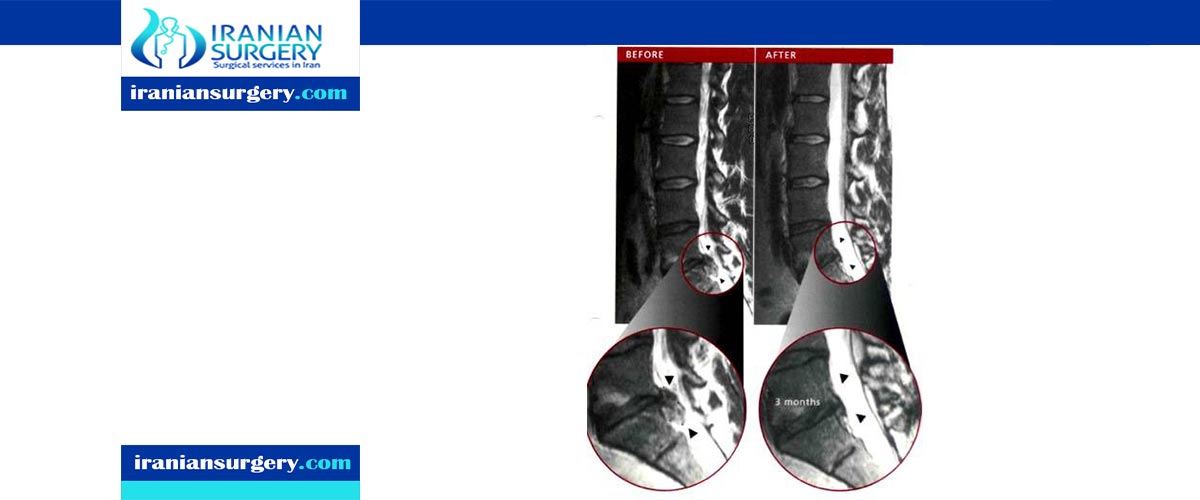
Disc Herniation Surgery Recovery
Overview
Lumbar discectomy is a surgery to remove a herniated or degenerative disc in the lower spine. The incision is made posterior, through the back muscles, to remove the disc pressing on the nerve. Discectomy may be recommended if physical therapy or medication fail to relieve leg or back pain or if you have signs of nerve damage, such as weakness or loss of feeling in your legs. The surgery can be performed in an open or minimally invasive technique.
Read more about : Femoral hernia recovery
What is lumbar discectomy?
Discectomy literally means "cutting out the disc." A discectomy can be performed anywhere along the spine from the neck (cervical) to the low back (lumbar). The surgeon reaches the damaged disc from the back (posterior) of the spine—through the muscles and bone. The surgeon accesses the disc by removing a portion of the lamina. The lamina is the bone that forms the backside of the spinal canal and makes a roof over the spinal cord. Next, the spinal nerve is retracted to one side. Depending on your particular case, one disc (single-level) or more (multi-level) may be removed.
A variety of surgical tools and techniques can be used to perform a discectomy. An “open” technique uses a large skin incision and muscle retraction so that the surgeon can directly view the area. A “minimally invasive” technique or a microendoscopic discectomy uses a small skin incision. A series of progressively larger tubes, called dilators, are used to tunnel through the muscles. Special instruments help the surgeon see and operate in a smaller space. A minimally invasive incision causes less disruption of the back muscles and may decrease recovery time. Your surgeon will recommend the technique most appropriate for your specific case.
A fusion may be done at the same time as discectomy to help stabilize the spine for patients who are athletes, perform heavy labor, or have spinal instability. Fusion uses a combination of bone graft and hardware (screws/plates) to connect two vertebrae together. During the healing process, the two vertebrae fuse into one piece of bone. Fusion is rarely needed for a herniated lumbar disc.
Do I Need Surgery?
Herniated disk surgery is an option if you're otherwise healthy but:
- You feel so much pain that you can't get around or do your daily activities.
- You have numbness or weakness from the disk pressing on nerves.
- You can't control your bladder or bowels.
- You have trouble standing or walking.
Before surgery
When considering surgery, make sure you see a qualified spine (orthopedic or neurosurgical) surgeon, and get a second opinion. Before recommending one surgical procedure over another, your surgeon will likely order imaging tests, which may include:
- X-ray: An X-ray produces clear pictures of your vertebrae and joints.
- Computed tomography (CT/CAT scan): These scans provide more detailed images of the spinal canal and surrounding structures.
- Magnetic resonance imaging (MRI): An MRI produces 3-D images of the spinal cord and nerve roots, as well as the discs themselves.
- Electromyography or nerve conduction studies (EMG/NCS): These measure electrical impulses along nerves and muscles.
Types of surgery for herniated disc
After gathering all the information they can, your surgeon may recommend one of these surgeries. In some cases, a person may require a combination of surgeries.
Laminotomy/laminectomy
In a laminotomy, a surgeon makes an opening in the vertebral arch (lamina) to relieve pressure on your nerve roots. This procedure is performed through a small incision, sometimes with the aid of a microscope. If necessary, the lamina can be removed. This is called a laminectomy.
Discectomy/microdiscectomy
Discectomy is the most common surgery used for herniated disc in the lumbar region. In this procedure, the portion of the disc that is causing the pressure on your nerve root is removed. In some cases, the entire disc is removed.
The surgeon will access the disc through an incision in your back (or neck). When possible, your surgeon will use a smaller incision and special instruments to achieve the same results. This newer, less invasive procedure is called microdiscectomy. In some cases, these procedures can be performed on an outpatient basis.
Artificial disc surgery
The disc is the soft cushioning structure located between the individual bones of the spine, called “vertebra.” It is made of cartilage-like tissue and consists of an outer portion, called the annulus, and an inner portion, called the nucleus (Figure 1). In most cases, the disc is flexible enough to allow the spine to bend.
