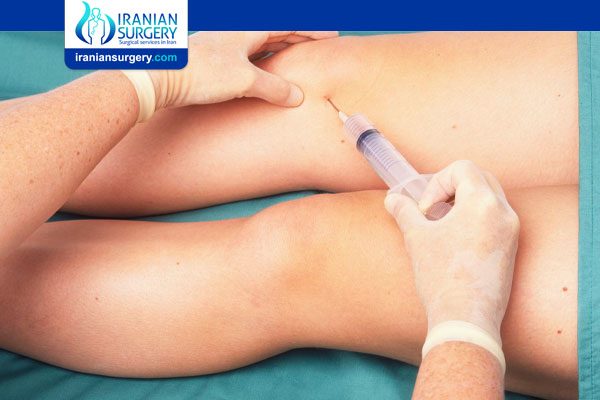
Arthrocentesis (Joint Aspiration)
What is Arthrocentesis (Joint Aspiration)?
Joint aspiration is a procedure to remove excess fluid through a needle from a joint (commonly a knee, ankle, elbow or hip). Joint injection involves injecting medications, such as corticosteroids, into the joint to relieve pain.
Arthrocentesis (joint aspiration) can help your healthcare provider find the cause of swollen, painful joints. It can also provide symptom relief.
Healthcare providers use a thin needle to remove (aspirate) fluid from the affected joint. After aspiration, your provider may inject medications into the joint. These medicines temporarily ease pain and inflammation.
Before Arthrocentesis (Joint Aspiration)
What causes joint pain?
Joints are part of your skeletal system. They are the connection where two bones meet.
Cartilage tissue at the ends of bones helps them move and glide. Synovial fluid cushions and lubricates joints and cartilage. Joint pain, inflammation and swelling occur when something reduces the synovial fluid, cartilage or both.
Conditions that cause joint pain include:
. Arthritis, including osteoarthritis, gout and psoriatic arthritis.
. Autoimmune diseases, including rheumatoid arthritis and lupus.
. Bacterial infections, including Lyme disease.
. Bursitis and tendonitis.
Read more about : Knee replacement
What is the purpose of joint aspiration (arthrocentesis), and when is it performed?
Joint aspiration can be both used for diagnosis and medical treatment of arthritis of a joint. Joint aspiration is used to obtain fluid from the patient's joint for examination in the laboratory.
Analysis of joint fluid can help the physician to define causes of joint swelling (joint effusion) or arthritis, such as infection, gout arthritis, and rheumatoid disease. Fluid from the joint can be tested for white cell count, crystals, protein, glucose, as well as cultured to detect infection. Each of these laboratory parameters can be helpful in defining the cause of a particular form of arthritis, particularly in distinguishing inflammatory from non-inflammatory forms of arthritis. The result can be key to identifying various potential rheumatology diseases and musculoskeletal conditions.
Joint aspiration can also be a helpful treatment in relieving joint swelling and pain. Removal of synovial fluid from the joint that is inflamed can also remove the white blood cells within that are sources of enzymes that can be destructive to the joint.
This treatment can more rapidly restore the health of the joint. Bursa aspiration procedure and indications for bursitis are analogous to joint aspiration for arthritis, except the bursa is the target instead of the joint (intra-articular). The result and analysis of the fluid (aspirate) is similarly evaluated for various diseases and conditions in the laboratory.
What are joint injections?
After joint aspiration, your healthcare provider may inject corticosteroids into the joint. This anti-inflammatory medication eases pain, swelling and stiffness. The drugs may also slow the return of excess fluid to the joint.
Steroid injections work best for inflammatory conditions like arthritis and tendonitis. Treatment effects last a couple of months. You shouldn’t get more than four injections in the same joint within a year. Steroid overuse can damage the joint and weaken supporting tendons and ligaments.
What is viscosupplementation?
Viscosupplementation is a type of joint injection that specifically treats osteoarthritis. Research on the effectiveness of this treatment shows mixed results. Some people have less pain and improved movement after treatment. But some people see no change.
Your healthcare provider injects hyaluronic acid into a joint (usually the knees). This substance occurs naturally in synovial fluid surrounding joints.
You get one to five injections over a few weeks. It can take several weeks for symptoms to improve. Viscosupplementation may relieve pain and improve mobility for about six months. You can get the treatment again.
Who should not undergo joint aspiration (arthrocentesis)?
There are few health contraindications to a joint aspiration. People who are taking blood-thinning medicines (anticoagulants such as warfarin [Coumadin]) for underlying health reasons can have bleeding into the joint.
The risk of this is extremely low, unless the level of blood thinner is too high (making the blood very thin), in which case the procedure may need to be temporarily delayed. The risk of bleeding into the joint is minimized when the physician uses the thinnest needle possible and applies cold packs after the procedure. If the skin over a joint is infected, the joint should not be aspirated, in order to prevent the infection from spreading into the joint.
