Scoliosis
Scoliosis
What is Scoliosis?
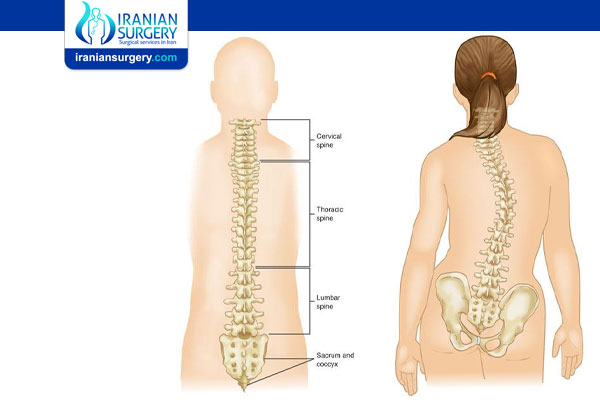
Scoliosis is a sideways curvature of the spine that most often is diagnosed in adolescents. While scoliosis can occur in people with conditions such as cerebral palsy and muscular dystrophy, the cause of most childhood scoliosis is unknown.
Most cases of scoliosis are mild, but some curves worsen as children grow. Severe scoliosis can be disabling. An especially severe spinal curve can reduce the amount of space within the chest, making it difficult for the lungs to function properly.
Children who have mild scoliosis are monitored closely, usually with X-rays, to see if the curve is getting worse. In many cases, no treatment is necessary. Some children will need to wear a brace to stop the curve from worsening. Others may need surgery to straighten severe curves.
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best Surgeons to treat your Scoliosis in Iran. The price of Scoliosis Treatment in Iran can vary according to each individual’s case and will be determined by an in-person assessment with the doctor.
For more information about the cost of Scoliosis Treatment in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number 0098 901 929 0946. This service is completely free.
Before Scoliosis Treatment
Symptoms
Signs and symptoms of scoliosis may include:
. Uneven shoulders
. One shoulder blade that appears more prominent than the other
. Uneven waist
. One hip higher than the other
. One side of the rib cage jutting forward
. A prominence on one side of the back when bending forward
With most scoliosis cases, the spine will rotate or twist in addition to curving side to side. This causes the ribs or muscles on one side of the body to stick out farther than those on the other side.
When to see a doctor
Go to your doctor if you notice signs of scoliosis in your child. Mild curves can develop without you or your child knowing it because they appear gradually and usually don't cause pain. Occasionally, teachers, friends and sports teammates are the first to notice a child's scoliosis.
Causes
Doctors don't know what causes the most common type of scoliosis — although it appears to involve hereditary factors, because the disorder sometimes runs in families. Less common types of scoliosis may be caused by:
. Certain neuromuscular conditions, such as cerebral palsy or muscular dystrophy
. Birth defects affecting the development of the bones of the spine
. Previous surgery on the chest wall as a baby
. Injuries to or infections of the spine
. Spinal cord abnormalities
Risk factors
Risk factors for developing the most common type of scoliosis include:
. Age. Signs and symptoms typically begin in adolescence.
. Sex. Although both boys and girls develop mild scoliosis at about the same rate, girls have a much higher risk of the curve worsening and requiring treatment.
. Family history. Scoliosis can run in families, but most children with scoliosis don't have a family history of the disease.
Complications
While most people with scoliosis have a mild form of the disorder, scoliosis may sometimes cause complications, including:
. Breathing problems. In severe scoliosis, the rib cage may press against the lungs, making it more difficult to breathe.
. Back problems. People who had scoliosis as children may be more likely to have chronic back pain as adults, especially if their abnormal curves are large and untreated.
. Appearance. As scoliosis worsens, it can cause more noticeable changes — including uneven hips and shoulders, prominent ribs, and a shift of the waist and trunk to the side. Individuals with scoliosis often become self-conscious about their appearance.
