Amenorrhea
Amenorrhea
What is Amenorrhea?
Amenorrhea is when you don’t get your monthly period. It can be temporary or permanent. Amenorrhea can result from a change in function or a problem with some part of the female reproductive system.
There are times when you’re not supposed to get your period, such as before puberty, during pregnancy and after menopause. If amenorrhea lasts for more than three months, it should be investigated.
Before Amenorrhea Treatment
How does the menstrual cycle work?
A complex system of hormones controls the menstrual cycle. Every month, hormones prepare the body for pregnancy. Ovulation then occurs. If there is no pregnancy, the cycle ends with the uterus shedding its lining. That shedding is the menstrual period.
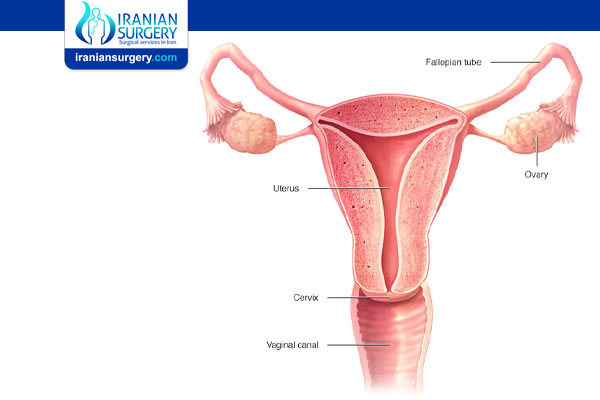
The hormones responsible for this cycle originate in different parts of the body. A dysfunction in any of these parts can prevent a person from getting a period:
. Hypothalamus, which controls the pituitary gland.
. Pituitary gland, called “the master gland,” which produces the hormones that instruct the ovaries to ovulate.
. Ovaries, which produce the egg for ovulation and the hormones estrogen and progesterone.
. Uterus, which responds to the hormones and prepares the lining. This lining sheds as the menstrual period if there’s no pregnancy.
What are the types of amenorrhea?
There are two classifications of amenorrhea:
. Primary amenorrhea is when you haven’t gotten a first period by age 15 or within five years of the first signs of puberty. It can happen due to changes in organs, glands and hormones related to menstruation.
. Secondary amenorrhea is when you’ve been getting regular periods, but you stop getting your period for at least three months, or you stop your menses for six months when they were previously irregular. Causes can include pregnancy, stress and illness.
Who is at risk for amenorrhea?
Risk factors for amenorrhea include:
. Family history of amenorrhea or early menopause.
. Genetic or chromosomal condition that affects your menstrual cycle.
. Obesity or being underweight.
. Eating disorder.
. Over-exercising.
. Poor diet.
. Stress.
. Chronic illness.
What causes amenorrhea?
The different types of amenorrhea have different causes.
Common causes of primary amenorrhea include:
. Chromosomal or genetic problem with the ovaries (the female sex organs that hold the eggs).
. Hormonal issues stemming from problems with the hypothalamus or the pituitary gland.
. Structural problem with the reproductive organs, such as missing parts of the reproductive system.
Common causes of secondary amenorrhea include:
. Pregnancy (which is the most common cause of secondary amenorrhea).
. Breastfeeding.
. Menopause.
. Some birth control methods, such as Depo Provera, intrauterine devices (IUDs) and certain birth control pills.
. Chemotherapy and radiation therapy for cancer.
. Previous uterine surgery with subsequent scarring (for example, if you had a dilation and curettage, often called D&C).
Other causes of secondary amenorrhea can include:
. Stress.
. Poor nutrition.
. Weight changes — extreme weight loss or obesity.
. Exercising associated with low weight.
. Ongoing illness or chronic illness.
You may also have conditions that can cause secondary amenorrhea:
. Primary ovarian insufficiency, when you experience menopause before age 40.
. Hypothalamus disorders, such as functional hypothalamic amenorrhea (FHA) — which is also called hypothalamic amenorrhea (HA). FHA is a condition where amenorrhea is associated with stress or weight loss, but isn’t clearly caused by an organic issue with a woman’s body.
. Pituitary disorders, such as a benign pituitary tumor or excessive production of prolactin.
. Other hormonal problems, such as polycystic ovary syndrome, adrenal disorders or hypothyroidism.
. Ovarian tumors.
. Surgery to remove uterus or ovaries.
