1How long does it take to recover from a discectomy?
1 to 4 weeks
The recovery time varies from 1 to 4 weeks depending on the underlying disease treated and your general health. You may feel pain at the site of the incision.
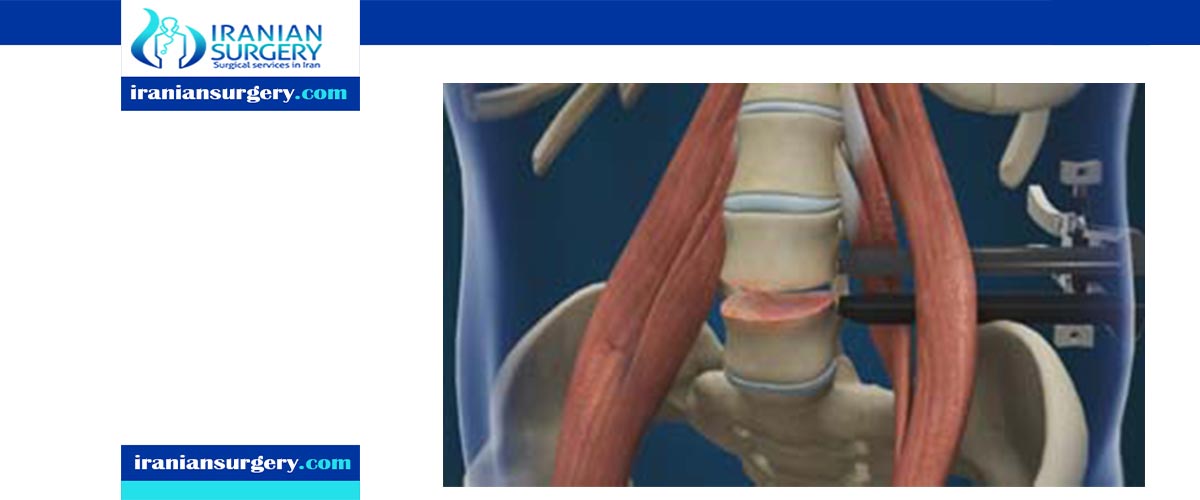
2What is lumbar discectomy surgery?
Discectomy is surgery to remove lumbar (low back) herniated disc material that is pressing on a nerve root or the spinal cord. It tends to be done as microdiscectomy, which uses a special microscope to view the disc and nerves. ... It allows the surgeon to better see the herniated disc.
3What is the success rate of a discectomy?
The success rate for microdiscectomy spine surgery is generally high, with one extensive medical study showing good or excellent results overall for 84% of people who have the procedure.
4Is a lumbar discectomy painful?
A bulging disc may press on the spinal cord or spinal nerves and cause leg pain and numbness. Your doctor made a 2.5 to 5 centimetre cut (incision) in the skin over the spine.
5Is walking good for herniated disc?
What Kind of Exercise to Do When You Have a Herniated Disc. You don't need to endure an intense cardio program or lift heavy weights—simple stretching and aerobic exercises can effectively control your herniated disc pain. ... Moderate aerobic activities, including walking, biking, and swimming, also help relieve pain.
6Does a discectomy weaken the back?
Chronic Low Back Pain: Removing a disc fragment that's compressing a nerve can be quite effective in relieving leg and buttock pain. This type of surgery, however, will not decrease low back pain. ... Sometimes surgeons will recommend a spinal fusion for persistent back pain after a discectomy.
7What happens if a bulging disc goes untreated?
An untreated, severe slipped disc can lead to permanent nerve damage. In very rare cases, a slipped disc can cut off nerve impulses to the cauda equina nerves in your lower back and legs. If this occurs, you may lose bowel or bladder control.
8Is Microdiscectomy major surgery?
Microdiscectomy is a very common, if not the most common, surgery performed by spine surgeons. The operation consists of removing a portion of the intervertebral disc, the herniated or protruding portion that is compressing the traversing spinal nerve root.
9Is a discectomy an outpatient surgery?
With the outpatient microdiscectomy low back surgery, patients are able to go home the same day as the surgery. Outpatient minimally invasive microdiscectomy surgery is usually done under general anesthesia. The patient is unconscious during the procedure and will not feel anything during surgery.
10How should I sleep after a lumbar discectomy?
John's Hopkins Orthopaedic Surgery recommends that if you lay on your back, slipping a pillow (or tightly rolled blanket) beneath your knees will help reduce any pressure. When sleeping on your back, try to avoid sleeping with your arms over your head because it will put stress on your shoulders and neck.