Luteinizing Hormone (LH)
Luteinizing Hormone (LH)
What is Luteinizing Hormone?
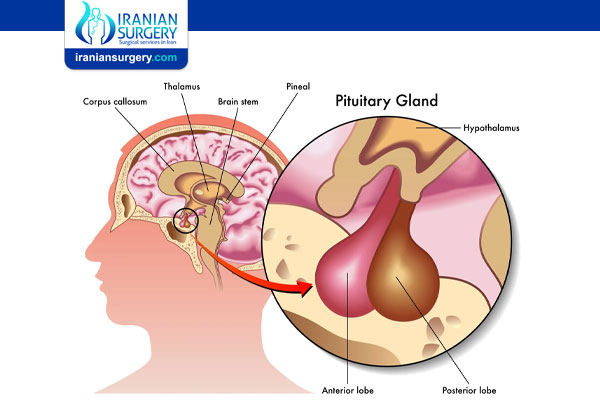
Luteinizing hormone (LH) stimulates processes in your body that are important for sexual health, development and reproduction. A tiny structure in your brain called the pituitary gland secretes LH. In turn, LH causes changes in your sex organs — your ovaries or testes — that allow your reproductive system to function correctly.
Function
What does luteinizing hormone do?
Your pituitary gland secretes two important hormones that work together to regulate processes in your reproductive system: follicle-stimulating hormone (FSH) and luteinizing hormone (LH). These hormones are chemical messengers that signal your sex organs (ovaries or testes) to start processes needed to support your reproductive health.
Think of LH as a chemical agitator that spurs your reproductive system to action.
Your sex organs produce either steroids or hormones (progesterone, testosterone) in response to LH.
. In the pituitary of people designated female at birth (DFAB), LH is released only in the second part of the menstrual cycle. That is, after an initial surge causes the release of an egg (ovulation), LH is released at a constant pace for two weeks. This stimulates ovarian progesterone production.
. In the pituitary of people designated male at birth (DMAB), LH is released at a constant pace over time and testosterone is produced at a constant level, as well.
Luteinizing hormone in women or DFAB
LH stimulates changes in your ovaries that maintain your menstrual cycle and support pregnancy. LH causes these changes in people designated female at birth (DFAB), including cisgender women and some transgender men and nonbinary people with vaginas.
. Ovulation: A surge in LH causes your ovary to release a mature egg around the second week of each menstrual cycle. A high LH level around this time means that you’re at that moment in your cycle when you’re most likely to get pregnant.
. Progesterone production: LH causes a structure in your ovary called the corpus luteum to produce more progesterone during the third and fourth week of your menstrual cycle. Progesterone is a hormone that’s needed to support the early stages of pregnancy.
As you age and go through menopause, your LH levels will increase as your levels of estrogen and progesterone decrease.
Luteinizing hormone in men or DMAB
LH stimulates your testes to make testosterone, a hormone your body needs to produce sperm. Testosterone is also responsible for secondary sex characteristics, like a deeper voice and more body hair and muscle mass. LH causes testosterone release in people designated male at birth (DMAB), including cisgender men and some transgender women and nonbinary people with penises.
LH hormone levels remain fairly stable after puberty among DMAB people.
Luteinizing hormone in infants and children
During puberty, LH stimulates both ovaries and testes to make more testosterone. In the ovary, testosterone is then converted into estrogen. These hormones cause changes related to sexual development.
Anatomy
Where is it located?
LH gets made in the part of your body that’s responsible for regulating complex processes, your brain. But the organs that LH helps regulate are in your reproductive system.
LH is part of a complex communication network that involves your brain (hypothalamus and pituitary gland) and your sex organs (ovaries and testes). Your hypothalamus secretes a hormone called gonadotropin-releasing hormone (GnRH) that signals your pituitary gland to secrete LH. LH signals your ovaries or testes to make the hormones needed to start and maintain reproductive processes.
Understanding this communication network is important when it comes to diagnosing reproductive health issues. For example, the root cause of fertility issues may involve your sex organs or hormone production in your brain. Your healthcare provider will consider multiple factors that play a role in your reproductive health when diagnosing conditions that involve LH.
Conditions and Disorders
What are the common conditions and disorders associated with luteinizing hormone?
LH levels fluctuate, especially with your menstrual cycle. A high or low LH level isn’t simply good or bad.
For instance, a surge in your LH can show that you’re about to ovulate. You’re most likely to become pregnant at this time. This information that LH provides about your fertility is helpful if you’re trying to have a baby.
LH levels in your body can signal problems, too. Knowing your LH level at a particular moment in time can help your provider learn:
. If you have a pituitary disorder.
. What’s causing fertility issues.
. What’s causing you to have irregular periods (DFAB people).
. How close you are to perimenopause or menopause (DFAB people).
. What’s causing you to have low testosterone levels (DMAB people).
LH levels tests can also help your provider diagnose early or delayed puberty in children.
What happens when luteinizing hormone levels are high?
High LH levels can signify that your sex organs aren’t producing enough steroid hormones needed for a reproductive process to take place. This is typical of when the ovaries and testes have exhausted their ability to produce estrogen and testosterone, from genetic, autoimmune, surgical, or physiologic causes.
Turner syndrome or Fragile X in DFAB people and Klinefelter syndrome in DMAB people are examples of genetic conditions associated with high LH levels.
Polycystic ovary syndrome (PCOS) is a condition that affects DFAB people that can cause mildly elevated LH levels. These are associated with irregular periods and infertility.
What happens when luteinizing hormone levels are low?
Low LH levels can signify that your pituitary gland isn’t making the LH needed to spur changes in your body that support sexual development or reproduction.
Low LH levels can be a sign of:
. Kallmann syndrome: A rare condition that leads to insufficient testosterone and estrogen production.
. Functional Hypothalamic Amenorrhea: When irregular or missed periods are related to excessive exercise habits.
Common tests to check luteinizing hormone levels?
An LH level test checks how much LH is in your blood and involves a simple blood draw. Sometimes, your healthcare provider will recommend doing an LH level test alongside an FSH test since these hormones work together to regulate your reproductive system.
What is a normal luteinizing hormone level?
When you get your test results, remember that what’s considered normal depends on various factors, including your age, gender and medical history. For DFAB people, the timing of your menstrual cycle or whether you’ve gone through menopause will affect your LH levels.
The numbers below provide a general snapshot of normal LH levels for cisgender men and women. Ask your healthcare provider what your test results mean for you.
. Women, weeks one and two of the menstrual cycle: 1.37 to 9 IU/L (international units per liter).
. Women, week two, before ovulation: 6.17 to 17.2 IU/L.
. Women, weeks three and four of the menstrual cycle: 1.09 to 9.2 IU/L.
. Women, postmenopausal: 19.3 to 100.6IU/L.
. Men: 1.42 to 15.4 IU/L.
Care
What foods increase luteinizing hormone?
A handful of studies have explored the relationship between vegetarian diets and low levels of LH and estrogen. Currently, no evidence shows that vegetarian diets reduce LH levels. Related, no evidence supports the thinking that food or diet can increase LH levels.
Speak with your healthcare provider about diet and lifestyle recommendations to improve your overall health, including habits that support brain functioning and reproductive health.
Source:
. https://my.clevelandclinic.org/health/body/22255-luteinizing-hormone