Diagnosis
The doctor will initially take a detailed medical history and may ask questions about recent growth. During the physical exam, your doctor may have your child stand and then bend forward from the waist, with arms hanging loosely, to see if one side of the rib cage is more prominent than the other.
Your doctor may also perform a neurological exam to check for:
. Muscle weakness
. Numbness
. Abnormal reflexes
Imaging tests
Plain X-rays can confirm the diagnosis of scoliosis and reveal the severity of the spinal curvature. Repeated radiation exposure can become a concern because multiple X-rays will be taken over the years to see if the curve is worsening.
To reduce this risk, your doctor might suggest a type of imaging system that uses lower doses of radiation to create a 3D model of the spine. However, this system isn't available at all medical centers. Ultrasound is another option, although it can be less precise in determining the severity of the scoliosis curve.
Magnetic resonance imaging (MRI) might be recommended if your doctor suspects that an underlying condition — such as a spinal cord abnormality — is causing the scoliosis.
During Scoliosis Treatment
Treatment
Scoliosis treatments vary, depending on the severity of the curve. Children who have very mild curves usually don't need any treatment at all, although they may need regular checkups to see if the curve is worsening as they grow.
Bracing or surgery may be needed if the spinal curve is moderate or severe. Factors to be considered include:
. Maturity. If a child's bones have stopped growing, the risk of curve progression is low. That also means that braces have the most effect in children whose bones are still growing. Bone maturity can be checked with hand X-rays.
. Severity of curve. Larger curves are more likely to worsen with time.
. Sex. Girls have a much higher risk of progression than do boys.
Braces
If your child's bones are still growing and he or she has moderate scoliosis, your doctor may recommend a brace. Wearing a brace won't cure scoliosis or reverse the curve, but it usually prevents the curve from getting worse.
The most common type of brace is made of plastic and is contoured to conform to the body. This brace is almost invisible under the clothes, as it fits under the arms and around the rib cage, lower back and hips.
Most braces are worn between 13 and 16 hours a day. A brace's effectiveness increases with the number of hours a day it's worn. Children who wear braces can usually participate in most activities and have few restrictions. If necessary, kids can take off the brace to participate in sports or other physical activities.
Braces are discontinued when there are no further changes in height. On average, girls complete their growth at age 14, and boys at 16, but this varies greatly by individual.
Surgery
Severe scoliosis typically progresses with time, so your doctor might suggest scoliosis surgery to help straighten the curve and prevent it from getting worse.
Surgical options include:
. Spinal fusion. In this procedure, surgeons connect two or more of the bones in the spine (vertebrae) together so they can't move independently. Pieces of bone or a bone-like material are placed between the vertebrae. Metal rods, hooks, screws or wires typically hold that part of the spine straight and still while the old and new bone material fuses together.
. Expanding rod. If the scoliosis is progressing rapidly at a young age, surgeons can attach one or two expandable rods along the spine that can adjust in length as the child grows. The rods are lengthened every 3 to 6 months either with surgery or in the clinic using a remote control.
. Vertebral body tethering. This procedure can be performed through small incisions. Screws are placed along the outside edge of the abnormal spinal curve and a strong, flexible cord is threaded through the screws. When the cord is tightened, the spine straightens. As the child grows, the spine may straighten even more.
Complications of spinal surgery may include bleeding, infection or nerve damage.
Lifestyle and home remedies
There are no specific activities that are known to cause or correct scoliosis. In general, people with scoliosis have no restrictions regarding lifting or activities. General exercise or participating in sports may have the benefit of improving overall health and well-being.
Alternative medicine
Studies indicate that the following treatments for scoliosis don't help correct the curve:
. Chiropractic manipulation
. Soft braces
. Electrical stimulation of muscles
. Dietary supplements
After Scoliosis Treatment
Recovery and Postoperative Care
Spinal fusion for scoliosis is a major surgery. However, the surgery itself is only one part of a long process. While the patient will be able to return to some limited activities in two to four weeks, the full recovery period is typically at least 6 to 12 months of steady progress achieved by following a care plan outlined by the medical team.
