Knee Arthroscopy Complication
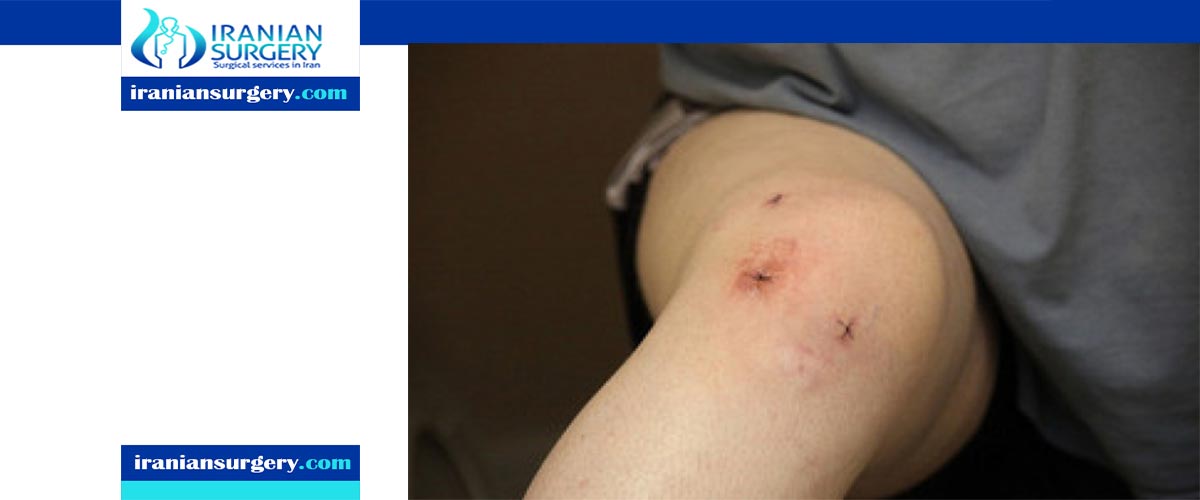
What are the risks of arthroscopic knee surgery?
How long does it take to fully recover from arthroscopic knee surgery?
How long should your knee hurt after arthroscopic surgery?
What is the success rate of arthroscopic knee surgery?
Knee arthroscopy is one of the most common surgical procedures worldwide. Knee arthroscopy is widely acknowledged to be a safe procedure. Still, there are also known serious complications such as joint infection, deep vein thrombosis, pulmonary embolism, and there are even deaths reported. For more complex arthroscopic procedures that involve ligament reconstruction, the risk of complication has been reported to be the highest followed by meniscal repair, chondroplasty, and meniscectomy. However, there is a substantial variation in the reported absolute risks for complications pyogenic arthritis between 0.08% and 0.42%, deep vein thrombosis between 0.12% and 41% and pulmonary embolism between 0.03% and 0.11%.
The possible complications following a knee arthroscopy include:
- Infection
- Thrombophlebitis (clots in a vein)
- Artery damage
- Excessive bleeding (haemorrhage)
- Allergic reaction to the anaesthesia
- Nerve damage
- Numbness at the incision sites
- Ongoing pain in the calf and foot.
Read more about: limb lengthening surgery
Read more about: Knee replacement surgery
Read more about: Knee Replacement Surgery Pain
What are the risks of arthroscopic knee surgery?
Common Risks
The overall risk of complications associated with knee arthroscopy has been estimated to be approximately 5 percent.
The likelihood of a serious complication resulting from knee arthroscopy is much less than 1 percent.
The most common risks of surgery are typically not life-threatening, but they can be an inconvenience. These risks include:
· Swelling
Swelling is a sign of inflammation within a joint. Often people undergoing knee arthroscopy have swelling of their joint before any surgical intervention. Sometimes, the knee swelling can be persistent after surgery, and may even worsen. Swelling can occur as a result of persistent inflammation within the joint, bleeding within the joint, or infection.
There are steps you can take to reduce swelling, including resting the knee joint, ice application, compression bandages, and elevating the extremity. However, for some people, the swelling becomes persistent and can be a frustrating source of discomfort following arthroscopic surgery. Worsening swelling can also be a sign of a more significant problem.
