Varicose veins
What is the best treatment for varicocele?
What are Varicose Veins?
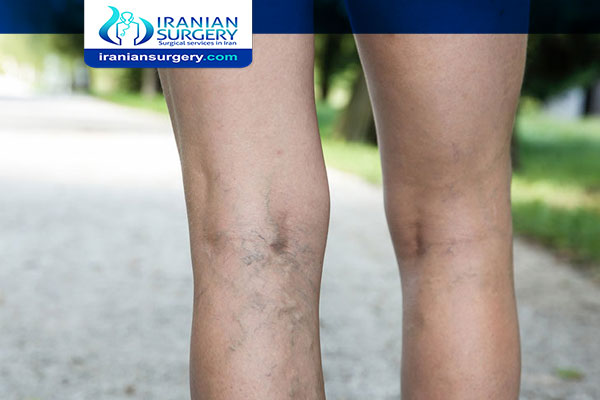
Varicose veins, also known as varicoses or varicosities, occur when your veins become enlarged, dilated, and overfilled with blood. Varicose veins typically appear swollen and raised, and have a bluish-purple or red color. They are often painful.
The condition is very common, especially in women. Around 25 percent of all adults have varicose veins. In most cases, varicose veins appear on the lower legs.
Read more about : Varicose vein laser surgery recovery time
Read more about : Leg pain after varicose vein surgery
Read more about : Varicose Vein Complications
Before Varicose Veins Treatment
Symptoms
In the majority of cases, there is no pain, but signs and symptoms of varicose veins may include:
. Veins look twisted, swollen, and lumpy (bulging)
. The veins are blue or dark purple
Some patients may also experience:
. Aching legs
. Legs feel heavy, especially after exercise or at night
. A minor injury to the affected area may result in longer bleeding than normal
. Lipodermatosclerosis – fat under the skin just above the ankle can become hard, resulting in the skin shrinking.
. Swollen ankles
. Telangiectasia in the affected leg (spider veins)
. There may be a shiny skin discoloration near the varicose veins, usually brownish or blue in color.
. Venous eczema (stasis dermatitis) – skin in the affected area is red, dry, and itchy.
. When suddenly standing up, some individuals experience leg cramps.
. A high percentage of people with varicose veins also have restless legs syndrome.
. Atrophie Blanche – irregular whitish patches that look like scars appear at the ankles.

When to see a doctor
Self-care — such as exercise, elevating your legs or wearing compression stockings — can help you ease the pain of varicose veins and may prevent them from getting worse. But if you’re concerned about how your veins look and feel and self-care measures haven’t stopped your condition from getting worse, see your doctor.
Causes
The veins have one-way valves so that the blood can travel in only one direction. If the walls of the vein become stretched and less flexible (elastic), the valves may get weaker. A weakened valve can allow blood to leak backward and eventually flow in the opposite direction. When this occurs, blood can accumulate in the vein(s), which then become enlarged and swollen.
The veins furthest from the heart are most often affected, such as those in the legs. This is because gravity makes it harder for blood to flow back to the heart. Any condition that puts pressure on the abdomen has the potential to cause varicose veins; for instance, pregnancy, constipation and, in rare cases, tumors.
Risk factors
Experts are not sure why the walls of veins stretch or why the valves become faulty. In many cases, it occurs for no clear reason. However, some potential risk factors include:
. Menopause
. Pregnancy
. Being aged over 50
. Standing for long periods
. Family history of varicose veins
. Obesity
The following risk factors are linked to a higher risk of having varicose veins:
. Gender: Varicose veins affect women more often than males. It may be that female hormones relax veins. If so, taking birth control pills or hormone therapy (HT) might contribute.
. Genetics: Varicose veins often run in families.
. Obesity: Being overweight or obese increases the risk of varicose veins.
. Age: The risk increases with age, due to wear and tear on vein valves.
. Some jobs: An individual who has to spend a long time standing at work may have a higher chance of varicose veins.
Read more about : Carpal Tunnel Surgery
Read more about : Herniated disk treatment
Read more about : Cycling after knee arthroscopy
Read more about : Heart attack
Pregnancy and varicose veins
Women are much more likely to develop varicose veins during their pregnancy than at any other time in their lives. Pregnant women have much more blood in their body; this places extra pressure on the circulatory system.
Additionally, changes in hormone levels can lead to a relaxation of the blood vessel walls. Both these factors raise the risk of having varicose veins.