Full recovery takes up to 12 months
When most people hear about a spinal fusion surgery, they may mistakenly think that the spine is fused during the surgery. Instead, this surgery sets the groundwork with rods, screws, and bone grafts for the spine to fuse gradually over a long period of time, a process that usually takes 6 to 12 months.
Patients can start to move around within a day or two after scoliosis surgery. The total hospital stay is typically four to seven days. Patients can return to school or a sedentary/desk job about two to four weeks after surgery, but activity needs to be limited while the bone is fusing.
Factors That Affect Recovery
Most patients who have surgery for idiopathic scoliosis—scoliosis with no clear cause—are teenagers or young adults. This age group tends to recover well from surgeries compared with people who are much older and have more pre-existing health issues.
Other factors that can negatively affect recovery include:
. Smoking. Nicotine is a known bone toxin that hampers bone growth. Smoking or any other form of nicotine—such as patches, gum, dipping, e-cigarettes, or secondhand smoke—will greatly increase the risk for the spinal fusion surgery to fail. While not an easy task, nicotine users should quit before having spinal fusion surgery.
. Obesity. Studies have shown that obese people have more complications during and after surgery compared with the rest of the population.
. Depression. People with depression tend to have delayed recoveries from surgery, in part because they are less likely to follow doctor’s orders, such as the prescribed activity levels and medication dosages.
The above is not a complete list of factors that can affect a patient’s recovery from scoliosis surgery. Doctors will assess the patient’s medical history and lifestyle when discussing the potential pros and cons of scoliosis surgery.
Return to Pre-Surgery Activities
Typically, patients can resume most of their pre-surgery activities 6 to 12 months after a thoracic fusion since fusing the thoracic and upper lumbar spine does not extensively change the biomechanics of the spine. Female patients who have recovered from scoliosis surgery can still become pregnant and deliver babies vaginally.
Pain Control in the Hospital
The patient will still have several attachments, such as monitors and intravenous lines. One of these attachments may be a patient-controlled analgesia (PCA) pump. If the patient starts to experience pain, he or she can press the PCA pump to deliver narcotic medication into the bloodstream and get relief.
By the second day after surgery, most of the attachments, such as IV tubes and drains, are removed from the patient’s body. Within three days after surgery, the narcotic pain medication can be taken orally instead of intravenously.
Before leaving the hospital, the patient will want to have a plan for how to get refills of the oral pain medication at home because new regulations make it tougher to quickly get refills on narcotics. A delay could result in being without the painkiller for a few days, which could lead to pain, reduced activity levels, and a slower recovery.
Incision Wound Care
A large bandage, called a surgical dressing, will cover the incision wound on the back for about the first day after surgery. When changed, it will be replaced by a smaller dressing. A nurse will check the wound every day to ensure it is staying dry and clean.
Showers may not be allowed the first few days after surgery. However, the patient can be given a sponge bath so long as the wound does not get wet.
Starting to Move Around Again
The day after the procedure, most people who have scoliosis surgery are able to briefly get out of bed and walk to a nearby chair with the help of a nurse or physical therapist. Some people take two or three days before feeling up to the challenge of getting out of bed.
It is normal for the patient to be hesitant or fearful before attempting to get out of bed the first time. The patient will likely be in some pain, as well as tired and possibly dizzy. However, even small amounts of moving around and walking will be important for starting the process of strengthening the back and regaining some flexibility.
During these first few days of recovery, medical professionals may need to use a sheet to help transfer the patient in and out of bed. The person will also practice the “log roll” technique of keeping the back straight and bent knees together while rolling into bed without twisting or bending the spine.
What to Eat and Drink
Due to the medications taken during scoliosis surgery, it will be a few days before the stomach and intestines start working again and food and beverages can be consumed. In the meantime, the patient will only be given some ice and/or sips of water.
