What is Esophageal Cancer?
Esophageal cancer is a cancer that occurs in the esophagus — a long, hollow tube that runs from your throat to your stomach. Your esophagus helps move the food you swallow from the back of your throat to your stomach to be digested.
Esophageal cancer usually begins in the cells that line the inside of the esophagus. Esophageal cancer can occur anywhere along the esophagus. More men than women get esophageal cancer.
Esophageal cancer is the sixth most common cause of cancer deaths worldwide. Incidence rates vary within different geographic locations. In some regions, higher rates of esophageal cancer may be attributed to tobacco and alcohol use or particular nutritional habits and obesity.
Read more about : Gastric cancer treatment
Before Esophageal Cancer Treatment
Symptoms
Signs and symptoms of esophageal cancer include:
. Difficulty swallowing (dysphagia)
. Weight loss without trying
. Chest pain, pressure or burning
. Worsening indigestion or heartburn
. Coughing or hoarseness
Early esophageal cancer typically causes no signs or symptoms.
When to see a doctor
Make an appointment with your doctor if you have any persistent signs and symptoms that worry you.
If you've been diagnosed with Barrett's esophagus, a precancerous condition caused by chronic acid reflux, your risk of esophageal cancer is higher. Ask your doctor what signs and symptoms to watch for that may signal that your condition is worsening.
Screening for esophageal cancer may be an option for people with Barrett's esophagus. If you have Barrett's esophagus, discuss the pros and cons of screening with your doctor.
Causes
It's not exactly clear what causes esophageal cancer.
Esophageal cancer occurs when cells in the esophagus develop changes (mutations) in their DNA. The changes make cells grow and divide out of control. The accumulating abnormal cells form a tumor in the esophagus that can grow to invade nearby structures and spread to other parts of the body.
Read more about : Colorectal cancer surgery
Read more about : Anal Cancer Treatment
Risk factors
It's thought that chronic irritation of your esophagus may contribute to the changes that cause esophageal cancer. Factors that cause irritation in the cells of your esophagus and increase your risk of esophageal cancer include:
. Having gastroesophageal reflux disease (GERD)
. Smoking
. Having precancerous changes in the cells of the esophagus (Barrett's esophagus)
. Being obese
. Drinking alcohol
. Having bile reflux
. Having difficulty swallowing because of an esophageal sphincter that won't relax (achalasia).
. Having a steady habit of drinking very hot liquids
. Not eating enough fruits and vegetables
. Undergoing radiation treatment to the chest or upper abdomen
Complications
As esophageal cancer advances, it can cause complications, such as:
. Obstruction of the esophagus. Cancer may make it difficult for food and liquid to pass through your esophagus.
. Pain. Advanced esophageal cancer can cause pain.
. Bleeding in the esophagus. Esophageal cancer can cause bleeding. Though bleeding is usually gradual, it can be sudden and severe at times.
Prevention
You can take steps to reduce your risk of esophageal cancer. For instance:
. Quit smoking. If you smoke, talk to your doctor about strategies for quitting. Medications and counseling are available to help you quit. If you don't use tobacco, don't start.
. Drink alcohol in moderation, if at all. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women and up to two drinks a day for men.
. Eat more fruits and vegetables. Add a variety of colorful fruits and vegetables to your diet.
. Maintain a healthy weight. If you are overweight or obese, talk to your doctor about strategies to help you lose weight. Aim for a slow and steady weight loss of 1 or 2 pounds a week.
Diagnosis
Tests and procedures used to diagnose esophageal cancer include:
. Barium swallow study. During this study, you swallow a liquid that includes barium and then undergo X-rays. The barium coats the inside of your esophagus, which then shows any changes to the tissue on the X-ray.
. Using a scope to examine your esophagus (endoscopy). During endoscopy, your doctor passes a flexible tube equipped with a video lens (videoendoscope) down your throat and into your esophagus. Using the endoscope, your doctor examines your esophagus, looking for cancer or areas of irritation.
. Collecting a sample of tissue for testing (biopsy). Your doctor may use a special scope passed down your throat into your esophagus (endoscope) to collect a sample of suspicious tissue (biopsy). The tissue sample is sent to a laboratory to look for cancer cells.
Determining the extent of the cancer
Once a diagnosis of esophageal cancer is confirmed, your doctor may recommend additional tests to determine whether your cancer has spread to your lymph nodes or to other areas of your body.
