Ventricular Septal Defects (VSD)
Ventricular Septal Defects (VSD)
What is a Ventricular Septal Defect?
A ventricular septal defect is a condition where you're born with a hole in the wall between the two lower chambers of your heart. Often shortened to VSD, this condition is the most common congenital (meaning you have it when you're born) heart defect and often happens alongside other types of heart problems or defects. A small VSD is usually minor and has few or no symptoms. However, a larger hole may need to be repaired to avoid permanent damage and complications.
Before Ventricular Septal Defect Treatment
What happens inside my heart if I have a ventricular septal defect?
Your heart has four chambers. To pump blood efficiently, the chambers much seal shut. A VSD is a leak that disrupts that efficient pumping ability.
Under normal circumstances, the right ventricle pumps oxygen-poor blood that just arrived from your body out of your heart and into your lungs so the blood can pick up oxygen. The blood then returns to the heart, and its last stop in the heart is the left ventricle, which pumps oxygen-rich blood out to your entire body.
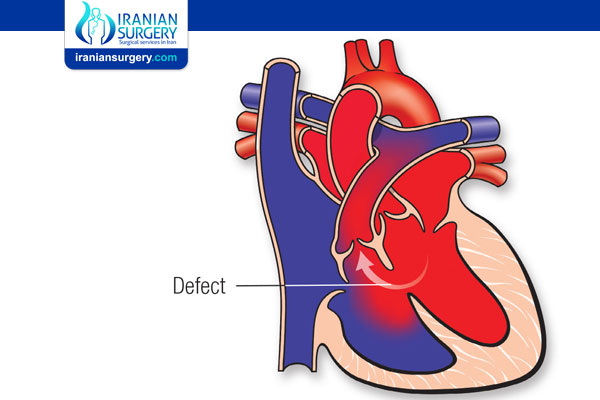
A VSD is a potential problem because it can act as a shunt (a connection) between the heart's two lower chambers, the left ventricle and the right ventricle. Because the pressure in the left ventricle is higher than the pressure in the right ventricle, oxygen-rich blood mixes with oxygen-poor blood in the right ventricle and then goes to the lungs. That leads to extra blood in the lungs which can cause serious problems.
Who does it affect?
Almost all VSDs are present at birth. A VSD diagnosis most likely happen during childhood, though adults can also receive this diagnosis. However, this only happens in 10% or less of cases. VSD is also slightly more likely to happen in premature babies and babies with certain genetic conditions.
In very rare cases, a heart attack can tear a hole between the ventricles and create a VSD. While this type of VSD — sometimes called ventricular septal rupture (VSR) — is technically a side effect, it is still a dangerous problem that needs to be repaired.
How common is this condition?
VSD happens in about one-third of 1% of all newborns. However, a VSD diagnosis in adults is much less likely because the defect closes on its own during childhood in 90% of cases.
VSDs that are a side effect of a heart attack are extremely rare, especially because of modern heart attack treatment methods. Today, it happens in less than 1% of all heart attacks.
What are the different types of VSD?
There are four main types of VSD, which differ in their location and the structure of the hole (or holes). The types of VSD are:
. Membranous: This is the most common type of VSD and makes up about 80% of cases. These VSDs happen in the upper section of the wall between the ventricles.
. Muscular: These account for about 20% of VSDs in infants, and there is often more than one hole that’s part of the defect.
. Inlet: This is a hole that happens just below the tricuspid valve in the right ventricle and the mitral valve in the left ventricle. That means when blood enters the ventricles, it must pass a VSD that connects the two chambers.
. Outlet (conoventricular): This kind of VSD creates a hole just before the pulmonary valve in the right ventricle and just before the aortic valve in the left ventricle, connecting the two chambers. That means blood has to go by the VSD on its way through both valves.
How does this condition affect my body?
VSD doesn't cause symptoms in most cases because the hole isn't large enough to cause problems. However, in cases where the hole is large enough (or if there are multiple holes), it can cause problems with blood leaking between the two chambers instead of circulating through the heart in the correct order.