· Stiffness
Stiffness of the knee joint can occur as a result of scar tissue formation around the knee joint, or as a result of persistent swelling of the knee joint. Most people can find resolution of stiffness with appropriate therapeutic intervention following surgery.
However, for some people, the stiffness does not improve and can be a frustrating source of ongoing discomfort and disability after knee arthroscopy. Bending the knee and performing regular rehabilitation exercises in the early phase following surgery can help prevent excessive stiffness.
· Progression of Cartilage Damage
Many people who undergo arthroscopic knee surgery have some early damage to the cartilage of their knee joint. In general, arthroscopic surgery is not a good treatment for arthritis, and many people who have arthritis will have a progression of their condition.
Sometimes, people who have arthroscopic surgery can actually have a more rapid progression of arthritis following their surgical intervention.
There is also a medical condition called osteonecrosis that can spontaneously occur following arthroscopic surgery. This condition, abbreviated SONK (spontaneous osteonecrosis of the knee), can lead to a much more rapid deterioration of the knee joint cartilage, and ultimately may require knee replacement.
Less Common Risks
Uncommon risks of knee arthroscopy represent roughly 1% of people who undergo this surgical procedure. These are the risks that most people are concerned about, and fortunately, they are exceedingly infrequent following arthroscopic knee surgery. However, they can occur, and anyone who is considering arthroscopic knee surgery should be aware of the following possible complications:
· Infection
Infection is an unusual complication of knee arthroscopy, but it certainly can occur. Infection can either occur around the incisions, where it is considered a superficial infection, or it can occur within the knee joint, where it is a more serious, deeper infection.
When infection does occur, additional surgical procedures to clean out the infection may become necessary. Having bacteria within the knee joint can cause significant damage to the cartilage of the joint, and therefore urgent treatment of any suspected infection is necessary.
If the infection is only in the superficial area around the incision, sometimes antibiotics alone will be sufficient to cure the infection. When the infection is deeper within the knee joint, additional surgery in addition to antibiotics is typically necessary to eradicate the infection.
· Blood Clot
The risk of blood clots in the deep veins of the lower extremity is small after arthroscopic knee surgery, but it does occur. Blood clots can occur in anyone, but they are more common in people with specific risk factors for developing a clot.
One of these risk factors for developing a blood clot is lower extremity surgery with prolonged immobilization. For that reason, it is important to follow your doctor's advice and move your extremity as much as possible to keep blood flowing to the extremity and prevent the formation of blood clots.
For people with other risk factors (including smoking, oral contraception, clotting disorders, and others) additional precautions may be necessary.
· Death
The risk of mortality following knee arthroscopy is exceedingly small. In fact, the risk of mortality in patients undergoing knee arthroscopy has been found to be smaller than in the general population. This has been attributed to the fact that people undergoing arthroscopic surgery tend to be more active individuals.
The overall risk of mortality associated with arthroscopic knee surgery has been estimated at 0.008 percent within 30 days of the surgery.
Read more about : Herniated disk treatment
Read more about : Cycling after knee arthroscopy
How long does it take to fully recover from arthroscopic knee surgery?
Recovering from this type of knee surgery takes time and occurs in stages, just like with every surgical procedure. Depending on the physical health of the person in question, the exercise regime, overall lifestyle among other factors, recovery from arthroscopic knee surgery could take anywhere from two to six weeks.
The first three days after surgery involves some pain for anyone who has undergone the procedure, so people usually use crutches to assist with walking during this period. When the patient feels less pain, they then walk with a cane. With walking and leg strengthening exercises, most people regain normal use of their knee within four to six weeks. The swelling, pain, and limited motion ceases three to four months after the surgery.
Ultimately, the recovery period for those who have gone through this process varies per person, so it's not easy to predict how long it will take a particular individual to recover from the surgery completely.
Read more about : Knee arthroscopy orthobullets
Read more about : Hip replacement
How long should your knee hurt after arthroscopic surgery?
Here are some of the top reasons why your knee may hurt after having a knee scope.
Persistent Swelling
Arthroscopic surgery is a minimally invasive surgical procedure that is used to see inside your knee joint, and repair or remove any damage. While this all sounds gentle and noninvasive, it needs to be understood that your body will react to the trauma of surgery.
