How Does Egg Freezing Work?
How Does Egg Freezing Work?
People with ovaries are increasingly spending their 20s and 30s moving up the career ladder or achieving financial stability — and postponing having kids until later in life. But biology hasn’t quite caught up: Even as we put off children, fertility continues to decline as we age. Though egg freezing (or other artificial reproductive technology procedures) isn’t a guarantee of future fertility, preserving the quantity and quality of the eggs you're able to retrieve at a younger age can give you more options later in life.
That said, the process itself is pretty involved and can get in the way of your typical day-to-day. But if you understand the steps and possible side effects before making your decision, you can take time off or reschedule prior engagements — making it easier to accommodate daily injections, regular clinic appointments, and any reactions to medication. Everyone’s experience is 100% unique, but hearing from people who've gone through it can help you better prepare you for whatever comes.
So, we’re breaking down the steps of the process and including real-life examples of the egg freezing experience — all in an effort to give you the info you need to make the right decisions for you.
Here’s a summary before we dive in:
. Egg freezing is a method of fertility preservation that involves four phases: prep, stimulation and monitoring, egg retrieval, and the postoperative period.
. Research shows you may expect to retrieve about 14 mature eggs on average if you're 36 and under, about 10 if you're 37-39, about nine if you're 40-42, and about seven if you're 43+.
. According to the American Society for Reproductive Medicine, the chances of one single frozen egg resulting in a live birth later on are between 2% and 12%. Freezing more eggs increases those chances.
. If you're younger than 35, you have a 70% chance of a live birth if you freeze nine or more mature eggs. If you're in your early 40s, you may need to freeze significantly more eggs — 28 or more — for that same 70% chance of a live birth.
. One 2015 study found that the biggest difference in live birth rates between people who did and didn’t freeze their eggs was at age 37. At younger ages, the differences in live birth rates in people who did and did not freeze their eggs were smaller.
What Is Egg Freezing?
Egg freezing, or oocyte cryopreservation in medical-speak, is a fertility preservation technique where eggs are extracted from the ovaries and flash-frozen so they can be used for an assisted reproductive technology (ART) procedure, like in-vitro fertilization (IVF), later on.
What Happens When You Freeze Your Eggs?
Here, we'll explain each of the steps involved in freezing your eggs and recommend questions you can ask at the clinic to make sure you're fully prepared.
Prepping for the procedure
Before the egg freezing can begin, you’ll meet with a reproductive endocrinologist (REI) at a fertility clinic for a comprehensive evaluation. Here’s what you can typically expect to happen:
. They'll take your medical history, do bloodwork and fertility hormone testing, perform a physical exam, and conduct a vaginal ultrasound to assess your antral follicle count, or AFC (the number of eggs in your ovaries at that point in time, aka your ovarian reserve).
. You’ll talk with the doctor about the egg freezing process (which you’ll already have a leg up on after this post!) and schedule an appointment a few weeks later, after your test results come back.
. The clinic will then develop your unique plan of action, or “stimulation protocol.” Your exact stimulation protocol will be designed for you to maximize the numbers of mature eggs retrieved and to minimize the risk of ovarian hyperstimulation syndrome (OHSS), which very rarely happens during the fertility treatment process when there are a significant number of follicles present.
. You’ll also talk with your doctor about how many eggs you can expect to retrieve after stimulation (and we’ll cover this a bit below). You might discover that you need more than one round of retrieval before you get enough eggs for in-vitro fertilization (IVF) — the procedure that will allow you to fertilize and implant the frozen eggs after thawing.
. You’ll meet with a nurse to discuss your medications, how to mix them and give them to yourself, and go over an outline of your calendar and an estimated timeline for the egg retrieval process.
If you are on birth control pills, your fertility doctor may have you stop those 4-8 weeks prior to proceeding with your egg freezing cycle as studies have shown prolonged OCP use may reduce the number of eggs retrieved in some patients.
Possible questions to ask at the fertility clinic:
Does the clinic have experience in freezing eggs and, importantly, thawing eggs?