That leaking makes your heart's pumping efforts less efficient, though if the leak is smaller, it may not be enough to cause any symptoms or problems. However, your heart needs to pump harder to compensate for the reduced blood flow when the leak is larger. When your heart works harder like that long-term, it can cause symptoms and problems in the heart and lungs that may become severe.
VSD size and effects
VSDs range in size from small to large, with the size playing a role in what effects — if any — the VSD will cause.
. Small (3 mm in diameter or less): Most VSDs fall in this category and don’t cause symptoms. About nine out of 10 of this type will close on their own by the time a child is 6 years old. Surgery for these is rare.
. Moderate (3-5 mm in diameter): These VSDs don’t usually cause symptoms. If they aren’t causing symptoms or problems elsewhere in the heart and lungs, delaying surgery is usually advised because some also close on their own.
. Large (6-10 mm in diameter): These VSDs often require surgery (the timing of the surgery can vary slightly). Repair of a large VSD before age 2 can prevent damage to the heart and lungs. Without repair before age 2, the damage becomes permanent and gets worse over time.
When a moderate or large VSD is not treated in time, Eisenmenger syndrome can develop. This is a condition where long-term damage to blood vessels in the lungs forces oxygen-poor blood from the right ventricle through a large VSD and into the left ventricle. That means some of the blood pumped to the body doesn't contain enough oxygen. That causes an overall oxygen shortage throughout the body. This condition is typically severe and can have major consequences on a person’s life and the activities in which they can participate.
The left ventricle has greater pumping strength than the right, which means it can force blood into the right ventricle. The right ventricle can’t push the extra blood back, so the extra blood instead gets pumped into the lungs. That puts too much pressure on and damages the lung’s blood vessels. Over time, the damage in the lung’s blood vessels starts to force the leak in the heart to reverse direction, forcing oxygen-poor blood from the right ventricle into the left.
Once the direction of the leak reverses, the damage is permanent and repairing the hole will cause right-sided heart failure. Surgical repair of a moderate or large VSD before age 2 is vital to prevent permanent damage and developing Eisenmenger syndrome.
What are the symptoms?
In infants, moderate to large VSD causes symptoms that look like heart failure. These include:
. Shortness of breath, including fast breathing or struggling to breathe.
. Sweating or fatigue during feeding.
. Failure to thrive (slow weight gain).
. Frequent respiratory infections.
VSD in older children and adults can cause the following:
. Feeling tired or out of breath easily when exercising.
. Slightly higher risk of heart inflammation caused by infections.
. After Eisenmenger syndrome develops, very pale skin or a bluish tinge to skin and lips (a condition called cyanosis) may happen.
What causes the condition?
VSD that's present at birth doesn't currently have any known causes. However, it does sometimes happen along with other heart defects, heart conditions or genetic disorders. Taking certain anti-seizure medications (sodium valproate and phenytoin) or drinking alcohol during pregnancy may also increase the risk of your child developing a VSD. However, it will take more research to confirm if these are definite causes.
The only known cause of VSD is when it happens as a rare side effect of a heart attack.
Diagnosis and Tests
How is it diagnosed?
A physician can diagnose a VSD — especially when they’re moderate- or large-sized — based on a combination of symptoms, a physical exam and imaging tests. A minor VSD may go undetected when the hole is too small to cause signs or symptoms.
A physical exam is one of the most common ways for a doctor to discover a VSD. That’s because a VSD — when it’s large enough —causes a sound called a heart murmur that your doctor can hear when listening to your heart with a stethoscope. It’s even possible to estimate the size of the defect from the sound of a murmur.
What tests will be done to diagnose this condition?
Other tests that help diagnose VSD include the following imaging tests:
. Echocardiogram: This test sends ultra-high-frequency sound waves through your body from a device held against the skin of your chest. Those sound waves create a picture of the inside and outside of the heart. Depending on the size of the VSD and its exact location, it’s likely to be visible on an echocardiogram. This test is also painless and only takes minutes to complete.