Preparing for Joint Aspiration (Arthrocentesis)
A needle and syringe are used to aspirate excess fluid from a joint. A local anesthetic may be used to limit pain and discomfort. Before the procedure takes place, a patient should tell the doctor if they:
. Take any medications, including over-the-counter medicines and herbal supplements
. Are allergic to any medications, latex, or anesthesia
. Have any kind of infection or a blood or bleeding disorder
. Are or could be pregnant
Some patients who take blood thinners or anticoagulants may be asked to stop taking these medications in the days leading up to arthrocentesis. Other patients may continue to take these medications but will need to give the aspirated joint a little extra care, such as applying direct pressure to the needle site and resting the joint for a little longer than normal.
Patients who will undergo general anesthesia and those whose joint fluid will be tested for glucose levels may need to fast before arthrocentesis. (Most individuals do not need to fast.)
Patients may also want to ask their doctors if their ability to drive or do other essential tasks will be affected in the hours following the procedure.
Risks and Complications
What are potential risks or complications of arthrocentesis (joint aspiration) and joint injections?
Joint aspirations and injections are relatively safe. Rarely, these complications develop:
. Allergic reaction: Some people are allergic to the anesthetic or the injectable medication. In very rare instances, this can cause anaphylaxis, a life-threatening response.
. Infection: Rarely, people develop infections after getting steroid injections.
. Post-injection flare: An estimated 1 in 50 people develop post-injection flare several hours after getting an injection. It causes joint swelling and pain that subsides in a few days.
Who performs a joint aspiration (arthrocentesis)?
Joint aspirations can be performed under medical guidelines by qualified doctors, including general physicians, internists, orthopedic surgeons, rheumatologists, interventional radiologists, emergency room physicians, as well as nurse practitioners and physician assistants.
During Arthrocentesis (Joint Aspiration)
How does arthrocentesis (joint aspiration) work?
Fluid buildup in joints (effusion) puts pressure on the joint. Excess fluid causes pain and swelling. You may find it difficult to bend and move the joint.
Your healthcare provider may drain the fluid and send a sample to a lab. Tests can determine the cause of the fluid buildup.
As a treatment, joint aspiration eases swelling and joint pressure. You should have less pain and find it easier to move after this procedure. Excess fluid often comes back. You may need joint aspiration again.
Healthcare providers typically use arthrocentesis on the:
. Hips, knees, ankles and feet.
. Elbows, shoulders, wrists and hands.
How are arthrocentesis (joint aspiration) and joint injections performed?
Joint aspirations and injections take place in your healthcare provider’s office. Your provider may use images from an ultrasound or X-rays (fluoroscopy) to guide procedures.
First, your provider disinfects the skin. For smaller joints, your provider applies a numbing cream to the skin. You may need a local anesthetic to numb a bigger joint section like the hips or shoulders.
During joint aspiration and injection, your provider:
- Inserts a thin needle into the joint.
- Attaches an empty syringe to the needle and draws fluid out of the joint (aspiration). Your provider may need multiple syringes to remove all of the fluid.
- Removes the syringe with the excess fluid and replaces it with a syringe that contains medication.
- Uses the same needle and entry point to inject medication into the joint.
- Places a bandage over the treatment area.
After Arthrocentesis (Joint Aspiration)
Arthrocentesis Recovery
While some patients may resume activities immediately after arthrocentesis, others may be told to rest the affected joint from anywhere between 4 to 24 hours. These patients may be required to have another person drive them home following the procedure.
Local anesthetics, such as lidocaine, typically wear off in 2 to 4 hours, so patients may feel an increase in pain shortly after leaving the doctor’s office. It is common to have mild soreness for a day or two after the procedure.
Patients should ask their doctors whether it is okay to take nonsteroidal anti-inflammatory drugs (NSAIDs) or other over-the-counter pain medications. Depending on the circumstances, the doctor may recommend periodically icing the affected joint and wrapping it in a bandage to prevent re-swelling.
How effective are arthrocentesis (joint aspiration) and joint injections?
Joint aspiration and injections can temporarily relieve joint inflammation and pain. The treatments can also improve mobility.
When should I call the doctor?
Call your healthcare provider if you experience:
. Allergic reaction, such as worsening pain or difficulty breathing.
. Fever, chills.
. Signs of infection, such as redness, heat or swelling at the treatment site.
. Worsening pain at the treatment site.
Sources:
. https://my.clevelandclinic.org/health/treatments/14512-arthrocentesis-joint-aspiration
. https://www.arthritis-health.com/treatment/joint-aspiration/what-arthrocentesis-joint-aspiration