Can they share their thaw rates for frozen eggs as well as pregnancy or live birth rates from people coming back to use their frozen eggs?
How many eggs may be expected from one retrieval?
Is there a chance you may need more than one cycle of egg freezing to freeze a sufficient number of eggs?
What is the cost of the procedure at the clinic?
Does the clinic offer a discount if you may need to do more than one cycle?
If you have questions during this process (which you likely will), is there a direct contact for you to ask questions to?
Do they batch cycles? (This means a clinic has designated days during the month to start patients' stimulation cycles so this may mean less flexibility for you in terms of timing.)
Stimulation and monitoring
When it’s time for stimulation of the ovarian follicles (the structures that house and mature your eggs), there’s a typical order of operations:
. Starting injections: There are different protocols of when you will start your injections based on where you are in your cycle, timing, and ovarian reserve:
. You may start a short course of birth control pills, estrogen, lupron, or aygestin (a form of progesterone) prior to starting injections. The purpose of these medications is to help synchronize your follicles so they're all starting at the same time and will (hopefully) be equally responsive to medication — and to help with timing so you can do this process when it's convenient for you.
. Most clinics will start giving you these medications during your period or after ovulation. You’ll also get another ultrasound and possibly more blood work prior to starting your fertility injections.
. Monitoring: Once you're done with these medications, you’ll return to the clinic for another evaluation via ultrasound and possible blood tests. At that time, you’ll start the injections if everything's going as expected.
. The nursing team will guide you through the injections, but they'll usually be a combo of menotropins (equal amounts of follicle-stimulating hormone, or FSH, and luteinizing hormone, or LH) and gonadotropins (pure FSH) to stimulate your ovaries to grow multiple eggs at one time.
. You’ll likely give yourself the injections in your belly at the same time each day, in the evening, for 10-12 consecutive evenings. Depending on how you respond to the meds, your physician may adjust your dose to be higher or lower.
. Measuring your anti-Mullerian hormone (AMH) in advance can give you an idea of how well you’ll respond to ovarian stimulation and how many cycles of retrieval you might expect — this is because AMH is a great marker of ovarian reserve.
. More injections: You’ll be given an additional injection that you'll take daily (either Ganirelix or Cetrotride) usually starting around day 5-7 of injections to prevent ovulation during this process.
. When you start this additional shot, this is normally the time when your ovaries are starting to enlarge and where your clinic will likely recommend reducing vigorous activity (like running, HIIT exercises, or other high-impact workouts) to minimize the risk of ovarian torsion.
. You may notice a little redness or itching around the injection site. This is totally normal.
. Continued monitoring: You’ll continue to be monitored at the clinic through ultrasounds and blood tests, typically done in the morning to get same-day results back on your labs and determine your dosing of injections.
. The number of visits will be determined by your doctor, but they are usually more spread out during the first half of your cycle — then close to every day or every other day by the second half of your cycle. You can usually anticipate anywhere from 4-7 of these “monitoring” visits.
. Trigger shot prior to retrieval: When you're ready for retrieval, based on the size of the follicles (as measured by ultrasound) and estrogen blood levels, you’ll give yourself a final shot known as the "trigger shot" of the hormone human chorionic gonadotropin (hCG) and/or lupron about 36 hours before the procedure for final egg maturation.
Possible questions to ask at the fertility clinic:
What time does morning monitoring begin?
Who will be doing the scans? (Clinics may have different people doing the monitoring ultrasound including your doctor, the doc of the day, nurse practitioners, and/or ultrasound technicians.)
Based on the protocol picked for you, how many days can you expect to do the injections?
Egg retrieval and recovery
This step in the process is also sometimes referred to as "egg harvesting." Here's what may happen:
. You'll get an iv started: When you arrive, you'll have an IV started that will be used to administer sedation medications to help you fall asleep — as well as provide initial pain relief after the procedure.
. Anesthesia begins: You'll then be taken back to the procedure room, have an oxygen cannula placed under your nose, and be given propofol anesthesia medications through your IV to go to sleep. Throughout the entire egg freezing procedure, you'll be breathing on your own (i.e., no intubation).
