Colectomy surgery in Iran
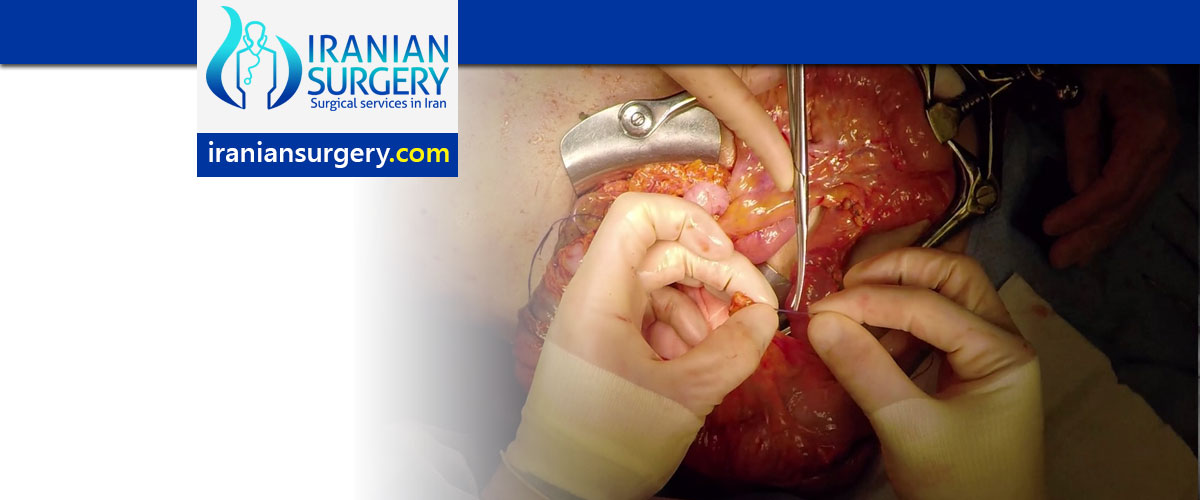
Colectomy surgery in Iran
Colectomy is a surgical procedure to remove all or part of the colon (also called the large intestine). It is performed in order to treat or prevent certain diseases and conditions such as uncontrollable bleeding in the colon, a bowel obstruction, colon cancer, ulcerative colitis, Crohn's disease, and diverticulitis.
There are different types of colectomies, which vary according to each patient. A total colectomy is the removal of the whole colon. A partial colectomy removes part of the colon. A hemicolectomy removes either the right or left section of the colon and a proctocolectomy removes both the colon and the rectum.
Types of colectomy surgery in Iran
Total colectomy involves removing the entire colon.
Partial colectomy involves removing part of the colon and may also be called subtotal colectomy.
Hemicolectomy involves removing the right or left portion of the colon.
Proctocolectomy involves removing both the colon and rectum.
Colectomy surgery usually requires other procedures to reattach the remaining portions of your digestive system and permit waste to leave your body.
Colectomy surgery cost in Iran
What affects the final cost of Colectomy surgery in Iran?
Qualifications/expertise of specialist
Incision location/type
Extent of surgery needed
The patient's general health
Minimally invasive surgery or open surgery
Colectomy surgery cost in iran start from $2800.
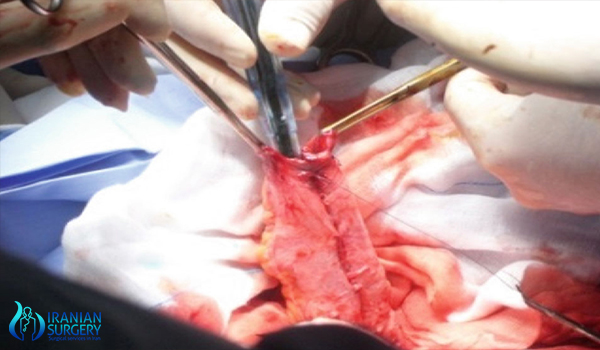
Why it's done?
Colectomy is used to treat and prevent diseases and conditions that affect the colon, such as:
Bleeding that can't be controlled. Severe bleeding from the colon may require surgery to remove the affected portion of the colon.
Bowel obstruction. A blocked colon is an emergency that may require total or partial colectomy, depending on the situation.
Colon cancer. Early-stage cancers may require only a small section of the colon to be removed during colectomy. Cancers at a later stage may require more of the colon to be removed.
Crohn's disease. If medications aren't helping you, removing the affected part of your colon may offer temporary relief from signs and symptoms. Colectomy may also be an option if precancerous changes are found during a test to examine the colon (colonoscopy).
Ulcerative colitis. Your doctor may recommend total colectomy if medications aren't helping to control your signs and symptoms. Colectomy may also be an option if precancerous changes are found during a colonoscopy.
Diverticulitis. Your doctor may recommend surgery to remove the affected portion of the colon if your diverticulitis recurs or if you experience complications of diverticulitis.
Preventive surgery. If you have a very high risk of colon cancer due to the formation of multiple precancerous colon polyps, you may choose to undergo total colectomy to prevent cancer in the future. Colectomy may be an option for people with inherited genetic conditions that increase colon cancer risk, such as familial adenomatous polyposis or Lynch syndrome.
Discuss your treatment options with your doctor. In some situations, you may have a choice between various types of colectomy operations. Your doctor can discuss the benefits and risks of each.
Risk of Colectomy surgery
Colectomy carries a risk of serious complications. Your risk of complications is based on your general health, the type of colectomy you undergo and the approach your surgeon uses to perform the operation. In general, complications of colectomy can include:
Bleeding
Blood clots in the legs (deep vein thrombosis) and the lungs (pulmonary embolism)
Infection
Injury to organs near your colon, such as the bladder and small intestines
Tears in the sutures that reconnect the remaining parts of your digestive system
You'll spend time in the hospital after your colectomy to allow your digestive system to heal. Your health care team will also monitor you for signs of complications from your surgery. You may spend a few days to a week in the hospital, depending on your condition and your situation.