Tests may include:
. Bronchoscopy
. Endoscopic ultrasound (EUS)
. Computerized tomography (CT)
. Positron emission tomography (PET)
Your doctor uses the information from these procedures to assign a stage to your cancer.
Read more about : Bone cancer stage
During Esophageal Cancer Treatment
Types of esophageal cancer
Esophageal cancer is classified according to the type of cells that are involved. The type of esophageal cancer you have helps determine your treatment options. Types of esophageal cancer include:
. Adenocarcinoma. Adenocarcinoma begins in the cells of mucus-secreting glands in the esophagus. Adenocarcinoma occurs most often in the lower portion of the esophagus. Adenocarcinoma is the most common form of esophageal cancer in the United States, and it affects primarily white men.
. Squamous cell carcinoma. The squamous cells are flat, thin cells that line the surface of the esophagus. Squamous cell carcinoma occurs most often in the upper and middle portions of the esophagus. Squamous cell carcinoma is the most prevalent esophageal cancer worldwide.
. Other rare types. Some rare forms of esophageal cancer include small cell carcinoma, sarcoma, lymphoma, melanoma and choriocarcinoma.
Esophageal cancer stages
Making an educated esophageal cancer treatment decision begins with determining the stage, or progression, of the disease. The stage of esophageal cancer is one of the most important factors in evaluating treatment options.
Our cancer doctors use a variety of diagnostic tests to evaluate esophageal cancer and develop an individualized treatment plan. If you have been recently diagnosed, we will review your pathology to confirm you have received the correct diagnosis and staging information and develop a personalized treatment plan. If you have a recurrence, we will perform comprehensive testing and identify a treatment approach tailored to your needs.
It’s also important to understand that the stage of your cancer may change. Your care team will let you know if your staging information is affected by the progression, or regression, of your disease.
The stages of esophageal cancer are assigned based on the American Joint Committee on Cancer’s (AJCC) TNM system, a commonly accepted method based on three key components:
. T (tumor): This describes the size of the original tumor.
. N (node): This indicates whether the cancer is present in the lymph nodes.
. M (metastasis): This refers to whether cancer has spread to other parts of the body.
A number (0-4) or the letter X is assigned to each factor. In esophageal cancer staging, as in all cancer staging, a higher number indicates increasing severity. For instance, a T1 score indicates a smaller tumor than a T2 score. The letter X means the information could not be assessed.
Once the T, N and M scores have been assigned, one of these overall stages is assigned:
. Stage 1 esophageal cancer: A stage 1 esophageal cancer tumor is small (7 cm or less across) and limited to the esophagus.
. Stage 2 esophageal cancer: A stage 2 esophageal cancer tumor has grown larger but still remains within the esophagus. In this stage of the disease, there is no evidence of spread to lymph nodes or distant sites.
. Stage 3 esophageal cancer: A stage 3 esophageal cancer tumor has grown beyond the esophagus and may now extend into nearby tissues or organs. The cancer may or may not have spread to nearby lymph nodes.
. Stage 4 esophageal cancer: A stage 4 esophageal cancer tumor may be any size and has grown beyond the esophagus. In this stage of esophageal cancer, the disease may have spread to lymph nodes or distant sites like the liver or abdominal cavity.
Treatment
What treatments you receive for esophageal cancer are based on the type of cells involved in your cancer, your cancer's stage, your overall health and your preferences for treatment.
Surgery
Surgery to remove the cancer can be used alone or in combination with other treatments.
Operations used to treat esophageal cancer include:
. Surgery to remove very small tumors. If your cancer is very small, confined to the superficial layers of your esophagus and hasn't spread, your surgeon may recommend removing the cancer and margin of healthy tissue that surrounds it. Surgery can be done using an endoscope passed down your throat and into your esophagus.
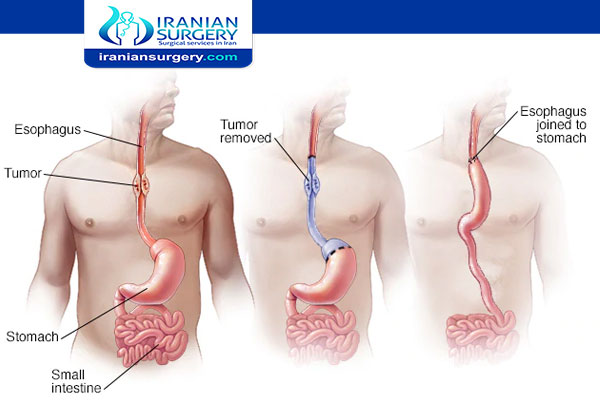
. Surgery to remove a portion of the esophagus (esophagectomy). During esophagectomy, the surgeon removes the portion of your esophagus that contains the cancer, along with a portion of the upper part of your stomach, and nearby lymph nodes. The remaining esophagus is reconnected to your stomach. Usually this is done by pulling the stomach up to meet the remaining esophagus.
