Is ICSI more successful than IVF?
Does ICSI improve IVF success?
What percentage of eggs fertilize with ICSI?
Is it better to transfer 1 or 2 embryos?
IVF&ICSI
Prior to IVF or ICSI, oocytes (eggs) are retrieved from the woman. Women of advanced age typically have a lower number of oocytes retrieved. As the number of oocytes are fewer, some doctors prefer to use ICSI as it has a greater success rate of fertilization compared to conventional IVF, in general.
In assisted reproductive technology (ART) there are two ways eggs can be fertilised: IVF (in-vitro-fertilisation) or ICSI (intracytoplasmic sperm injection). In IVF thousands of sperm are added to each egg in the hope that one will fertilise the egg. In ICSI the embryologist uses a microscope and very technically advanced equipment to select a single sperm which is injected into the egg. A few days after IVF and ICSI the embryologist checks to see of the eggs have fertilised and developed into embryos. If there are embryos, one (sometimes two) is placed in the uterus and any remaining embryos can be frozen for later use if the treatment is not successful.
Read more about : Type of Infertility Treatment in Iran
Read more about : Egg donation in iran
Read more about: Ivf in Iran
When IVF was first developed in the 1980s it helped many couples who had previously been infertile have children. But IVF didn’t work for couples where the man had very poor sperm. That’s why, in the early 1990s, the ICSI procedure was developed. ICSI has been remarkably successful and helped couples with male factor infertility around the world have children.
Since then there has been an increasing trend to use ICSI for all causes of infertility. In Australia, around two thirds of ART treatments are ICSI. But, is ICSI better than IVF for couples who don’t have male factor infertility? That was the question researchers asked in a paper published today in the journal Human Reproduction.
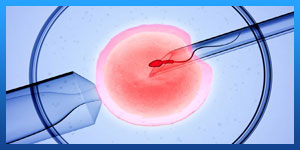
have male factor infertility, ICSI doesn’t increase the chance of having a baby.
The success rates for two common fertility treatments have peaked, with only one in four attempts resulting in pregnancy. The success rate for IVF and a similar technique called intracytoplasmic sperm injection (ICSI) have been around this level for about a decade.
Read more about: What is the success rate of ICSI IVF?
Is ICSI more successful than IVF?
ICSI isn't an alternative to IVF, but rather an optional part of it. It might not be as well known in modern parlance, but it’s much more common and more successful than you’d think. ICSI fertilizes 50% to 80% of eggs," but it’s not foolproof.
Read more about: when is assisted hatching done in IVF
Does ICSI improve IVF success?
ICSI, which has been around since 1992, is an IVF technique that involves a clinical embryologist injecting healthy sperm directly into the ripened egg itself to increase the odds of fertilization. ICSI boasts a pregnancy success rate of 24%. While IVF without ICSI still has a slightly higher pregnancy success rate at 27%, those aren’t bad odds for anyone who’s already tried other methods of assisted reproductive technology. The rate of successful egg fertilization in the laboratory was found to be higher when ICSI was used: 67.5% versus 47.8% with conventional insemination. Fertilization failure was found to be significantly higher when ICSI was not used.
Read more about: IUI vs IVF
What percentage of eggs fertilize with ICSI?
The fertilization rate in the UCSF IVF laboratory is exceptional currently 80 to 85 percent. That is to say, on average, eight out of every 10 eggs will fertilize normally.
Read more about: IVF with frozen donor eggs process
Is it better to transfer 1 or 2 embryos?
Two embryos are not always better than one. Research still shows that transferring one embryo per cycle is the safest option. Transferring two increases the chance of a multiple pregnancy and associated complications. When you transfer more embryos in a transfer, the risk rises that you will have a multiple pregnancy. Let’s look at Sweden: they did away with multiple-embryo transfer and now they have almost exclusively singletons born from IVF.
Read more about: Assisted hatching ivf



