DNA Fragmentation Test
DNA Fragmentation Test
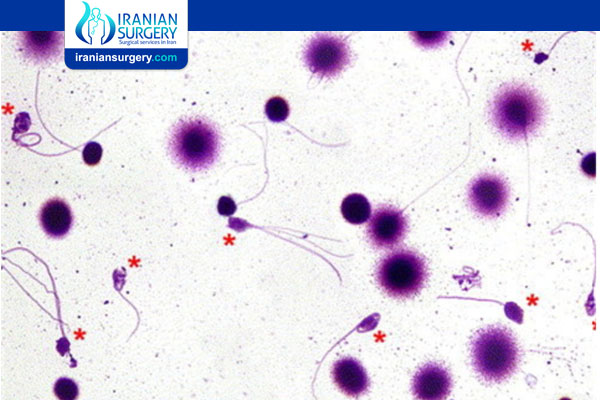
What is Sperm DNA Fragmentation?
DNA is the hereditary material in humans and other organisms and consists of two long chains—DNA strands—that are coiled around each other, each made of sugars and phosphate. The information in DNA is stored as a code made up of four types of molecules called bases, which are attached to the DNA strands like rungs on a ladder. Although all humans have the same bases, the order of these bases determines the information available for building and maintaining an organism. Just as different combinations of letters create different words and sentences, the unique sequence of these bases makes your DNA different.
Sperm DNA fragmentation occurs when there is a change in the bases or a physical break in one or both of the DNA strands of the chromosomes contained within the sperm.
What Does Testing for Sperm DNA Fragmentation Involve and Who Should Have It Performed?
There are many different tests for sperm DNA fragmentation, but the most commonly studied ones are the sperm chromatin structure assay (SCSA), the deoxynucleotidyl transferase-mediated dUTP nick end labeling assay (TUNEL), the single-cell gel electrophoresis assay (COMET), and the sperm chromatin dispersion test (SCD). These tests provide an estimate of the degree of DNA damage present in a semen sample. Testing for sperm DNA fragmentation is typically performed at an outside laboratory using a semen sample obtained through ejaculation.
Despite many studies investigating the utility of these DNA fragmentation tests, the 2013 American Society for Reproductive Medicine Practice (ASRM) committee opinion concluded that there was not enough data to support a consistent relationship between increased DNA fragmentation and reproductive outcomes. This is likely due to the fact that there are millions of sperm, and unless there is 100 percent DNA fragmentation present, it is unlikely that this is the sole cause for infertility.
Currently, there is not enough evidence that DNA fragmentation testing alone can predict pregnancy rates in the context of fertility treatment, and routine testing is not recommended at this time. As always, there are select populations for which this testing would be useful, and a reproductive urologist would be able to determine if this additional information would be helpful in formulating a treatment plan.
Source:
. https://progyny.com/education/how-to-test-for-sperm-dna-fragmentation/