterine wall cannot be removed with this technique.
This is an outpatient surgical procedure, during which the patient is usually asleep. During the procedure, you will lie on your back with your feet held in gynecology stirrups. A speculum is placed in the vagina. A long, slender "telescope" is placed through the cervix into the uterine cavity. Fluid is introduced into the uterine cavity to lift apart the walls. Instruments passed through the hysteroscope are used to shave off the submucosal fibroids.
After the procedure, you will be able to go home after several hours of observation in the recovery room.
You may experience cramping and light bleeding after the procedure. Typical recovery involves one to four days of resting at home. You will not have any scars on your skin after the procedure.
Read more about: Hysteroscopy for unexplained infertility
Good candidate for Myomectomy
Myomectomy is an option for women with fibroids who wish to get pregnant in the future, or who want to keep their uterus for another reason.
Unlike a hysterectomy, which takes out your entire uterus, myomectomy removes your fibroids but leaves your uterus in place. This allows you to try for children in the future.
The type of myomectomy your doctor recommends depends on the size and location of your fibroids:
- Abdominal myomectomy may be best for you if you have many or very large fibroids growing in your uterine wall.
- Laparoscopic myomectomy may be better if you have smaller and fewer fibroids.
- Hysteroscopic myomectomy may be better if you have smaller fibroids inside your uterus
Read more about: Hysteroscopy infertility treatment
What can one expect from Myomectomy?
Immediate relive from troublesome symptoms of fibroids is anticipated following this surgery. Complete recovery takes place after 2-3 weeks after a laparoscopic Myomectomy, while abdominal / open Myomectomy requires 4-6 weeks for a complete recovery. Heavy and weight bearing activities such as lifting heavy objects, running, climbing stairs, driving and strenuous exercises are asked to be avoided during the recovery phase. Surgeon may also advice to avoid intercourse and using tampon till complete recovery takes place. It is also advisable to wait till three months after surgery before attempting for conception.
You will still have your uterus and all reproductive organs following myomectomy. Once healed, there should be no effects on your sexual activity, and you should still be able to conceive. Depending on the depth of the scar in your uterus, you may require an elective caesarean section at 38 weeks to safely give birth. If you are seeking myomectomy as a remedy to excessive menstrual bleeding, it is important to know that the operation is unsuccessful in around 20 per cent of cases - your heavy menstrual flow may be due to factors other than fibroids. See your doctor for further information and advice.
Read more about: Can hysteroscopy cause infertility?
Myomectomy surgery risk
Myomectomy has a low complication rate. Still, the procedure poses a unique set of challenges. Risks of myomectomy include:
- Excessive blood loss. Many women with uterine leiomyomas already have low blood counts (anemia) due to heavy menstrual bleeding, so they're at a higher risk of problems due to blood loss. Your doctor may suggest ways to build up your blood count before surgery.
During myomectomy, surgeons take extra steps to avoid excessive bleeding. These may include blocking flow from the uterine arteries by using tourniquets and clamps and injecting medications around fibroids to cause blood vessels to clamp down. However, most steps don't reduce the risk of needing a transfusion.
In general, studies suggest that there is less blood loss with hysterectomy than myomectomy for similarly sized uteruses.
- Scar tissue. Incisions into the uterus to remove fibroids can lead to adhesions — bands of scar tissue that may develop after surgery. Laparoscopic myomectomy may result in fewer adhesions than abdominal myomectomy (laparotomy).
- Pregnancy or childbirth complications. A myomectomy can increase certain risks during delivery if you become pregnant. If your surgeon had to make a deep incision in your uterine wall, the doctor who manages your subsequent pregnancy may recommend cesarean delivery (C-section) to avoid rupture of the uterus during labor, a very rare complication of pregnancy. Fibroids themselves are also associated with pregnancy complications.
- Rare chance of hysterectomy. Rarely, the surgeon must remove the uterus if bleeding is uncontrollable or other abnormalities are found in addition to fibroids.
- Rare chance of spreading a cancerous tumor. Rarely, a cancerous tumor can be mistaken for a fibroid. Taking out the tumor, especially if it's broken into little pieces (morcellation) to remove through a small incision, can lead to spread of the cancer. The risk of this happening increases after menopause and as women age.