What are the symptoms of amenorrhea?
The main symptom is the lack of periods. Other symptoms depend on the cause. You may experience:
. Hot flashes.
. Nipples leaking milk.
. Vaginal dryness.
. Headaches.
. Vision changes.
. Acne.
. Excess hair growth on your face and body.
Diagnosis and Tests
How is amenorrhea diagnosed?
If you miss a period, contact your healthcare provider. Your provider will ask you about your symptoms and medical history. If amenorrhea occurred because of pregnancy, you can start prenatal care. If it’s happening because of menopause, there is help if symptoms are uncomfortable. Missed periods leading to menopause usually begin in your 40s. Your provider will perform a physical exam and a pelvic exam.
Will I need any tests to diagnose amenorrhea?
Your healthcare provider may want to do some tests, including:
. Pregnancy test.
. Blood tests to check hormone levels and detect thyroid or adrenal gland disorders.
. Genetic testing, if you have primary ovarian insufficiency and are younger than 40.
. MRI, if your provider suspects a problem with the pituitary gland or hypothalamus.
Do I need to keep track of when my periods happened?
Diagnosing amenorrhea can be challenging. If the cause of amenorrhea isn’t obvious, such as pregnancy, your provider may ask you to keep a record of changes in your menstrual cycle. This history of your periods can help your provider figure out a diagnosis.
Using an app or a journal, note:
. How long your periods last.
. When you had your last period.
. Medications you are taking.
. Changes in your diet or exercise routine.
. Emotional challenges you’re having, such as stress.
Prevention
How can I prevent amenorrhea?
Living a healthy lifestyle can help prevent some causes of secondary amenorrhea. Try to:
. Maintain a healthy weight and eat a healthy diet.
. Be aware of your menstrual cycle (so you’ll know if you miss a period).
. Get regular gynecological appointments, including having a pelvic exam and Pap test.
. Get regular and adequate sleep.
Are there complications of amenorrhea?
Amenorrhea is not life-threatening. However, some causes may lead to increased risks over the long term, so amenorrhea should always be evaluated. Researchers have found a greater risk of hip and wrist fractures in people with amenorrhea. You may also be at high risk for bone thinning and fertility difficulties.
During Amenorrhea Treatment
Management and Treatment
How is amenorrhea treated?
If your period stopped because of menopause or pregnancy, your provider will not need to treat it. In other cases, your treatment will depend on the cause and may include:
. Losing weight through dieting and exercise (if excess weight is the cause).
. Gaining weight through an individualized diet plan (if extreme weight loss is the cause).
. Stress management techniques.
. Changing exercise levels.
. Hormonal treatment (medication), as prescribed by your healthcare provider.
. Surgery (in rare cases).
In addition, your healthcare provider may recommend some treatments to help with the side effects of amenorrhea:
. Estrogen therapy to relieve hot flashes and vaginal dryness.
. Calcium and vitamin D supplements to keep bones strong.
. Strength training.
Amenorrhea may be a symptom of anorexia nervosa, an eating disorder. If you or a loved one has this condition, talk to a healthcare provider immediately so you can get the right treatment.
Will I need surgery for amenorrhea?
Surgery for amenorrhea is rare. Your healthcare provider may recommend it if you have:
. Genetic or chromosomal problems.
. Pituitary tumor.
. Uterine scar tissue.
After Amenorrhea Treatment
Outlook / Prognosis
Will my period return?
Typically, your period will return once you treat the underlying cause. However, it may take time to become regular again.
In some cases, you may have a health problem that means you’ll never have a period. If that is the case, your provider can talk to you about fertility options if you wish to have a baby.
What are the outcomes for people with amenorrhea?
Your particular outcome will depend on the cause. For example, if you have PCOS, you will likely need lifelong care to prevent health complications and to establish regular cycles.
How can I take care of myself if I have amenorrhea?
Amenorrhea can affect bone health. It’s important to eat a calcium-fortified diet and exercise regularly.
When should I see my healthcare provider about amenorrhea?
You should call your healthcare provider if you miss three months of periods or miss a period and:
. Have trouble with balance, coordination or vision, which could indicate a more serious condition.
. Produce breast milk when you have not given birth.
. Notice excessive body hair growth.
. Are older than 15 and haven’t gotten your first period yet.
Source:
. https://my.clevelandclinic.org/health/diseases/3924-amenorrhea