Recovery after Prostatectomy
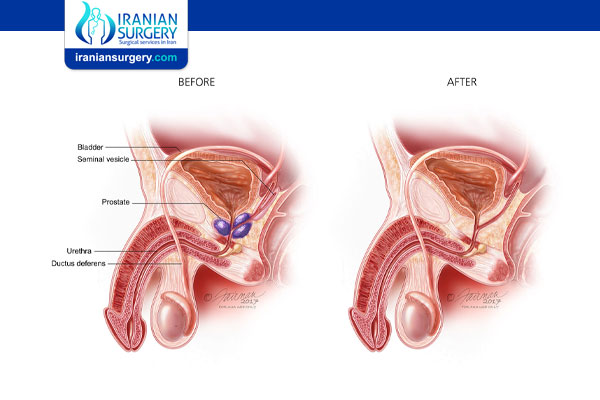
After Prostatectomy
You will wake up in the recovery room. You will have an oxygen mask on, as you will be breathing more slowly than usual while the anaesthetic wears off. You will have a drip in your arm to give you fluids and pain relief, and you will have a catheter in place to drain urine from your bladder.
You may also have a thin tube in your lower abdomen to drain fluid from the area where your prostate used to be. This is usually removed 24 to 48 hours after the operation.
Catheter
You’ll have a thin, flexible tube (called a catheter) passed up your penis to drain urine from your bladder while the area heals. It will be put in place during the operation, while you’re asleep. It may feel strange or uncomfortable at first and you may feel like you need to urinate all the time. But the catheter should drain all the urine without you needing to do anything, and this feeling usually passes after a few hours.
Most men go home with the catheter in. Your nurse will show you how to look after it, and it will be removed at the hospital one to three weeks later.
Pain
You will be given pain-relieving drugs after the operation if you need them. These should control any pain you have, but tell your doctor or nurse if you are in any pain.
The drugs are usually given into a vein in your arm or hand through a drip (intravenous infusion). You might have a pump so that you can give yourself pain relief without having to wait for someone to bring it to you. There is a limit on the pump so that you can't give yourself too much medicine by mistake.
Swelling
You may have some bruising and swelling in and around your testicles and penis. This can make it uncomfortable to sit on hard surfaces. It shouldn’t last more than a few weeks. If you have a lot of swelling, or if it’s getting worse, tell your doctor.
When you go home, you may find underpants (briefs) give you more support and are more comfortable than loose boxer shorts. You can also buy supportive underwear, such as a jock strap or testicle support.
If you had lymph nodes removed during the operation, this can very occasionally cause swelling in the scrotum (the skin containing your testicles) and one or both legs (lymphoedema). You will be given compression stockings to help encourage the fluid to drain from your legs if you need them.
Eating and drinking
Your team will let you know when it’s safe to start eating and drinking. You will usually start with sips of water.
Getting out of bed
You will be encouraged to get out of bed and start moving around as soon as you can to lower the risk of blood clots. You may also be prescribed injections to reduce the risk of blood clots.
You will go home one to five days after your operation, depending on your recovery and your doctor’s advice.
Going home
You will have the name of someone in your hospital team to contact in case there’s a problem after you go home. A district nurse might also visit you during the first few weeks.
Read more about : Prostate cancer treatment
Care of your catheter
Before you go home, your nurse will show you how to look after your catheter.
The catheter will be attached to a bag that can be worn inside your trousers, strapped to your leg. Make sure the tube isn’t bent or blocked, as this could stop urine draining into the bag.
The following tips can help prevent urine infections.
. Always wash your hands with warm, soapy water before and after touching your catheter.
. Wash the catheter and the area near the tip of your penis at least twice a day with warm water and unscented soap. Use one wash cloth for this and a different one for the rest of your body. Wipe downwards along the catheter, away from your body, and dry it carefully afterwards.
. Drink plenty of water (about 1.5 to 2 litres, or 3 to 4 pints a day).
. Eat plenty of fibre to avoid constipation (difficulty emptying your bowels) as this can stop the catheter draining properly.
Your catheter will be removed at the hospital one to three weeks after your surgery. Your doctor or nurse will make sure you can urinate before you go home.
