Undescended Testicles
Undescended Testicles
What are Undescended Testicles?
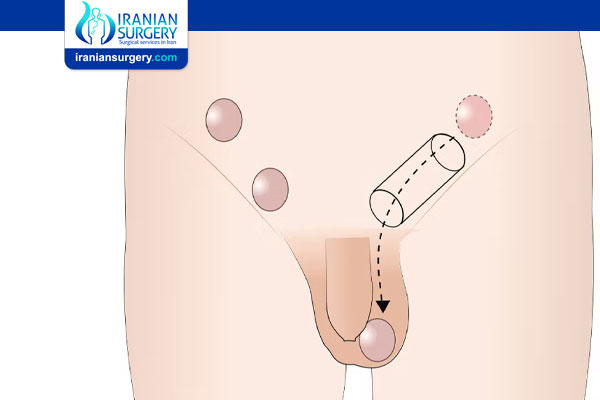
The testicles develop in the abdomen while a male baby is still in the uterus. Before birth, the testicles typically drop from inside the abdomen down into the scrotum. The scrotum is the sack of skin hanging behind the penis where the testicles are housed.
Undescended testicles fail to drop into the scrotum before birth or in the first few months of life. The condition is also called cryptorchidism.
Before Undescended Testicles Treatment
How common are undescended testicles?
About 3% of babies are born with undescended testicles, however the condition is much more common in premature babies (up to 30%). In about half of babies born with undescended testicles, the testicles descend on their own within a few months of life.
What are retractile testicles?
In some cases, the absence of testicles in the scrotum is a result of a muscle reflex. This condition is called retractile testicles. The reflex will pull the testicles out of the scrotum and back up into the body when he’s cold or scared. The reflex is temporary and usually resolves at puberty.
Retractile testicles naturally descend back into the scrotum. Your child’s healthcare provider can usually guide retractile testicles back into the scrotum during a physical exam. Retractile testicles don’t generally require surgery or other treatment.
What causes undescended testicles?
There is no clear reason why some babies are born with undescended testicles. In some cases, hormones could interfere with the testicles’ development.
The condition is more common in premature babies who haven’t had a full nine months to develop before birth. There is no evidence that anything a mother does while pregnant causes a baby to have undescended testicles.
What are the symptoms of undescended testicles?
Most babies and children with this condition have no symptoms. The only sign is that the scrotum is empty
What are the complications of undescended testicles?
After a boy goes through puberty, the testicles start producing sperm. To make healthy sperm, the testicles need to be two to three degrees cooler than the body’s core temperature. That’s why the testicles hang below the body, inside the scrotum.
If the testicles don’t drop into the scrotum, they may not function normally and produce healthy sperm. This can lead to infertility later in life.
Males born with undescended testicles also have a higher risk of testicular cancer in adulthood. If the testicles are in the abdomen and not down in the scrotum, this can make it more difficult to diagnose and treat.
Diagnosis and Tests
How are undescended testicles diagnosed?
Your child’s healthcare provider should physically examine your child’s testicles at each checkup. If the testicles are “non-palpable” (meaning the provider cannot feel them), they may be undescended.
Your healthcare provider may recommend following up with a pediatric urologist. An ultrasound may be recommended by the urologist, however they often are not necessary.
Prevention
How are undescended testicles prevented?
There is no known way to prevent this condition.
During Undescended Testicles Treatment
Management and Treatment
How are undescended testicles treated?
If your child’s testicles haven’t dropped into the scrotum by the time he’s six months old, talk to your healthcare provider about treatment. A pediatric urologist is a specialist who treats undescended testicles.
Undescended testicle treatment options include:
. Hormone therapy: In rare cases — especially when the testicles are near the scrotum — your healthcare provider may recommend hormonal treatment. The healthcare provider gives the child a series of hCG (human chorionic gonadotropin) injections. The hormones encourage the testicles to drop into the scrotum.
. Surgery: Surgery is the most common, and effective, treatment for undescended testicles. The procedure to move testicles down into the scrotum is called orchiopexy. It’s usually best for your child to have surgery between six months and one year old.
After Undescended Testicles Treatment
Outlook / Prognosis
What is the prognosis (outlook) for people with undescended testicles?
Surgery to fix undescended testicles is about 98% effective. In most cases, the testicles will develop normally in the scrotum. They produce healthy sperm later in life.
Boys who had undescended testicles continue to have a slighter higher risk of testicular cancer. Starting in their teens, they should perform monthly testicular self-exams and get routine checks by their healthcare provider.
When should I call my healthcare provider?
You should call your healthcare provider if your child experiences:
. Bleeding or signs of infection at surgical incision site.
. Severe pain in their groin.
. Side effects of hormonal treatment.
Source:
. https://my.clevelandclinic.org/health/diseases/17594-undescended-testicles