kidney stone surgery stent removal
Ureteric stent removal
What is a Ureteric Stent?
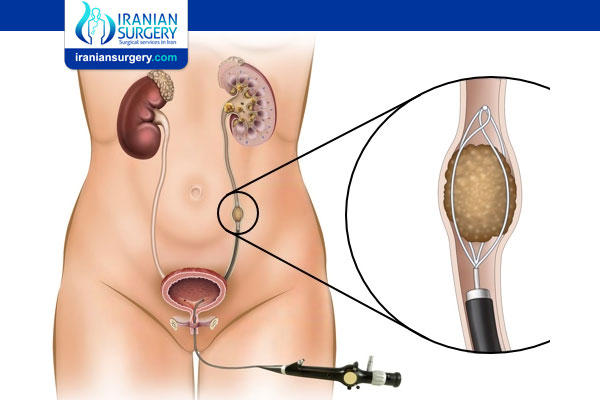
The ureter is a vital thin tube structure allowing the urine that is produced by the kidney, to drain into the bladder. If this tube becomes blocked, it can result in pain, life threatening infection and damage to the kidney. A ureteric stent is a plastic tube used to keep the kidney draining and prevent these problems. There are curls on each end to stop the stent from moving. Stents are temporary and in some circumstances, a small length of string is attached to the lower part of the stent to facilitate removal.
A ureteric stent is sometimes placed as an emergency to bypass an unexpected blockage in the ureter such as kidney stones. This is usually a temporary measure only to treat the blockage and you will be required to return after several weeks for a definitive procedure to breakdown and remove the stones.
A ureteric stent may also be inserted at the end of surgery involving your ureter. This is to protect you from blockage caused by swelling that occurs in the first few days after the procedure. Your surgeon should give you an indication of how long a stent is intended to stay in for, as the length of time can vary.
Read more about : kidney stone surgery complications
Read more about : Kidney Stone Surgery
How is the stent removed?
If you have had a stent inserted after kidney stone surgery, it is temporary and only needed for a short period of time. There are two main methods for removal.
. Stent on a string
For most patients, the stent will only stay in place for 5-7 days. In these cases, we often place the stent attached to a string which stays outside the body. The string can be gently pulled until the entire stent is removed. This is very quick and does not cause significant discomfort. This can be done at home yourself, or if you prefer, one of the medical team can do it for you in the hospital.
The stent is about 20-30 cm long with 2 curls on each end. A string is attached to the lower end as shown in the pictures below.
. Flexible Cystoscopy
If the stent is not attached to a string, the stent is removed by flexible cystoscopy in the outpatient department. Some local anaesthetic gel is used and a small camera is inserted into the bladder via your urethra (water pipe) by one of the urology staff. The end of the stent can then be grasped and pulled out. You will be given an appointment for this procedure.
Source:
. https://www.thh.nhs.uk/documents/_Patients/PatientLeaflets/urology/Having_a_Ureteric_Stent.pdf


1 Comment
The removal of a stent most certainly is painful and discomforting. It only takes a few moments but those moments are painful. This pain will subside over the next few days.