. Electrocardiogram (ECG or EKG): This test uses multiple sensors attached to the skin of your chest to detect the electrical activity of your heart. That activity appears as a wave on a printout or digital display for a healthcare provider to review and interpret. Over time, your heart structure can change because of a VSD. When the structure changes, the electrical pattern also changes. However, this test will often be normal if the VSD isn’t large enough or if the heart hasn’t started to change shape.
. Chest or heart X-ray: When a VSD is large enough, it will cause the structure of your heart to change. That change is visible on certain types of chest or heart X-rays. In some cases, it also involves injecting a substance into the blood that is easily visible on X-rays, which allows healthcare providers to see any unusual blood circulation that indicates a VSD or other problem.
. Computed tomography (CT) scan: This test uses a computer to process X-ray images into a three-dimensional picture of the inside of the heart. Like with a chest or heart X-ray, an injectable substance that’s highly visible on a CT scan may help.
. Cardiac catheterization: This procedure uses a catheter device to look at the heart from the inside. A specialist inserts the device into a major blood vessel, usually one near your upper thigh, and then passes it up to your heart. Once inside your heart, it can help pinpoint the size and location of any problems like a VSD. The most likely reason to use this test is when a healthcare provider suspects blood vessel damage in the lungs.
What are the possible complications or side effects of the treatments?
In general, your healthcare provider is the best person to explain the potential risks, complications and side effects that are possible with a VSD or related procedures and treatments. This is especially true for any recommended medications.
Common side effects or complications from surgery or transcatheter procedures for a VSD include:
. Bleeding.
. Infections, especially heart infections within the first six months after surgery.
. Disruption of nearby heart valves, causing them to leak.
. Heart rhythm problems (arrhythmias and heart blocks), which might lead to implantation of a pacemaker or indefinite treatment with medication.
. Follow-up surgery to close a recurring hole.
Prevention
How can I prevent this condition or reduce my risk?
Because there aren’t any known causes for VSD, prevention isn’t usually possible. However, you can decrease the risk by avoiding alcohol use and certain anti-seizure medications during pregnancy.
During Ventricular Septal Defect Treatment
Management and Treatment
How is it treated, and is there a cure?
The majority of VSDs are too small to cause any kind of problem, and they will likely close on their own by age 6. In those cases, a healthcare provider is likely to recommend against surgery, advise monitoring for symptoms and see if the defect closes independently. When VSDs are moderate-sized or larger, your doctor will likely recommend repairing the VSD by closing the hole.
The two main ways to repair a VSD are:
. Surgery: The most reliable way to close a VSD is to patch it surgically. To do this, a cardiac (heart) surgeon will operate and patch or close the hole. Depending on the size and location of the hole, it may be as simple as stitching the hole shut. In other cases, it might involve a patch made of a synthetic material or a graft of your own tissue.
. Transcatheter procedures: Like cardiac catheterization, these procedures use a transcatheter (catheter-based) approach to access the heart via a major artery. Once the catheter device reaches the defect, it can place a specialized device called an occluder and plug the hole. These devices are typically made of a mesh framework covered in a synthetic material.
In either of the above cases, your heart tissue will grow over and around the patch or occlude device. Ultimately, the patch or device should become part of the heart wall between the ventricles.
In cases where an infant or child is underweight or isn’t growing at the expected rate, their healthcare provider may recommend special measures to help them get enough nutrition. This might include a special diet or even a feeding tube.
What medications/treatments are used?
Medication can treat symptoms of a VSD before surgery or if the VSD is likely to close on its own over time. Common medications for VSD are often the same as those that treat heart failure. They include:
. Diuretics: These medications increase the amount of fluid your kidneys remove from your body. This is helpful when fluid is building up around your heart, a common effect of heart failure. These medications may make you urinate (pee) more often.
. Heart failure medications: These medications help control the strength and timing of your heartbeats. An example is digoxin, a common medication in the treatment of heart failure that is also helpful for VSD.
After Ventricular Septal Defect Treatment
How soon after treatment will I feel better, and how long does it take to recover from this treatment?