Fluids will be given intravenously (IV) during this initial period. Once the doctors confirm that the stomach and intestines are starting to work again, small amounts of solid food can be tried.
Tobacco or nicotine in any form is not permitted during recovery because that would increase the likelihood for infection and decrease the chance for a successful fusion.
Ready to Return Home
Before patients are given clearance to leave the hospital and go home, they will have to be able to do the following:
Get in and out of bed without help. By this point, the patient should be able to use the log roll technique on his or her own.
. Show improvement in walking. The patient must have the ability to walk the hallways and even go up and down a few steps.
. Eat solid foods. Being able to have a bowel movement is a key indicator for whether the patient is ready to leave the hospital. If the stomach and intestines are not functioning normally, the patient will have to remain in the hospital until they do.
. Show no sign of infection. Some signs of infection could include fever, pus at the incision site, unusual swelling, or delayed healing. Anything that indicates an infection would delay the patient’s return home.
Once the patient is deemed safe to leave the hospital, he or she will be given a ride home by a friend or family member. The patient will not be permitted to drive until later in the recovery process.
When a patient returns home from scoliosis surgery, he or she will still be heavily medicated, weak, and in need of much rest. The patient will also have a list of precautions that must be strictly followed to protect and care for the healing spine.
During these first couple of weeks back at home, the patient will need the help of a friend, family member, or home health aide who can assist with some basic care and daily tasks. In addition, the patient will not be allowed to drive yet and should limit car rides.
No Bending, Lifting, or Twisting
The most basic of precautions for the patient during the recovery process will be “no BLTs.” These include:
. No bending. The patient is allowed to bend at the knees and hips, but not at the back.
. No lifting. Nothing should be lifted that is more than 8 pounds, which is about the weight of a gallon of milk. Someone else will need to handle tasks that require lifting more than that for now.
. No twisting. Even simple tasks often involve twisting the spine, but that motion will have to be restricted during recovery. For example, to avoid twisting (and bending) the spine while getting in and out of bed, the patient will need to use the “log roll” technique described on the previous page.
While it is important to follow these movement restrictions, it is normal for people to occasionally forget and move in a way that is not advised. This type of movement—bending, twisting, or lifting—will cause some additional pain during recovery and serve as a reminder not to move in that manner again.
Depending on the extent of the surgery, some surgeons may prescribe a back brace to be worn for part of the recovery period. If a brace has been prescribed, it will help the patient to avoid risky activities until the fusion and healing of the spine becomes more stable.
Pain Management Plan
A key component of recovering from scoliosis surgery is pain management, but it requires balance. On one hand, pain must be kept under control to enable the patient to concentrate on tasks and move around, which helps the recovery process. On the other hand, narcotic pain medication—which is strong and tends to control severe pain well—should not be taken for too long in order to reduce the risks of developing complications, such as addiction or other serious health problems.
It is advised that the patient go off narcotics as soon as he or she can effectively manage the pain with a weaker medication. Typically, a scoliosis surgery patient will transition off narcotic pain medication during the second week at home or shortly thereafter.
Acetaminophen (e.g. Tylenol) is frequently recommended as a pain medication that scoliosis surgery patients might switch to after being on narcotics. However, NSAIDs, such as ibuprofen, naproxen, or COX-2 inhibitors (e.g. Advil, Aleve, Celebrex, and Motrin) are usually avoided for the first three months, because they might interfere with bone growth and could cause the fusion to fail.
Most patients are completely off pain medication four to six weeks after surgery. Although, some patients might take considerably longer before being ready to go off pain medication.
Incision Site Care
It is important to maintain good care of the incision site. Every day, the patient will need to keep that area clean and dry. Typically, no creams, ointments, or powders are recommended.
When the patient first starts taking showers again, which is usually upon returning home, the incision site must be covered—such as with an occlusive dressing provided by the hospital or taped saran wrap—to prevent it from getting too wet.