Persistent swelling is one of the most common symptoms after knee arthroscopy.
Swelling is a difficult problem to resolve, as there are many possible causes, some of these listed below. In addition, some patients who have an arthroscopic surgery have persistent swelling as a result of lingering inflammation from the trauma of surgery.
If more serious problems related to surgery, such as infection, have been eliminated, treatments of swelling may include:
- Ice application
- Anti-inflammatory medications
- Compression wraps and braces
- Physical therapy
- Knee Swelling
Infection
Infection is a very uncommon complication of arthroscopic surgery.3 But it is the complication most feared by patients. Typical symptoms of infection include:
- Persistent swelling
- The warmth of the joint
- Redness around the incisions or draining fluid
- Fevers, chills, or sweats
If the infection is untreated, there can be serious repercussions. Infection can damage the cartilage leading to the early onset of arthritis within a joint. As an infection persists, it can be more difficult to cure.
While an infection is an uncommon cause of pain after knee arthroscopy, it is one that needs to be the top of everyone's list to consider as early treatment is essential to have the best chance at recovery. Treatment of infection requires prolonged antibiotic treatment and can require additional surgery to clean out the joint.
Read more about : Knee Ligament Repair
Read more about : Hip replacement
Inadequate Rehabilitation
When people have a knee injury, such as a torn meniscus or cartilage damage, they can develop poor mechanics of the knee joint. In order to protect their joint and reduce pain, people often limp or develop an abnormal gait.5 Once the problem is taken care of, patients may need to correct these mechanical abnormalities of knee function.
In addition, some knee joint injuries are the result of poor mechanics of the extremity. Current research is focused on dynamic stability of the lower extremity in other words, how sturdy your knee is when subjected to normal forces and movements. Patients with dynamic instability may be more prone to injury and may require surgical treatment.
After surgery, your doctor may recommend specific rehabilitation to address weakness or gait abnormalities that may have caused an injury or be the result of having had an injury. Insufficient rehabilitation can be a cause of persistent knee pain after an injury.
Spontaneous Osteonecrosis
One complication that has been linked to knee arthroscopy is a condition called spontaneous osteonecrosis of the knee, or SONK.7 This condition is most often found in middle-aged women who have a knee arthroscopy. After their surgery, they develop persistent pain, typically along the inner (medial) side of the knee.
SONK is a condition that causes inflammation within the bone. While the condition is called osteonecrosis, a word that means there is spontaneous bone cell death, the problem has been thought to be the result of microscopic fracture of the bone around the knee joint.
These subchondral fractures cause inflammation within the bone and significant pain. The pain is typically worsened by activity and relieved by rest.
Treatment of SONK can be very frustrating, and many patients find the pain worse than the pain they had prior to arthroscopy. Eventually, that pain does settle down, but often the only way to find relief is to limit weight by using crutches for weeks or months after knee arthroscopy.
Braces and medications can also help with the symptoms. In some patients, the symptoms can be so severe that patients end up having either a partial knee replacement or full knee replacement.
Arthritis in the Joint
Probably the most common reason why patients have persistent pain after arthroscopic knee surgery is that their knee has damage to the cartilage of the joint that can't be adequately repaired by an arthroscopic procedure.
It is well established that typical arthritis pain does not warrant an arthroscopic surgery; numerous studies have shown that the benefit of arthroscopy in these patients is no better than with nonsurgical treatments.
However, there are times when patients with osteoarthritis may have problems that can improve with arthroscopic surgery, or your surgeon may not be aware of the extent of arthritis until the time of surgery.
In these cases, patients may have an arthroscopic surgery but may have to manage ongoing pain from arthritis that does not improve despite the surgical procedure. The good news is that there are many treatments for knee arthritis, and often these can help patients find relief from their symptoms.
What is the success rate of arthroscopic knee surgery?
Arthroscopic surgery has an approximately 90% success rate. Over time, the success rate diminishes following the surgery due to the impact of having less meniscus cartilage.
Read more about: Total Knee Replacement
Read more about: Knee Ligament Surgery Recovery
10 common question about knee arthroscopy complication
[kkstarratings]