An artificial disc (also called a disc replacement, disc prosthesis or spine arthroplasty device) is a device that is implanted into the spine to imitate the functions of a normal disc (carry load and allow motion).
There are many artificial disc designs classified into two general types: total disc replacement and disc nucleus replacement. As the names imply, with a total disc replacement, all or most of the disc tissue is removed and a replacement device is implanted into the space between the vertebra. With a disc nucleus replacement, only the center of the disc (the nucleus) is removed and replaced with an implant. The outer part of the disc (the annulus) is not removed.
Artificial discs are usually made of metal or plastic-like (biopolymer) materials, or a combination of the two. These materials have been used in the body for many years. Total disc replacements have been used in Europe since the late 1980s. The most commonly used total disc replacement designs have two plates. One attaches to the vertebrae above the disc being replaced and the other to the vertebrae below. Some devices have a soft, compressible plastic-like piece between these plates. The devices allow motion by smooth, usually curved, surfaces sliding across each other.
Most nucleus replacement devices are made of plastic-like (biopolymer) materials. One such material is called hydrogel. This material expands as it absorbs water. The device is placed into the nuclear cavity of the disc and hydrates to expand and fill the cavity. The device is compressible and by this means, allows motion, much like a normal disc nucleus. Another design consists of a piece of a plastic-like material that coils around to fill the nuclear cavity. No nuclear replacement devices are available for use in the United States at this time, even as a part of an FDA-approved study.
There are also disc replacements designed for use in the cervical spine (the neck). These devices have only been used a relatively short time, and several are currently undergoing evaluation in FDA-approved trials in the United States.
Spinal fusion
General anesthesia is required for spinal fusion. In this procedure, two or more vertebrae are permanently fused together. This may be accomplished with bone grafts from another part of your body or from a donor. It may also involve metal or plastic screws and rods designed to provide additional support. This will permanently immobilize that portion of your spine.
Spinal fusion usually requires a hospital stay of several days.
Your Recovery
Microdiscectomy is surgery to remove part or all of a bulging or damaged (herniated) disc in the lower spine. A herniated disc may press on the spinal nerves and cause pain and numbness in the buttock and leg.
Your doctor made a 3- to 5-centimetre cut (incision) in the skin over the spine. He or she put surgical tools through the incision and then used a special microscope (scope) to view the area.
You can expect your back to feel stiff or sore after surgery. This should improve in the weeks after surgery. You may have relief from your symptoms right away, or you may get better over days or weeks. In the weeks after your surgery, it may be hard to sit or stand in one position for very long. You may need pain medicine. It may take up to 8 weeks to get back to doing your usual activities.
Your doctor may advise you to work with a physiotherapist to strengthen the muscles around your spine and trunk. You will need to learn how to lift, twist, and bend so you don't put too much strain on your back.
This care sheet gives you a general idea about how long it will take for you to recover. But each person recovers at a different pace. Follow the steps below to get better as quickly as possible.
TIPS TO ENSURE A SPEEDY RECOVERY FROM HERNIATED DISC SURGERY
Once surgery has been performed, the road to recovery begins. It goes without saying that listening to your doctor’s instructions is the number one way to reduce recovery time after back surgery. Your doctor will carefully outline your recovery plan and you must follow it as directed. Below are some tips to help accelerate the process.
Get Plenty of Rest. Receiving the proper amount of rest is critical to a successful recovery from herniated disc surgery. Granted, this can be difficult to achieve with the discomfort you experience but try to build a sleep schedule and stick to it. If you feel yourself drifting in the middle of the day, distract yourself with some form of entertainment. This will make it easier to get an uninterrupted night of sleep.
Committ to Physical Therapy: Surgery is not the final step in addressing back pain. Following your surgery, you will spend at least a few weeks of physical therapy. Physical therapy is designed to help your body reach optimal recovery, but it can be very difficult. Ensure your follow your therapist’s instructions as closely as possible. This can help significantly speed up your recovery time.
Drink and Eat Properly. During your recovery time, your body is going to need additional calories to fuel its healing, but these extra calories do not need to come from fatty foods and sweets. Instead, eat a balanced diet in lean proteins and antioxidants to support tissue regeneration and ensure you’re receiving everything you need to heal optimally.
Avoid smoking and alcohol. Smoking and excessive drinking are not healthy habits for anyone, and this is especially true while recovering from herniated disc surgery. Smoking is specifically prohibited, especially if you’ve had spinal fusion surgery. Additionally, alcohol can have dangerous interactions with the pain medications you will need to take post-surgery.
Avoid activities that may prolong your recovery : Climbing stairs, lifting objects over a certain weight, or even walking too quickly before you’re ready can prolong your recovery time. Always err on the side of caution, and consider the use of devices such as walkers, shower seats, raised toilet seats, etc.
Take pain medication as directed. Proper pain control can make it far easier to sleep, which also promotes healing. Nevertheless, some patients hesitate to take their pain medication as prescribed because they fear addiction or other issues. Ensure you take your pain medication regularly, as directed. Wait too long, and you run the risk of waiting for a long period of time for the drug to take effect.
Pain
Immediately after surgery, you'll have some pain in and around the area where the operation was carried out. You'll be given pain relief to ensure you're comfortable and to help you move. The original leg pain you had before surgery usually improves immediately, but you should tell the nurses and your doctor if it doesn't.
A very small number of people have difficulty urinating after the operation. This is usually temporary, but in rare cases complications, such as nerve damage, may cause the legs or bladder to stop working properly. It's important to tell your doctor and nurses immediately if you have problems.
It can take up to 6 weeks for the general pain and tiredness after your operation to disappear completely.