Recovery from repair of a VSD depends on the method used. Transcatheter procedures have shorter recovery times, with recovery times measured in days or weeks. Surgeries have longer recovery times, measured in weeks or months. Symptoms of a VSD usually decrease or disappear after surgery or transcatheter repairs.
Outlook / Prognosis
What can I expect if I have this condition?
Most adults with a VSD don't know about it because it isn't large enough to cause any problems. However, the larger the VSD, the more likely it will affect how you live your life, especially if it isn't repaired.
How long does a VSD last?
Approximately 90% of VSDs will close on their own by the time a person turns 6 years old. Most of the remaining 10% of VSDs will close by age 20. However, a VSD is unlikely to close on its own after that.
An adult with a VSD will have it for the rest of their life unless they undergo a procedure to repair it.
What’s the outlook for this condition?
Most people with a VSD have the same life expectancy as someone who doesn't have one. This is especially true if the defect closes on its own.
In cases of a moderate or large VSD, repair of the hole is usually enough to prevent Eisenmenger syndrome and related problems. In rare cases, a follow-up surgery becomes necessary to close new leaks around the repair. Unfortunately, most people with a moderate or large VSD — even one that’s repaired —are more likely to have a lower life expectancy, especially if the VSD was not repaired early.
For people who have a VSD that isn’t repaired, about 87% of them will be alive 25 years after their diagnosis. The size of the VSD has a major effect on the odds of survival, however.
. Small: Small VSDs are unlikely to have a major impact on your life. Overall, 96% of people with an unrepaired small defect live more than 25 years after diagnosis.
. Moderate: Survival rates for people with unrepaired moderate VSDs are a little bit lower, with about 86% of them surviving at least 25 years after diagnosis.
. Large: Survival rates for people with a large unrepaired VSD are much lower. Only about 61% of these individuals are still alive 25 years after their diagnosis.
People who develop Eisenmenger syndrome from a moderate or large VSD tend to have the worst survival outlook. Only about 42% of these individuals will be alive at least 25 years after their diagnosis with a VSD. However, advancements in modern medicine are improving the outlook for individuals with this condition and some live to be in their 70s.
How can I take care of myself and manage my symptoms?
Overall, you should ask your healthcare provider for guidance on managing your symptoms and taking care of yourself. Their advice will be best suited to you because they can see the overall picture of your health and medical situation and tailor the guidance they give you accordingly.
If you have symptoms because of a VSD, your healthcare provider will likely advise you to rest and avoid too much physical activity or any activity that puts too much strain on your heart. This is especially true if you have Eisenmenger syndrome related to an untreated VSD. You should also be sure to take medications exactly as instructed and only change or stop taking medications if you have talked to your healthcare provider and they have confirmed it's safe to do so.
When should I see my healthcare provider?
When you don’t know about a VSD
If you have an infant that doesn’t have a VSD that you know of, you should talk to their healthcare provider if you notice any of the following symptoms:
. Slower than expected growth or weight gain.
. Sweating or getting tired while feeding.
. If they are very fussy or show signs of trouble breathing.
. If they have frequent respiratory infections.
If you are an adult and aren’t aware that you have a VSD, you should talk to your healthcare provider if you notice that you get tired or short of breath easily when you’re physically active, or if you are often pale or notice a blue tint to your fingertips or lips.
When you know about a VSD
If your child has a VSD, their healthcare provider can advise you on potential signs and symptoms of VSD-related problems. In general, look for the same symptoms of VSD that are described above. You should also talk to their healthcare provider if you notice any sudden or unusual changes in their existing symptoms.
If you have a VSD, you should also talk to your healthcare provider if you have any sudden changes in your symptoms. You should also talk to a healthcare provider about your condition before you have any surgery or dental work to make sure they know about your condition.
When should I go to the ER?
Your healthcare provider or the provider caring for your child can explain when you should get emergency medical care for symptoms that are or might be related to a VSD. In general, you should go to the emergency room if you or your child have trouble breathing or any signs of cyanosis (pale or bluish skin, lips or fingernails).
Source:
. https://my.clevelandclinic.org/health/diseases/17615-ventricular-septal-defects-vsd