. Surgery to remove part of your esophagus and the upper portion of your stomach (esophagogastrectomy). During esophagogastrectomy, the surgeon removes part of your esophagus, nearby lymph nodes and a larger part of your stomach. The remainder of your stomach is then pulled up and reattached to your esophagus. If necessary, part of your colon is used to help join the two.
Esophageal cancer surgery carries a risk of serious complications, such as infection, bleeding and leakage from the area where the remaining esophagus is reattached to the stomach.
Surgery to remove your esophagus can be performed as an open procedure using large incisions or with special surgical tools inserted through several small incisions in your skin (laparoscopically). How your surgery is performed depends on your individual situation and your surgeon's particular approach to managing it.
Treatments for complications
Treatments for esophageal obstruction and difficulty swallowing (dysphagia) can include:
. Relieving esophageal obstruction. If your esophageal cancer has narrowed your esophagus, a surgeon may use an endoscope and special tools to place a metal tube (stent) to hold the esophagus open. Other options include surgery, radiation therapy, chemotherapy, laser therapy and photodynamic therapy.
. Providing nutrition. Your doctor may recommend a feeding tube if you're having trouble swallowing or if you're having esophagus surgery. A feeding tube allows nutrition to be delivered directly to your stomach or small intestine, giving your esophagus time to heal after cancer treatment.
Chemotherapy
Chemotherapy is drug treatment that uses chemicals to kill cancer cells. Chemotherapy drugs are typically used before (neoadjuvant) or after (adjuvant) surgery in people with esophageal cancer. Chemotherapy can also be combined with radiation therapy.
In people with advanced cancer that has spread beyond the esophagus, chemotherapy may be used alone to help relieve signs and symptoms caused by the cancer.
The chemotherapy side effects that you experience depend on which chemotherapy drugs you receive.
Radiation therapy
Radiation therapy uses high-energy beams, such as X-rays and protons, to kill cancer cells. Radiation typically will come from a machine outside your body that aims the beams at your cancer (external beam radiation). Or, less commonly, radiation can be placed inside your body near the cancer (brachytherapy).
Radiation therapy is most often combined with chemotherapy in people with esophageal cancer. It's typically used before surgery, or occasionally after surgery. Radiation therapy is also used to relieve complications of advanced esophageal cancer, such as when a tumor grows large enough to stop food from passing to your stomach.
Side effects of radiation to the esophagus include sunburn-like skin reactions, painful or difficult swallowing, and damage to nearby organs, such as the lungs and heart.
Combined chemotherapy and radiation
Combining chemotherapy and radiation therapy may enhance the effectiveness of each treatment. Combined chemotherapy and radiation may be the only treatment you receive, or combined therapy can be used before surgery. But combining chemotherapy and radiation treatments increases the likelihood and severity of side effects.
Targeted drug therapy
Targeted drug treatments focus on specific weaknesses present within cancer cells. By blocking these weaknesses, targeted drug treatments can cause cancer cells to die. For esophageal cancer, targeted drugs are usually combined with chemotherapy for advanced cancers or cancers that don't respond to other treatments.
Immunotherapy
Immunotherapy is a drug treatment that helps your immune system to fight cancer. Your body's disease-fighting immune system might not attack cancer because the cancer cells produce proteins that make it hard for the immune system cells to recognize the cancer cells as dangerous. Immunotherapy works by interfering with that process. For esophageal cancer, immunotherapy might be used when the cancer is advanced, cancer has come back or the cancer has spread to other parts of the body.
Alternative medicine
Complementary and alternative therapies may help you cope with the side effects of cancer and cancer treatment. For instance, people with esophageal cancer may experience pain caused by cancer treatment or by a growing tumor. Your doctor can work to control your pain by treating the cause or with medications. Still, pain may persist, and complementary and alternative therapies may help you cope.
Options include:
. Acupuncture
. Guided imagery
. Massage
. Relaxation techniques
Ask your doctor whether these options are safe for you.
After Esophageal Cancer Treatment
Recovery after Esophagectomy
When you leave the hospital, the area around the cuts (incisions) may still be swollen or bruised. It may also feel numb. This is normal and may continue for a few weeks. You will probably need to take pain medicine for a few weeks.