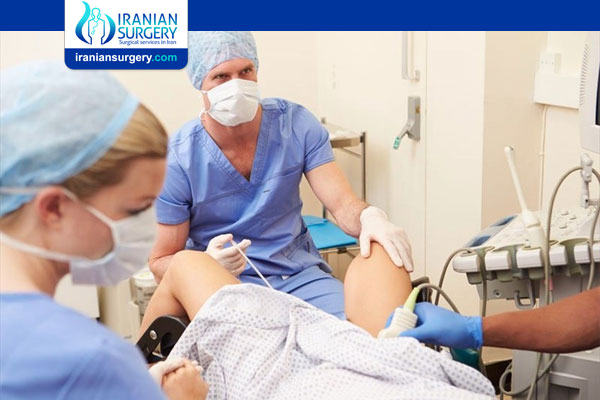
. Egg retrieval begins: Your doctor will use a vaginal probe with a needle attached to it and, using ultrasound guidance, will access your follicles. The needle will be inserted into your follicles and the fluid will be aspirated into tubes which are then given to the embryologist who will sort through the fluid to find the eggs. There will be constant communication between the specialists throughout the process, and once they’ve collected the eggs they can, you’ll be sent to the recovery room. The procedure will typically last for 10-20 minutes.
. You'll find out how many eggs you retrieved: Once you’re awake, you’ll find out how many eggs were retrieved — but you likely won't know how many mature eggs were frozen until 24 hours later. (Per one 2017 study, around 14 eggs retrieved will be mature enough to use for people under 36, and around eight for 40-year-olds.) You'll recover for about 30-60 minutes in the recovery area and will then be on your way home!
. Rest And Recover: After the egg retrieval, you'll go home to rest. Typical symptoms within the first 24 hours may include light vaginal spotting, abdominal cramping, bloating, and constipation. Usually, your clinic will recommend Tylenol and heating pads to help with the cramping. If you have severe abdominal pain, heavy vaginal bleeding, or feel faint or lightheaded, contact your clinic.
Possible questions to ask at the fertility clinic:
Who usually does the egg retrieval? Will it be your doctor or is there a rotation of doctors who do the procedures for that day?
When can you resume normal activity?
What side effects should you expect based on your ovarian reserve and anticipated number of eggs retrieved?
When can you go back to work?
And finally… egg freezing time
A few hours after retrieval, only your fully matured eggs will be frozen through a process called vitrification — a technique of rapid freezing in liquid nitrogen (which is 196 degrees below zero celsius) to reduce the formation of ice crystals on the eggs and improve their survival rates.
What Are the Success Rates for Egg Freezing?
Because ovarian reserve changes with age, the expected number of eggs retrieved changes with age too. It’s important, though, to note that just like with many other aspects of health, there’s variation between people when it comes to the number of eggs you have as you age. While some people may experience steep declines in egg quantity, that decline may be much more gradual for others.
One 2017 study looked at 520 people (with presumed "average" ovarian reserve for their age) who had undergone egg retrieval and found that:
. For ages 36 and under: About 14 mature eggs on average were retrieved.
. For ages 37-39: About 10 mature eggs on average were retrieved.
. For ages 40-42: About nine mature eggs on average were retrieved.
. For ages 43 and above: About seven mature eggs on average were retrieved.
Is There A "Best" Number When It Comes to Egg Retrieval?
No, but there are some guidelines about how many frozen eggs are needed for a good chance of a live birth later on:
. According to the American Society for Reproductive Medicine, if someone freezes one single egg, the chances of that single egg resulting in a live birth later on are between 2% and 12%.
. Freezing more eggs, either through one retrieval or through additional rounds, increases those chances.
. Someone younger than 35 has a 70% chance of a live birth if they freeze nine or more mature eggs.
. People in their early 40s may need to freeze significantly more eggs — 28 or more — for that same 70% chance of a live birth.
What About A "Best" Age for Freezing Your Eggs?
