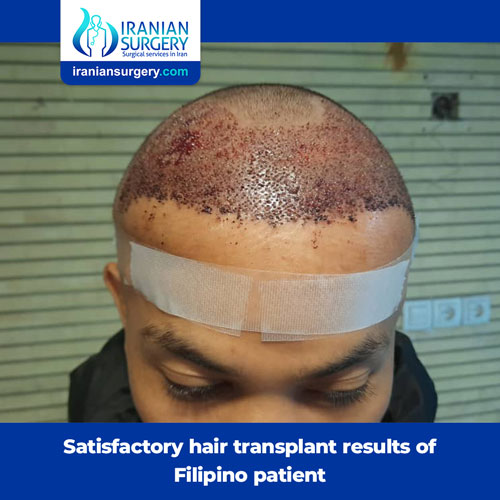
Repaired perforating globe injury
Pre-Op diagnosis:
Repaired perforating globe injury (of unknown mechanism) + intra-orbital foreign body (left eye)
Surgeon : Dr. Zarei is a Fellowship in Retina and Laser surgery and ophthalmologist
Chief Complaint:
The patient was a 3-year-old child who has suffered from perforating eye trauma nearly one month ago. According to documents, scleral laceration had been repaired in Oman and an intra-orbital FB was noticed in CT scan, adjacent to optic nerve.
Work Ups:
The patient was examined by a pediatric neurologist. All neurological examinations were within normal limits except of the lost vision in the left eye. The intra-orbital foreign body did not seem to impose significant ongoing or future risk to vital structures and the removal deemed to be unnecessary and risky. This evaluation was also confirmed by a neurosurgeon.
Ophthalmic examination and evaluation of clinical documents by a retinal surgeon, led to the conclusion that although the overall structural and functional outcome of the case seems to be guarded -a consequence of severity and extent of the primary injury- examination under anesthesia and exploratory/therapeutic eye surgery should be considered to maximize the chance for globe saving, especially considering the inherent limitation of clinical examination in this age group.
Procedure of ocular surgery and intraoperative findings:
Following general anesthesia, the eyes were inspected. No abnormality was noticed in OD. The left eye was formed and IOP was within normal limits (tactile evaluation). A total hyphema, precluding more posterior examination was present. After P&D and placement of a limbal inflow cannula, the AC was washed with BSS. A lacerated iris (supranasal) with posterior synechiae was noticed. Adhesions were released and lensectomy was performed. Vitreous cavity was filled with a massive clot and red cells (some already transformed to “khaki-colored cells”). Following partial clearing of media by doing 23-gauge pars plana deep vitrectomy, a total RRD, subretinal hemorrhage, and a large radial retinal laceration in supranasal area extending from mid periphery to optic disc area were revealed. The optic disc was covered with a mixed tissue that seemed to comprised of clot, fibrous and retinal
tissues. It was concluded that the exit site of FB was at the optic disc or the very close proximity of it and torn retinal tissue was incarcerated in it. After completion of vitrectomy, retinal re-attachment was achieved by performing two circumferential retinotomies, extending temporally and nasally from the most anterior border of retinal laceration and fluid-air exchange. Then 360-degree peripheral endolaser photocoagulation in 6-10 rows, as well as endolaser treatment of borders of retinal tears were performed. The eye was filled with silicone oil (Oxane 5700) and an inferior peripheral iridectomy was made. Pars plan ports and limbal inflow cannula were removed, IOP and leakage from surgical incisions were checked, sub-tenon triamcinolone acetonide and subconjunctival betamethasone + cefazolin were injected and the eye was patched.
Recommendation After Discharge:
Eye drop betamethasone Q2h and tapering to QID in one month
Eye drop homatropine QID for one month
Eye drop ciprofloxacin QID for one week
Ophthalmic evaluation at post-op week 1 and month 1