Keloid Scar
Keloid Scar
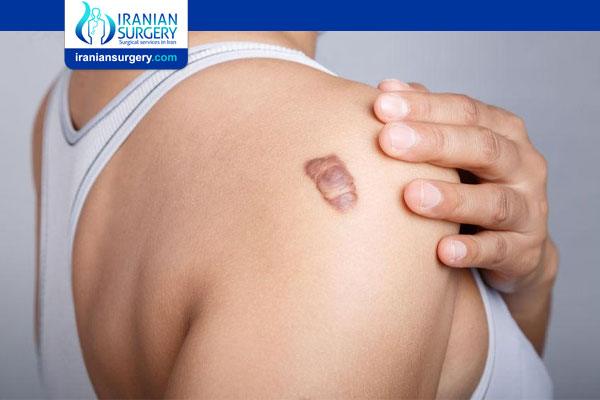
What is a Keloid Scar?
A keloid scar is a thick raised scar. It can occur wherever you have a skin injury but usually forms on earlobes, shoulders, cheeks or the chest. If you're prone to developing keloids, you might get them in more than one place.
A keloid scar isn't harmful to your physical health, but it can cause emotional distress. Prevention or early treatment is key.
Keloid scar treatment is possible. If you don't like how a keloid looks or feels, talk with a doctor about how to flatten or remove it. Even with treatment, a keloid can last for years or recur.
About Iranian Surgery
Iranian surgery website is an online medical tourism platform where you can find the best dermatologists in Iran. The price of Keloid Scar Treatment in Iran can vary according to each individual’s case and will be determined based on photos and an in-person assessment with the doctor.
For more information about the cost of Keloid Scar Treatment in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number 0098 901 929 0946. This service is completely free.
Before Keloid Scar Treatment
Symptoms
A keloid scar may form within months to years of the inciting injury. Signs and symptoms might include:
. Thick, irregular scarring, typically on the earlobes, shoulders, cheeks or middle chest
. Shiny, hairless, lumpy, raised skin
. Varied size, depending on the size of the original injury and when the keloid stops growing
. Varied texture, from soft to firm and rubbery
. Reddish, brown or purplish, depending on your skin color
. Itchiness
. Discomfort
When to see a doctor
Early treatment can help minimize growth of a keloid. Talk with a doctor soon after you notice a keloid. If you want to treat one that you've had for a while, talk with a doctor who specializes in skin conditions (dermatologist).
Causes
Experts don't completely understand what causes keloid scars. But most agree it's likely a dysfunction of the wound-healing process. Collagen — a protein found throughout the body — is useful to wound healing, but when the body produces too much, keloids can form.
Keloid growth might be triggered by any sort of skin injury — an insect bite, acne, an injection, body piercing, burns, hair removal, and even minor scratches and bumps. Sometimes keloids form for no obvious reason.
Keloids aren't contagious or cancerous.
A keloid is different from a hypertrophic scar. A hypertrophic scar stays within the bounds of the original wound and can fade over time without treatment.
Risk factors
Risk factors for keloids include:
. Having brown or Black skin. Keloids are most common in people with brown or Black skin. The reason for this predisposition is unknown.
. Having a personal or family history of keloids. Keloids can run in families, indicating that the tendency might be inherited. If you've had one keloid, you're at risk of developing others.
. Being under 30. You're more likely to develop a keloid if you're between the ages of 20 and 30.
Complications
Keloids located on a joint might develop hard, tight tissue that restricts movement.
Prevention
If you're prone to developing keloids, take these preventive self-care tips:
. Practice good wound care. Keep a wound clean and moist. Gently wash the area with mild soap and water. Apply a thin layer of petrolatum jelly (Vaseline, Aquaphor) or other ointment. Reapply the ointment throughout the day as needed. Your doctor might recommend applying a pressure pad or a silicone gel pad to a wound while it's healing. Adults need to take these preventive steps for six months after skin injury, and children up to 18 months.
Applying pressure earrings to your earlobes after an ear piercing helps prevent keloids.
. Protect your skin from injury. Try to avoid injuring your skin. Consider not getting body piercings, tattoos and elective surgeries. Even minor injuries — such as ingrown hairs, cuts and scratches — can incite a keloid to grow.
If you decide to undergo surgery, talk with your doctor about your tendency to develop keloids. Your doctor can use surgical techniques that reduce the risk of developing keloids at the surgical site. After surgery, ask your doctor about postoperative care and follow the instructions carefully.
Diagnosis
Your doctor usually can tell whether you have a keloid by looking at the affected skin. You might need a skin biopsy to rule out skin cancer.
