Retained Products of Conception (RPOC)
Retained Products of Conception (RPOC)
What are Retained Products of Conception?
Retained products of conception (RPOC) refers to tissue that remains in your uterus (womb) after a pregnancy ends. The tissue is usually from the placenta, which is an organ that develops in your uterus during pregnancy. However, this tissue can also be fetal tissue.
Retained placental or fetal tissue can happen after:
. Abortion (terminated pregnancy).
. Cesarean birth (C-section).
. Miscarriage.
. Vaginal delivery.
RPOC can cause bleeding and other health problems.
Before Retained Products of Conception Treatment
Are retained products of conception and a retained placenta the same thing?
Sometimes the entire placenta (also called “afterbirth”) remains in the womb after childbirth. A retained placenta can lead to hemorrhaging (bleeding), severe infection or even death.
A retained placenta most commonly happens after a vaginal delivery. But RPOC is more common when a pregnancy ends early. It may not cause problems until days, weeks or even months after the pregnancy ends.
Who is at risk of getting retained products of conception?
The following factors increase a woman’s risk of having RPOC:
. Placenta accreta (placenta attaches too deeply to the wall of the uterus).
. History of retained placenta in a previous pregnancy. This is the biggest risk.
. Advanced maternal age (older than 35 when pregnant).
. Assisted delivery (delivery using instruments such as forceps or vacuum).
. Delivery, miscarriage or abortion in the second trimester of pregnancy (weeks 13 to 26).
. Failure to progress (FTP) during delivery (prolonged labor lasting more than 14 hours).
. Prolonged use of oxytocin.
. Nulliparity (a woman who has never given birth before, though may have been pregnant).
. Past C-section.
. Past uterine surgery.
. Congenital uterine anomaly.
How common are retained products of conception?
RPOC is one of the most common reasons for postpartum (after birth) bleeding. Studies suggest it happens in up to 40% of second-trimester miscarriages or abortions. But it’s fairly rare in full-term pregnancies (a pregnancy that lasts about 40 weeks). It occurs in about 1% of these cases.
What causes retained products of conception?
The placenta is an organ that develops as a fetus grows in your uterus. It’s attached to the wall of your uterus. It delivers oxygen and nutrients to your baby through the umbilical cord.
The placenta and other tissues that develop during pregnancy naturally deliver from the uterus during childbirth. But in some cases, some of the tissue remains in your womb. RPOC prevent your uterus from returning to its pre-pregnancy state.
What are the symptoms of retained products of conception?
Your body goes through a lot of physical changes after pregnancy. Some bleeding and vaginal discharge are normal. But heavy bleeding or blood clots after pregnancy could indicate a problem.
Postpartum hemorrhage (vaginal bleeding after childbirth) is the most common symptom of RPOC. Other symptoms may include:
. Enlarged uterus.
. Fever.
. Hypomenorrhea (light or infrequent menstrual periods).
. Infection.
. Open ectocervix (the opening between vagina and uterus should be small or closed after pregnancy).
. Pelvic pain.
Diagnosis and Tests
How are retained products of conception diagnosed?
It can be difficult to diagnose RPOC based on symptoms alone. The symptoms may be similar to other postpartum health issues. The following exams and tests can confirm a diagnosis of RPOC.
Blood and tissue tests:
. Human chorionic gonadotropin (hCG) test: This test measures the amount of the hCG hormone in your blood. The placenta produces this hormone. RPOC may cause high hCG levels after pregnancy if pieces of the placenta are still in your uterus.
. Endometrial biopsy: During an endometrial biopsy, your healthcare provider removes a small piece of tissue from your uterus. They examine the tissue under a microscope. The presence of chorionic villi (placental tissue cells) means there is still placental tissue in your uterus. This procedure is rarely done. More commonly, your provider will look for tissue during a dilation and curettage (D&C) procedure. This procedure is also a treatment option for RPOC.
Imaging exams:
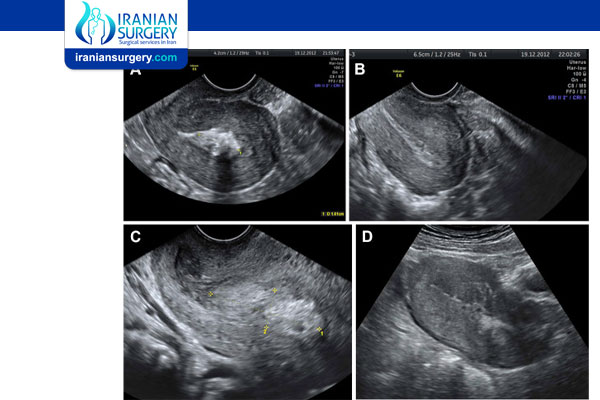
. Transvaginal ultrasound: This imaging exam uses an ultrasound probe in the vagina to check for an enlarged or thickened uterine lining. It also looks for tissue masses in your uterus.
. Color Doppler ultrasound: This imaging exam provides more detail than a transvaginal ultrasound. It shows how blood flows through your body. It can show whether extra tissue in the uterus still has a blood supply. A blood supply could indicate placental tissue still attached to the wall of the uterus.
. Hysteroscopy: During a hysteroscopy, your healthcare provider inserts a thin, lighted tube into your vagina. They examine the inside of your cervix and vagina for abnormal tissue or other problems.
Prevention
How can I prevent retained products of conception?
There’s no way to prevent RPOC. But you can make sure your healthcare provider knows your full medical history. You may be at a high risk for RPOC due to past pregnancy complications or surgeries. If that’s the case, your care team will monitor your health closely during and after any future pregnancies.
During Retained Products of Conception Treatment
Management and Treatment
How are retained products of conception treated?
There are several treatments for RPOC, including:
. Misoprostol: You may receive this drug by mouth or through your vagina. In pregnant women, it helps to induce labor. After an early pregnancy failure or an incomplete abortion, it triggers your body to expel (force out) retained tissue.
. Dilation and curettage (D&C): D&C is a minor surgical procedure to remove the contents of the uterus. Your healthcare provider dilates (opens) your cervix and uses a curette (small surgical tool) or suction to remove tissue.
Do these treatments have risks?
Misoprostol doesn’t carry any significant risks (significant bleeding can occur as complication from misoprostol, but this is very rare). D&C poses a greater risk than HR of:
. Bleeding.
. Infection.
. Perforation (making a hole) in the uterine wall.
. Intrauterine adhesions (uterine scarring).
Perforation is rare. The uterine wall usually heals on its own. If the perforation injures other organs, you may need surgery to repair them.
Uterine scarring, or Asherman’s syndrome, is rare, but can increase your risk of:
. Abnormal menstruation.
. Ectopic pregnancy.
. Infertility.
. Miscarriage.
. Postpartum hemorrhage.
. Premature labor or birth.
. Problems with the fetus or placenta.
After Retained Products of Conception Treatment
Outlook / Prognosis
Will I still be able to have children?
Most women who receive treatment for RPOC can still get pregnant and have healthy pregnancies. In rare cases, uterine scarring may cause fertility problems.
When should I call my doctor?
Seek immediate medical attention if you experience any of the following symptoms after a pregnancy:
. Difficulty breathing.
. Heavy vaginal bleeding.
. High fever.
. Nausea and vomiting.
. Severe pelvic pain.
Source:
. https://my.clevelandclinic.org/health/diseases/21512-retained-products-of-conception