As the uterus (womb) grows, there is more pressure on the veins in the mother’s pelvic area. In the majority of cases, the varicose veins go away after the pregnancy is over; this is not always the case, and sometimes, even if the varicose veins improve, there may be some left visible.
Diagnosis
A physical examination, mainly visual, by a doctor will decide whether or not a patient has varicose veins. The patient will be asked to stand while the doctor checks for signs of swelling.
The following diagnostic tests are sometimes ordered:
. Doppler test: An ultrasound scan to check the direction of blood flow in the veins. This test also checks for blood clots or obstructions in the veins.
. Color duplex ultrasound scan: This provides color images of the structure of veins, which helps the doctor identify any abnormalities. It can also measure the speed of blood flow.
The patient may also be asked questions about the symptoms. In some cases, a doctor might refer the patient to a vascular specialist.
Varicose Vein Complications
In addition to the several side effects of varicose veins, there are several complications that may occur. These complications are rare but, if present, usually develop several years after initial diagnosis for most patients.
The complication vary greatly in severity but some effects have the potential to be fatal, such as the possibility of pulmonary embolism occurring following deep vein thrombosis.
. Phlebitis
Phlebitis, also known as thrombophlebitis, refers to inflammation of the veins that may be accompanied by the formation of hard and tender clots. This is a distinct condition from deep vein thrombosis, however, and is markedly less severe and may not always require treatment.
This commonly results in symptoms of swollen, painful, reddened and heated skin due to the inflammation in the area.
. Bleeding
Rarely, patients with varicose veins experience a significant knock to their legs, resulting in bleeding from the ruptured vein. This can be quite alarming for patients as a significant volume of blood can be lost in a short period of time as the blood flows backwards out of the vein.
However, this complication can be managed relatively easily with adequate care. Simply raise the area and apply firm pressure to the veins, which is usually sufficient to stop the immediate flow of blood. This can be followed by pharmaceutical care to reduce the risk of a subsequent bleed.
. Deep Vein Thrombosis (DVT)
In some cases, blood clots can form in varicose veins and lead to serious consequences such as pulmonary embolism. It is not clear if varicose veins are likely to cause DVT, but the two conditioners are certainly related.
The development of blood clots in superficial veins is the most common and up to 1 in 5 of these may progress into a thrombus of the deep vein in the leg. If DVT is suspected it is essential that the patient seek appropriate medical therapy to reduce the risk of embolisation and further damage.
. Venous Insufficiency
If the blood flow remains disrupted for an extended period of time, it can affect the oxygen exchange and processing of nutrients and waste products, which is a condition known as chronic venous insufficiency. This then places the individual at a higher risk of other complications.
. Dermatitis and Complications of the Skin
There are several complications of varicose veins that are related to the skin including:
. Varicose eczema – results in red, scaly and flaky skin in the affected area. Some blisters and crust on the skin may also form.
. Lipodermatosclerosis – is a more serious complication that leads to hardened and tight skin, which may change colour to red or brown. This usually occurs in the calf area of the legs and is often non-reversible.
. Venous Ulcers
A venous ulcer may develop in a patient with varicose veins, due to the increased venous pressure in the lower legs. This occurs as a result of fluid building up underneath the skin and causing the area to swell and create an ulcer, most commonly near the ankles.
In most cases, a small injury such as a bite or scratch take longer to heal due to the insufficient blood flow to the area, which is responsible for causing the ulcer.
Prevention
There’s no way to completely prevent varicose veins. But improving your circulation and muscle tone may reduce your risk of developing varicose veins or getting additional ones. The same measures you can take to treat the discomfort from varicose veins at home can help prevent varicose veins, including:
. Exercising
. Watching your weight
. Eating a high-fiber, low-salt diet
. Avoiding high heels and tight hosiery
. Elevating your legs
. Changing your sitting or standing position regularly
Read more about : Herniated disk treatment
Read more about : Cycling after knee arthroscopy
Read more about : Heart attack
During Varicose Veins Treatment
Treatment
Fortunately, treatment usually doesn’t mean a hospital stay or a long, uncomfortable recovery. Thanks to less invasive procedures, varicose veins can generally be treated on an outpatient basis.
Ask your doctor if insurance will cover any of the cost of your treatment. If done for purely cosmetic reasons, you’ll likely have to pay for the treatment of varicose veins yourself.
Self-care
Self-care — such as exercising, losing weight, not wearing tight clothes, elevating your legs, and avoiding long periods of standing or sitting — can ease pain and prevent varicose veins from getting worse.