During Keloid Scar Treatment
Treatment
Keloid scar treatments include the following. One or a combination of approaches might be best for your situation. Even after successful flattening or removal, keloids can grow back, sometimes bigger than before. Or you may develop new ones.
. Wound care. For newer keloids, the first treatment option might be compression dressings made from stretchy fabric or other materials. This method is also used after surgery to remove keloids. The goal is to reduce or prevent a scar by putting pressure on the wound as it heals. Such dressings need to be worn for 12 to 24 hours a day for 4 to 6 months to be effective. This method can be very uncomfortable.
. Corticosteroid cream. Applying a prescription strength corticosteroid cream can help ease itchiness.
. Injected medicine. If you have a smaller keloid, your doctor might try reducing its thickness by injecting it with cortisone or other steroids. You'll likely need monthly injections for up to six months before seeing the scar flatten. Possible side effects of corticosteroid injections are skin thinning, spider veins and a permanent change in skin color (hypopigmentation or hyperpigmentation).
. Freezing the scar. Small keloids might be reduced or removed by freezing them with liquid nitrogen (cryotherapy). Repeat treatments might be needed. Possible side effects of cryotherapy are blistering, pain and loss of skin color (hypopigmentation).
. Laser treatment. Larger keloids can be flattened by pulsed-dye laser sessions. This method has also been useful in easing itchiness and causing keloids to fade. Pulsed-dye laser therapy is delivered over several sessions with 4 to 8 weeks between sessions. Your doctor might recommend combining laser therapy with cortisone injections. Possible side effects, which are more common in people with darker skin, include hypopigmentation or hyperpigmentation, blistering and crusting.
. Radiation therapy. Low-level X-ray radiation alone or after surgical removal of a keloid can help shrink or minimize the scar tissue. Repeat treatments might be needed. Possible side effects of radiation therapy are skin complications and, in the long term, cancer.
. Surgical removal. If your keloid hasn't responded to other therapies, your doctor might recommend removing it with surgery in combination with other methods. Surgery alone has a recurrence rate of 45% to 100%.
Alternative medicine
There are no proven methods of removing keloid scars naturally. Some clinical studies have shown that onion extract used orally or on the skin might possibly be effective in improving the appearance of keloid scars and reducing itchiness and discomfort.
After Keloid Scar Treatment
Potential future treatments
Research into wound-healing issues, including keloid formation, shows promise. For example, studies include:
. Experimental topical creams and injectables to reduce and stop the growth of keloids
. Botulinum toxin type A (Botox) to improve wound healing
. Identifying genetic markers in keloid tissue
. Stem cell therapy
Lifestyle and home remedies
Try these keloid self-care tips:
. Care for your wound as directed. Wound care can be time-consuming, and compression dressings can be uncomfortable. Try to stick with the routine recommended by your doctor, as these steps are important to keloid prevention.
. Apply a corticosteroid cream. This type of nonprescription cream can help ease itchiness.
. Apply silicone gel. Applying nonprescription silicone gel can help ease itchiness.
. Protect the area from re-injury. Avoid irritating the keloid with clothing or other types of friction or injury.
. Protect your skin from the sun. Sun exposure might change the color of your keloid, making it more noticeable. That change might be permanent. Before going outside, protect your skin by covering the keloid or by liberally applying sunscreen.
Hypertrophic scars vs. keloid scars
What’s the difference between a hypertrophic scar and a keloid scar?
Before treating a keloid scar, it’s important to differentiate it from a similar type of scar called a hypertrophic. Keloid scars are smooth, hard, benign growths that also form when scar tissue grows excessively. Even your doctor may have difficulty telling the difference between a hypertrophic scar and a keloid, but it’s important to distinguish them because the treatment may be different.
In general, hypertrophic scars:
. Are raised, but rarely more than 4 millimeters above the skin
. Are red or pink in color
. Can develop anywhere on the body
On the other hand, keloids usually:
. Are raised more than 4 millimeters from the skin
. Grow beyond the boundaries of the original incision or wound
. Are pink to purple in color
. Evolve and grow over time
. Form on the earlobes, shoulders, cheeks, and chest above the sternum
Both scars tend to occur more commonly in darker skin types. Hypertrophic scars tend to be easier to treat than keloids, which have a high recurrence rate despite treatment.
Sources:
. https://www.mayoclinic.org/diseases-conditions/keloid-scar/symptoms-causes/syc-20520901
. https://www.healthline.com/health/hypertrophic-scar-treatment#hypertrophic-vs-keloid