In 2014, the Food and Drug Administration (FDA) cautioned against using a laparoscopic power morcellator for most women undergoing myomectomy. The American College of Obstetricians and Gynecologists (ACOG) recommends you talk to your surgeon about the risks and benefits of morcellation.
Strategies to prevent possible surgical complications
To minimize risks of myomectomy surgery, your doctor may recommend:
- Iron supplements and vitamins. If you have iron deficiency anemia from heavy menstrual periods, your doctor might recommend iron supplements and vitamins to allow you to build up your blood count before surgery.
- Hormonal treatment. Another strategy to correct anemia is hormonal treatment before surgery. Your doctor may prescribe a gonadotropin-releasing hormone (GnRH) agonist, birth control pills or other hormonal medication to stop or decrease your menstrual flow. When given as therapy, a GnRH agonist blocks the production of estrogen and progesterone, stopping menstruation and allowing you to rebuild hemoglobin and iron stores.
- Therapy to shrink fibroids. Some hormonal therapies, such as GnRH agonist therapy, can also shrink your fibroids and uterus enough to allow your surgeon to use a minimally invasive surgical approach — such as a smaller, horizontal incision rather than a vertical incision, or a laparoscopic procedure instead of an open procedure.
Some research suggests that intermittent GnRH agonist therapy, over time, can shrink fibroids and decrease bleeding enough that surgery isn't needed.
In most women, GnRH agonist therapy causes symptoms of menopause, including hot flashes, night sweats and vaginal dryness. However, these discomforts end after you stop taking the medication. Treatment generally occurs over several months before surgery.
Evidence suggests that not all women should take GnRH agonist therapy before myomectomy. GnRH agonist therapy may soften and shrink fibroids so much that their detection becomes more difficult. The cost of the medication and the risk of side effects must be weighed against the benefits.
Another family of drugs called selective progesterone receptor modulators (SPRMs), such as ulipristal (ella), may also shrink fibroids and reduce bleeding. Outside the United States, ulipristal is approved for three months of therapy before a myomectomy.
Before Myomectomy surgery
Gather information. Before surgery, get all the information you need to feel confident about your decision to have a myomectomy. Ask your doctor and surgeon questions.
Follow instructions about food and medications. You'll need to stop eating or drinking anything in the hours before your surgery, follow your doctor's recommendations on the specific number of hours. If you're on medications, ask your doctor if you should change your usual medication routine in the days before surgery. Tell your doctor about any over-the-counter medications, vitamins or other dietary supplements that you're taking.
Discuss the type of anesthesia and pain medication you may receive. Abdominal, laparoscopic and robotic myomectomies are performed under general anesthesia, which means you're asleep during the surgery. Hysteroscopic myomectomy is performed under general anesthesia or spinal anesthesia, where medication is injected into your spinal canal to numb the nerves in the lower half of your body. Ask about pain medication and how it will likely be given.
Arrange for help. Your facility may require that you have someone accompany you on the day of surgery. Make sure you have someone lined up to help with transportation and to be supportive.
Plan for a hospital stay if necessary. Whether you stay in the hospital for just part of the day or overnight depends on the type of procedure you have. Abdominal (open) myomectomy usually requires a hospital stay of two to three days. In most cases, laparoscopic or robotic myomectomy only requires an overnight stay. Hysteroscopic myomectomy is often done with no overnight hospital stay.
Read more about: Hemorrhoidectomy surgery
During Myomectomy Surgery
The procedure will differ depending on what type of myomectomy you’re having.
- Abdominal myomectomy
During this procedure, you’ll be placed under general anesthesia.
Your surgeon will first make an incision through your lower abdomen into your uterus. This can be done in a couple of ways:
- A horizontal incision 3 to 4 inches long, just over your pubic bone. This type of incision causes less pain and leaves a smaller scar but may not be big enough to remove large fibroids.
- A vertical incision from just below your belly button to just above your pubic bone. This incision type is rarely used today but it may work better for larger fibroids and cuts down on bleeding.
Once the incision is made, your surgeon will remove your fibroids from your uterine wall. Then they’ll stitch your uterine muscle layers back together.
Most women who have this procedure spend one to three days in the hospital.