Compression stockings
Wearing compression stockings all day is often the first approach to try before moving on to other treatments. They steadily squeeze your legs, helping veins and leg muscles move blood more efficiently. The amount of compression varies by type and brand.
You can buy compression stockings at most pharmacies and medical supply stores. Prescription-strength stockings also are available, and are likely covered by insurance if your varicose veins are causing symptoms.
Additional treatments for more-severe varicose veins
If you don’t respond to self-care or compression stockings, or if your condition is more severe, your doctor may suggest one of these varicose vein treatments:
. Sclerotherapy. In this procedure, your doctor injects small- and medium-sized varicose veins with a solution or foam that scars and closes those veins. In a few weeks, treated varicose veins should fade.
Although the same vein may need to be injected more than once, sclerotherapy is effective if done correctly. Sclerotherapy doesn’t require anesthesia and can be done in your doctor’s office.
. Foam sclerotherapy of large veins. Injection of a large vein with a foam solution is also a possible treatment to close a vein and seal it.
. Laser treatment. Doctors are using new technology in laser treatments to close off smaller varicose veins and spider veins. Laser treatment works by sending strong bursts of light onto the vein, which makes the vein slowly fade and disappear. No incisions or needles are used.
. Catheter-assisted procedures using radiofrequency or laser energy. In one of these treatments, your doctor inserts a thin tube (catheter) into an enlarged vein and heats the tip of the catheter using either radiofrequency or laser energy. As the catheter is pulled out, the heat destroys the vein by causing it to collapse and seal shut. This procedure is the preferred treatment for larger varicose veins.
. High ligation and vein stripping. This procedure involves tying off a vein before it joins a deep vein and removing the vein through small incisions. This is an outpatient procedure for most people. Removing the vein won’t adversely affect circulation in your leg because veins deeper in the leg take care of the larger volumes of blood.
. Ambulatory phlebectomy. Your doctor removes smaller varicose veins through a series of tiny skin punctures. Only the parts of your leg that are being pricked are numbed in this outpatient procedure. Scarring is generally minimal.
. Endoscopic vein surgery. You might need this operation only in an advanced case involving leg ulcers if other techniques fail. Your surgeon uses a thin video camera inserted in your leg to visualize and close varicose veins and then removes the veins through small incisions. This procedure is performed on an outpatient basis.
Varicose veins that develop during pregnancy generally improve without medical treatment within three to 12 months after delivery.
Alternative medicine
Though they haven’t been well-studied, a number of alternative therapies claim to be helpful treatments for chronic venous insufficiency, a condition associated with varicose veins in which leg veins have problems returning blood to the heart. These therapies include:
. Horse chestnut
. Butcher’s broom
. Grape (leaves, sap, seed and fruit)
. Sweet clover
Talk with your doctor before trying any herb or dietary supplement to make sure these products are safe and won’t interfere with any medications.
After Varicose Veins Treatment
Lifestyle and home remedies
There are some self-care measures you can take to decrease the discomfort that varicose veins can cause. These same measures can help prevent or slow the development of varicose veins, as well. They include:
. Exercise. Get moving. Walking is a great way to encourage blood circulation in your legs. Your doctor can recommend an appropriate activity level for you.
. Watch your weight and your diet. Shedding excess pounds takes unnecessary pressure off your veins. What you eat can help, too. Follow a low-salt diet to prevent swelling caused from water retention.
. Watch what you wear. Avoid high heels. Low-heeled shoes work calf muscles more, which is better for your veins. Don’t wear tight clothes around your waist, legs or groin because these garments can reduce blood flow.
. Elevate your legs. To improve the circulation in your legs, take several short breaks daily to elevate your legs above the level of your heart. For example, lie down with your legs resting on three or four pillows.
. Avoid long periods of sitting or standing. Make a point of changing your position frequently to encourage blood flow.
Read more about : Open heart surgery
Read more about : Knee replacement
Read more about : Hip replacement
Outlook
Varicose veins normally get worse over time. This is true even if you make the necessary lifestyle changes to control them and manage your pain. While they may be unsightly, they usually don’t cause any long-term medical problems.
In some cases, varicose veins can lead to ulcers or sores on your legs, blood clots, or chronic inflammation. If you have a severe case, your veins could rupture.
You should see your doctor if you develop any of these symptoms. They may then suggest taking a more aggressive approach, such as surgery or other interventions.