Two to Four Weeks Post-Operation
During this time period, the patient will likely experience the following with permission from the surgeon:
. Start soaking in tubs if desired. Once the incision wound has healed, the patient is no longer at risk for bacteria to enter through the incision site and can be submerged in water again. If the patient prefers taking baths or just soaking in a tub or whirlpool, these activities can be resumed. However, great care must still be taken while getting in and out of a tub, and swimming should still be avoided.
. Return to school. If the patient is school-age, he or she can usually return to class within the first month after surgery. Activities such as gym class, exercise, and sports will usually require waiting a little longer. Most surgeons make these decisions on a case by case basis. Patients ease back into the rigors of school, so the first week back will probably just be half days. Also, some school districts offer home tutors who can help patients with their school work.
. Transition off narcotics. Most patients will be taken off narcotics (opioids) and switch to a weaker pain medication, such as acetaminophen (e.g., Tylenol), sometime between the two- and four-week mark. A few patients might take much longer to go off narcotics.
. Go out with friends. While friends have been allowed to visit the patient in the hospital and at home during the early stages of recovery, at about the four-week mark the patient can start going out with friends on a limited basis. However, the patient will need to be off narcotics before being cleared to go out with friends.
. Riding in vehicles. Except for doctor visits, car rides are discouraged during the early part of recovery because potholes and bumps in the road can cause the patient to bend or twist, which are to be avoided. As the patient’s recovery progresses, the doctor may give permission to ride in vehicles more often.
It should be reiterated that every patient is different, and no activity should be resumed without the doctor’s permission. For example, using a hot tub or spa before getting medical clearance is especially risky because they are more likely to contain harmful and resistant bacteria.
6 Weeks to 12 Weeks Post-Operation
At about six weeks, X-rays are taken to assess surgical healing and the fusion process. The patient will still not have normal energy levels, but the spine’s healing should be far enough along to permit activities.
If the patient has been moving around well enough and is off narcotics, he or she can also return to driving. Some surgeons recommend that the patient have physical therapy prior to driving in order for a therapist to assess level of pain, coordination, and reaction time.
Each individual has his or her own pathology and tolerates pain differently, so the timing can vary greatly in terms of when a patient can completely go off pain medication. Typically, patients will no longer need pain medication six weeks after scoliosis surgery.
If the patient has a job, he or she will likely be able to return to sedentary or desk work by the four- to six-week mark. However, it will probably take more than six weeks of recovery before jobs that are more strenuous can be resumed.
Keeping the spine aligned and getting plenty of rest were the top priorities in the first weeks and months after scoliosis surgery. After three months, the patient is usually given clearance to become more active and start doing moderate exercise again. This will probably include a physical therapy program to help strengthen back muscles and improve flexibility where possible.
Somewhere between the 6- and 12-month mark, the doctor will X-ray the spine again and note that the fusion has reached completion. Once the doctor verifies that the fusion has reached full strength, the patient is allowed to return to all activities with no restrictions.
Most activities that the patient had participated in prior to surgery should still be possible now. Although, depending on how much of the spine was fused, there could be some dance moves or gymnastic moves that are either no longer possible or must be done in a modified way due to some part of the back not bending. In addition, the patient may want to discuss high-impact activities with the surgeon, such as amusement park rides, bungee jumping, and full contact sports.
Even if the patient is given the OK to return to all activities, there are some habits that are to be continued for the rest of his or her life. These habits include sitting with good posture, bending at the knees when lifting heavy items, and not smoking.
Complete Recovery at One to Two Years
While the spinal fusion will reach completion within a year for most patients, any potential nerve trauma sustained during surgery may take up to two years to heal.
It is common for scoliosis surgery patients to experience some numbness in the back and/or legs immediately following the surgery, especially at the incision site. That numbness can linger for months but will likely be mostly or completely gone within a couple years.
Sources:
. https://www.mayoclinic.org/diseases-conditions/scoliosis/diagnosis-treatment/drc-20350721
. https://www.spine-health.com/treatment/back-surgery/scoliosis-surgery-postoperative-care