Before colectomy surgery in Iran
During the days leading up to your colon surgery, your doctor may ask that you:
Stop taking certain medications. Certain medications can increase your risk of complications during surgery, so your doctor may ask that you stop taking those medications before your surgery.
Fast before your surgery. Your doctor will give you specific instructions. You may be asked to stop eating and drinking several hours to a day before your procedure.
Drink a solution that clears your bowels. Your doctor may prescribe a laxative solution that you mix with water at home. You drink the solution over several hours, following the directions. The solution causes diarrhea to help empty your colon. Your doctor may also recommend enemas.
Take antibiotics. In some cases, your doctor may prescribe antibiotics to suppress the bacteria found naturally in your colon and to help prevent infection.
Preparing for colectomy isn't always possible. For instance, if you need an emergency colectomy due to bowel obstruction or bowel perforation, there may not be time to prepare.
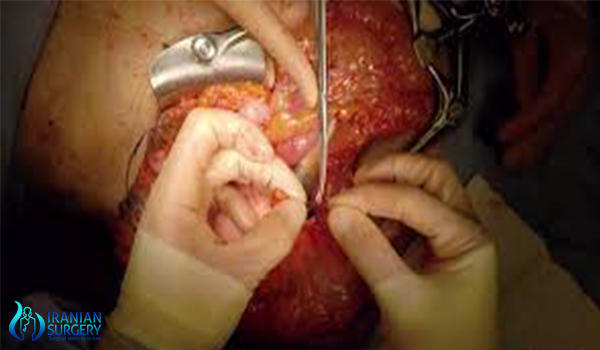
During colectomy surgery
There are a number of methods of performing a colectomy and this will be discussed with the doctor beforehand. The colon may be removed in its entirety, partially removed or removed to repair it and then reinserted.
An open colectomy involves making a long incision in the abdomen to access the colon. The surgeon uses tools to free the colon from the surrounding tissue, and will then cut a portion of the colon, or the entire colon out.
In a laparoscopic colectomy, or a minimally invasive colectomy, the surgeon makes several small incisions in the abdomen. Using a small camera threaded through one incision and using surgical tools through the other incisions, the colon is lifted out. This allows the surgeon to operate on the colon outside of the body without making large incisions. Once repairs are made to the colon, the surgeon reinserts the colon through the incision.
After the colon has been removed or repaired, the surgeon will then reconnect the colon to the digestive system in order to restore the function of getting rid of waste. How this reconnection is made, varies upon the type of removal or repair which has been carried out.
If there has been a partial removal of the colon, then the remaining sections will be stitched back together and the disposal of waste will resume as normal. Another method of reconnection, is to join the intestine to the abdomen via an opening. This involves the attachment of the colon to the small intestine which enables the body to dispel waste via the opening. After this reconnection, it may be necessary to be fitted with a colostomy bag on the outside of the opening, which can be a temporary or permanent solution, depending on the patient.
In the cases whereby a proctocolectomy has been performed, then the doctor will make a connection between the anus and small intestine, by using a small section of the small intestine to form the connection. This allows for normal evacuation of the waste.
Anesthesia
General anesthetic.
Procedure duration
The Colectomy takes 1 to 4 hours.
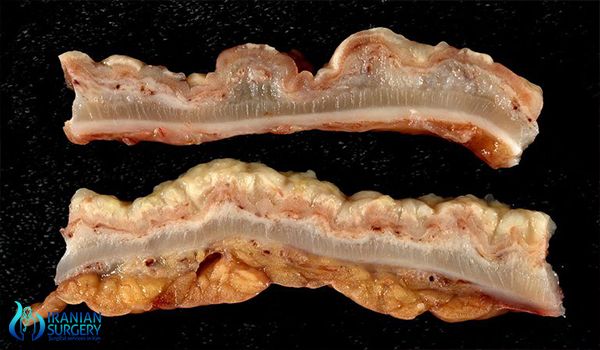
Recovery after your colectomy surgery
After colectomy surgery you'll be taken to a recovery room to be monitored as the anesthesia wears off. Then your health care team will take you to your hospital room to continue your recovery.
You'll stay in the hospital until you regain bowel function. This may take a couple of days to a week.
You may not be able to eat solid foods at first. You might receive liquid nutrition through a vein, often in your arm, and then transition to drinking clear liquids. As your intestines recover, you can eventually add solid foods.
If your surgery involved a colostomy or ileostomy to attach your intestine to the outside of your abdomen, you'll meet with an ostomy nurse who will show you how to care for your stoma. The nurse will explain how to change the ostomy bag that will collect waste.
Once you leave the hospital, expect a couple of weeks of recovery at home. You may feel weak at first, but eventually your strength will return. Ask your doctor when you can expect to get back to your normal routine.
10 common Questions about colectomy surgery
[kkstarratings]




2 Comments
Hello. I need a good surgent for colon cancer removal. Please let me know who you recommend. I am looking for someone with the highest level of experience.
Hello Ramin, Thank you for contacting Iranian surgery Regarding colon cancer, the details matters. you might need radiotherapy or chemotherapy and only after that you could undergo operation.
we have many professional surgeons performing colon cancer surgery both in Shiraz and Tehran, In MRI, Kowsar, Bazarganan, Mostafa khomeini ,etc hospitals.
To send your medical documents please contact us via Whatsapp number +98 922 176 2312 and get your personal consultation.