You will have to be very careful about what you eat for several months after surgery and maybe for the rest of your life. You will probably have a feeding tube (J-tube) in your belly. This will come out when you can eat normally and get enough nutrition. This could be about 4 to 6 weeks after surgery, but it could take longer. Your doctor will give you detailed information on what you can eat, how you should eat, and how to use the feeding tube.
You may also have digestive problems for a few months. These include weight loss, a lot of gas, and a problem called dumping syndrome. Dumping syndrome usually occurs after you eat rich or fatty meals. It may cause you to feel light-headed or sick to your stomach, or to have cramps and diarrhea.
Most people go back to work or their normal routine after 6 to 12 weeks. You will need more time to get better if you need other treatment for cancer, such as chemotherapy. It will take 3 to 4 months to get back to your usual activities.
This care sheet gives you a general idea about how long it will take for you to recover. But each person recovers at a different pace.
How can you care for yourself at home?
. Activity
. Rest when you feel tired.
. Be active. Walking is a good choice.
. You may be able to take showers (unless you have a drain in your incision). If you have a drain, follow your doctor's instructions to empty and care for it. Keep your feeding tube taped to your skin so it will not fall off. Do not soak in a tub or use a hot tub.
. Do not lean your head back quickly or for a long period of time. This puts pressure on the neck and may slow your healing.
. You can do your normal activities when it feels okay to do so.
. Allow your body to heal. Don't move quickly or lift anything heavy until you are feeling better.
. Ask your doctor when you can drive again.
. Diet
Your diet will go from a clear liquid diet, to a full liquid diet, and then to a soft diet before you can eat normally. This generally takes 1 to 2 months. Your doctor will give you specific information about what you can eat. In general:
. If you are on a clear liquid diet, eat or drink clear, fat-free broth or bouillon soup. You can also eat flavored ice pops and gelatin desserts, such as Jell-O.
. If you are on a full liquid diet, you can have everything on the clear liquid diet. You can also have creamy soups, cooked cereals, milk, protein shakes, fruit juices, puddings, and ice cream.
. If you are on a soft diet, eat foods that are easy to swallow and digest. These include:
. Most cereals.
. Scrambled eggs and omelets.
. Canned or cooked fruits.
. Finely ground beef, chicken, turkey, and pork.
. Mild cheeses.
. Mashed potatoes.
. Cooked or pureed vegetables.
. Yogurt.
. Medicines
. Your doctor will tell you if and when you can restart your medicines. He or she will also give you instructions about taking any new medicines.
. If you take aspirin or some other blood thinner, ask your doctor if and when to start taking it again. Make sure that you understand exactly what your doctor wants you to do.
. Be safe with medicines. Read and follow all instructions on the label.
. If the doctor gave you a prescription medicine for pain, take it as prescribed.
. If you are not taking a prescription pain medicine, ask your doctor if you can take an over-the-counter medicine.
. If your doctor prescribed antibiotics, take them as directed. Do not stop taking them just because you feel better. You need to take the full course of antibiotics.
. Incision care
. If you have strips of tape on the incision, leave the tape on for a week or until it falls off.
. Wash the area daily with warm, soapy water, and pat it dry. Your doctor will tell you how to take care of this. Don't use hydrogen peroxide or alcohol, which can slow healing.
. You may cover the area with a gauze bandage if it weeps or rubs against clothing. Change the bandage every day.
. Other instructions
. It is normal to have some yellowish mucus around your feeding tube. This is not a sign of infection.
. Keep your feeding tube clamped unless you are using it.
. Keep the tube taped to your skin at all times, and leave some slack in the tube. This helps prevent pain and keeps the tube from coming out.
. If you are using your feeding tube:
. Clean around the tube with water before and after you use it.
. Flush the tube daily as your doctor tells you to.
. Do not put any pills through the tube. They can clog it.
Long-term outlook
Your chances for recovery improve the earlier the cancer is found.
Esophageal cancer is usually found in the later stages when it can only be treated but not cured.
Your chances of survival may improve with surgery if the cancer hasn’t spread outside of your esophagus.
Sources:
. https://www.cancercenter.com/cancer-types/esophageal-cancer/stages
. https://www.mayoclinic.org/diseases-conditions/esophageal-cancer/symptoms-causes/syc-20356084
. https://www.healthline.com/health/esophageal-cancer
. https://my.clevelandclinic.org/health/diseases/6137-esophageal-cancer