- Laparoscopic myomectomy
While you’re under general anesthesia, your surgeon will make four small incisions. These will each be about ½-inch long in your lower abdomen. Your belly will be filled with carbon dioxide gas to help the surgeon see inside your abdomen.
The surgeon will then place a laparoscope into one of the incisions. A laparoscope is a thin, lighted tube with a camera on one end. Small instruments will be placed into the other incisions.
If the surgery is being done robotically, your surgeon will control the instruments remotely using a robotic arm.
Your surgeon may cut your fibroids into small pieces to remove them. If they are too large, your surgeon may change to an abdominal myomectomy and make a larger incision in your abdomen.
Afterward, your surgeon will remove the instruments, release the gas, and close your incisions. Most women who have this procedure stay in the hospital for one night.
- Hysteroscopic myomectomy
You will get a local anesthetic or be placed under general anesthesia during this procedure.
The surgeon will insert a thin, lighted scope through your vagina and cervix into your uterus. They’ll place a liquid in your uterus to widen it to allow them to see your fibroids more clearly.
Your surgeon will use a wire loop to shave off pieces of your fibroid. Then, the liquid will wash out the removed pieces of fibroid.
You should be able to go home the same day as your surgery.
Read more about: Laparoscopic surgery
Myomectomy recovery
After the operation, you can expect:
- Your temperature, pulse, respiration and blood pressure is observed and noted.
- Any vaginal discharge is noted.
- An intravenous fluid line may still be running into your arm to replace fluids in your body. Antibiotics may be included to combat infection.
- You may have some tubes at the wound site to drain off excess fluid if necessary.
- If you need pain relief, tell your nurse.
- You may have a catheter to drain off urine for the next day or so.
- You are given a normal diet, once your doctor feels it is safe to do so. Tell your nurses as soon as you pass wind or a bowel motion, as this shows that your digestive system is getting back to normal.
- Perform your breathing, coughing and leg exercises hourly when you are awake.
- You are assisted out of bed and taken for a walk the day following surgery.
- You may be in hospital for five to seven days following surgery.
Be guided by your doctor, but general suggestions include:
- Try to rest as much as possible for two weeks.
- Avoid standing for more than a few minutes at a time.
- Continue to take your medications, and follow strictly the instructions on taking your antibiotics.
- After two weeks, aim to walk for about 10 minutes every day, unless advised otherwise by your doctor.
- Depending on the type of surgery, you can return to work within two to six weeks (abdominal myomectomy takes the longest recovery time).
- If you have any excessive vaginal bleeding, or signs of infection at your wound site (such as redness, increasing pain, swelling, or an increased or offensive discharge from your wound), see your doctor immediately.
Read more about: Female Pelvic Laparoscopy
Results of Myomectomy
Outcomes from myomectomy may include:
- Symptom relief. After myomectomy surgery, most women experience relief of bothersome signs and symptoms, such as excessive menstrual bleeding and pelvic pain and pressure.
- Fertility improvement. Women who undergo laparoscopic myomectomy, with or without robotic assistance, have good pregnancy outcomes within about a year of surgery. After a myomectomy, suggested waiting time is three to six months before attempting conception to allow your uterus time to heal.
Fibroids that your doctor doesn't detect during surgery or fibroids that are not completely removed could eventually grow and cause symptoms. New fibroids, which may or may not require treatment, can also develop. Women who had only one fibroid have a lower risk of developing new fibroids — often termed the recurrence rate — than do women who had multiple fibroids. Women who become pregnant after surgery also have a lower risk of developing new fibroids than women who don't become pregnant.
Women who have new or recurring fibroids may have additional, nonsurgical treatments available to them in the future. These include:
- Uterine artery embolization (UAE). Microscopic particles are injected into one or both uterine arteries, limiting blood supply.
- Radiofrequency volumetric thermal ablation (RVTA). Radiofrequency energy is used to wear away (ablate) fibroids using friction or heat — for instance, guided by an ultrasound probe.
- MRI-guided focused ultrasound surgery (MRgFUS). A heat source is used ablate fibroids, guided by magnetic resonance imaging (MRI).
Some women with new or recurring fibroids may choose a hysterectomy if they have completed childbearing.
Read more about: Hysterectomy surgery