You may notice some bleeding while the catheter is still in and just after it’s removed. This is quite common and usually stops on its own.
It’s common to leak urine when the catheter is removed. Take some absorbent (incontinence) pads and spare underwear and trousers to the hospital. Close-fitting underwear can help to keep the pads in place and men often find loose trousers most comfortable.
Your wound
After keyhole surgery, the cuts are usually closed with a special type of glue, clips or stitches. The cuts heal within a few days and the stitches slowly dissolve and fall out on their own.
If you have open surgery, the cut is usually closed with stitches or clips. Some types of stitches need to be removed in hospital or by your GP after one to two weeks.
The muscles and tissues inside your body need time to heal. This may take several months, and can sometimes take up to a year.
You will need to take it easy for the first couple of weeks after surgery. Gentle exercise around the home and a healthy diet will help your recovery. Light exercise such as a short walk every day will help improve your fitness. If you can, avoid climbing lots of stairs, lifting heavy objects or doing manual work for eight weeks.
Constipation
Bowel habits may take a few weeks to return to normal. You may have no bowel movements for several days after surgery. This is usually caused by the painkillers you’ll be taking.
If this carries on or becomes uncomfortable you may need medicine to help empty your bowels (called a laxative). Ask your pharmacist for some as soon as you start having trouble. It’s important you don’t strain.
Eating high fibre foods (such as wholegrains and fruit), drinking plenty of fluids, and doing gentle physical activity will help.
Feeling tired
Some men get fatigue (extreme tiredness) for a few weeks or months after surgery. This should pass with time. Try to eat healthily and be physically active when you feel able to.
Read more about : Cancer treatment
When to call your doctor
It’s important to tell your doctor if:
. Your bladder feels full or your catheter isn’t draining urine
. Your catheter leaks or falls out
. Your urine contains blood clots, turns cloudy, dark or red, or has a strong smell
. Your wound area or the tip of your penis becomes red, swollen or painful
. You have a fever (high temperature of more than 38ºC or 101ºF)
. You feel sick (nauseous) or vomit
. You get cramps in your stomach area that will not go away
. You get pain or swelling in the muscles in your lower legs.
. Your doctor or nurse will let you know if you should go to the hospital.
What happens next?
You will have regular check-ups after your operation – this is called follow-up. Your check-ups will usually start between six and eight weeks after surgery, and they will usually be every three to six months. Over time you may have these less often and two to three years after your treatment you may start seeing your GP instead of your hospital doctor.
PSA tests
You will have a PSA test a week before your check-up, so the results are available at the appointment. The PSA test is a good way of checking if your treatment has worked.
Your PSA level should drop so low that it’s not possible to detect it (less than 0.1 ng/ml). A rise in your PSA level can suggest some prostate cancer cells were left behind. If this happens, your doctor will talk to you about further treatment.
Looking at the prostate
Your prostate will be sent to a laboratory to be looked at under a microscope. This can give a clearer idea of how aggressive the cancer might be and whether it has spread.
At your first check-up your doctor might talk about ‘positive surgical margin’ or ‘negative or clear surgical margin’.
. Negative or clear surgical margin – this means that the tissue the surgeon removed was surrounded by a layer of normal tissue. It suggests all the cancer was removed.
. Positive surgical margin – this means there are cancer cells on the edge of the tissue the surgeon removed. It suggests that some cancer cells may have been left behind and you may need further treatment.
Read more about: prostate cancer treatments pros and cons
Further treatment
If your results suggest some cancer cells may have been left behind or the cancer has come back, you might be offered radiotherapy on its own or with hormone therapy. You may also be able to take part in a clinical trial.
Going back to work
The amount of time you take off work will depend on how quickly you recover, how much physical effort your work involves, and whether you feel ready to go back to work. If you have open surgery, you might need longer to get back to your usual activities.
Driving
You will be able to sit in a car as a passenger while your catheter is still in. You may want to avoid long journeys for the first two weeks after the catheter is removed until you are more used to dealing with any problems, such as leaking urine.
There are no official guidelines for how long you should wait before driving. Speak to your doctor about when it’s safe for you to drive.