One 2015 study created decision-analysis models of egg freezing at different ages to figure out this very answer, with special attention to when egg freezing was the most beneficial for increasing the probability of live births.
When comparing people who froze their eggs to those who didn't, here's what the study's authors found:
. The greatest improvement in the probability of live birth was seen in 37-year-olds who tried to conceive seven years later (51.6% chance of a live birth in a 44-year-old who froze their eggs when they were 37, 21.9% in 44-year-olds who never froze their eggs and tried to conceive without treatment at 44).
. The highest overall live birth rates were in people who froze their eggs before they were 34.
The authors also made a handy tool so that you can actually see what these numbers could look like for you.
Ultimately, the younger you are when you freeze your eggs, the better your future outcomes as egg quantity and quality will be better. However, doctors must balance the age at which you freeze your eggs with the likelihood that you may actually need to use them — which is where studies are helpful.
What's It Really Like to Freeze Your Eggs?
Since the egg freezing experience varies so much from person to person, we here we have provided you with three firsthand accounts by patients who went through the process.
Sarah, 33, and her partner both underwent two rounds of egg retrieval. Sarah experienced no side effects during stimulation, "apart from severe bloat a few days prior to retrieval." As for the retrieval itself, Sarah says it was "pretty seamless": "We each had pain the first few hours that was helped by ibuprofen and rest. We got really good about pushing Gatorade to help with the bloat and cramping."
Ultimately, Sarah explains the biggest experience was feeling overwhelmed and confused along the way — which was compounded by the fact that she and her partner both went through it. "We also had to advocate for ourselves with our fertility clinic, which can be overwhelming when you don’t actually know what medication protocols should be, how the retrieval process works, etc." Sarah and her partner found the second round of egg retrieval easier to prepare for because they knew what to expect. "After both retrievals, I was able to freeze 42 viable oocytes — my partner has 40," she says.
Christine, who's 36 and has diminished ovarian reserve (DOR), calls the two retrieval rounds she went through to freeze her eggs "a stressful yet exciting time," but playing her favorite music and watching prep videos helped with taking her stimulation dose. "The first few nights I had some nausea, but that went away as my body got used to the meds," Christine explains. "I also had dry mouth from Menopur/Follistim. During my second stims, Omnitrope was added to my protocol which gave me minor morning headaches." She also felt lazier and fatigued. Christine says the clinic gave her pain medication before the retrieval, but she didn't feel any pain after it was over.
"I awoke around 9:30am for both retrievals and was discharged by 10:30am," Christine says. There was more bloating after the first retrieval and less after the second. Still, she was able to go back to working remotely the same day of each retrieval, though "with lower-than-normal productivity." In the end, Christine froze two eggs after her second retrieval — which was an expected outcome given the DOR diagnosis. While she found the results of her first retrieval "hard to swallow," "I was pleasantly surprised by the outcome of the second retrieval!" she explains.
33-year-old Ashley ended up "putting off" egg freezing for a year after her consultation before undergoing stimulation meds. For Ashley, the most complicated part of the process has been ordering her meds: "There are multiple possible pharmacies and I had to contact them all to compare prices," she says. Ashley felt anxious about egg freezing outcomes, but "learning from others in online communities, as well as listening to podcasts about fertility and egg freezing" have helped her feel more prepared.
If you’re considering egg freezing in the near (or far) future, testing your AMH levels with the Iranian Surgery Hormone Test can help you predict your outcomes. That way, when you head into that first clinic appointment, you’ll be ahead of the game — and already armed with plenty of info to help you make your decision.
About Iranian Surgery
Iranian surgery is an online medical tourism platform where you can find the best doctors and fertility specialists in Iran. The price of IVF in Iran can vary according to each individual’s case and will be determined by an in-person assessment with the doctor.
For more information about the cost of IVF in Iran and to schedule an appointment in advance, you can contact Iranian Surgery consultants via WhatsApp number 0098 901 929 0946. This service is completely free.
Source:
https://modernfertility.com/blog/egg-freezing-process/