Adenomyosis
Adenomyosis
What is Adenomyosis?
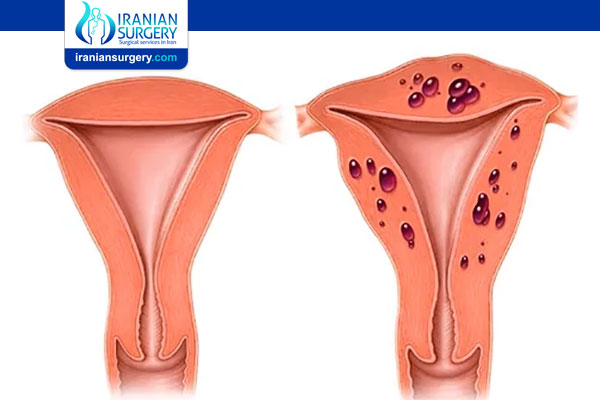
Adenomyosis is a condition of the female reproductive system. It causes the uterus to thicken and enlarge.
Endometrial tissue lines the inside of the uterine wall (endometrium). Adenomyosis occurs when this tissue grows into the myometrium, the outer muscular walls of the uterus. This extra tissue can cause the uterus to double or triple in size and lead to abnormal uterine bleeding and painful periods.
Before Adenomyosis Treatment
What is the difference between adenomyosis and endometriosis?
Adenomyosis and endometriosis are disorders that involve endometrial tissue. Both conditions can be painful. Adenomyosis is more likely to cause heavy menstrual bleeding. The difference between these conditions is where the endometrial tissue grows.
. Adenomyosis: Endometrial tissue grows into the muscle of the uterus.
. Endometriosis: Endometrial tissue grows outside the uterus and may involve the ovaries, fallopian tubes, pelvic side walls, or bowel.
How common is adenomyosis?
Many women aren’t aware they have adenomyosis because the condition doesn’t always cause symptoms. The condition may affect 20% to 65% of females.
Who might get adenomyosis?
Adenomyosis has been found in adolescents, but typically occurs in females between the ages of 35 and 50 who have:
. At least one pregnancy.
. Endometriosis.
. Uterine fibroids.
What causes adenomyosis?
Experts don’t know why some people develop adenomyosis. The condition is more common in women who have had children.
What are the symptoms of adenomyosis?
Many people with adenomyosis don’t have symptoms. Some people experience:
. Painful menstrual cramps (dysmenorrhea).
. Heavy menstrual bleeding (menorrhagia).
. Abnormal menstruation.
. Pelvic pain.
. Painful intercourse (dyspareunia).
. Infertility.
. Enlarged uterus.
Diagnosis and Tests
How is adenomyosis diagnosed?
Healthcare providers often diagnose adenomyosis based on symptoms and one or more of these tests:
. Pelvic exam: During a pelvic exam, your provider may notice that your uterus has gotten larger, softer, or more painful when palpated.
. Ultrasound: A transvaginal ultrasound uses sound waves to produce images of pelvic organs. These images can sometimes show thickening of the muscle raising suspicion for adenomyosis.
. Imaging scans: Magnetic resonance imaging (MRI) scans can show uterine enlargement and thickening of certain areas of the uterus which can be indicative of adenomyosis.
. Biopsy: Because tissue grows within the uterus walls, the only way to biopsy tissue is after a hysterectomy, which removes the uterus.
How does adenomyosis affect pregnancy?
Adenomyosis tends to affect women who have had at least one child. However, the condition may make it difficult to conceive for the first time or to have another child. Infertility treatments may help. Once pregnant, there is an increased risk of:
. Miscarriage (loss of pregnancy before a baby fully develops).
. Premature labor (childbirth before the 37th week of pregnancy).
Prevention
How can I prevent adenomyosis?
Because no one knows what causes adenomyosis, healthcare providers don’t know of anything you can do to prevent it.
What are the complications of adenomyosis?
Heavy menstrual bleeding from adenomyosis increases your risk of anemia. Anemia occurs when your body doesn’t have enough iron-rich red blood cells. You may feel chronically fatigued or cold.
During Adenomyosis Treatment
Management and Treatment
How is adenomyosis managed or treated?
Because the female hormone estrogen promotes endometrial tissue growth, adenomyosis symptoms often go away after menopause. In the meantime, these treatments can ease pain, heavy bleeding and other symptoms:
. Pain medications: Nonsteroidal anti-inflammatory drugs, or NSAIDs, such as ibuprofen (Advil®, Motrin®) or naproxen (Aleve®), ease cramping.
. Hormonal birth control: Estrogen thickens the uterine wall and can worsen bleeding and cramping. Certain hormonal contraceptives can stop menstruation and symptoms. Options include birth control pills, Depo-Provera® injection and hormonal intrauterine devices (IUD), such as Mirena®.
. Hysterectomy: This surgery removes the uterus. After a hysterectomy, you won’t have a menstrual cycle or be able to get pregnant.
After Adenomyosis Treatment
Outlook / Prognosis
What is the prognosis (outlook) for people with adenomyosis?
Many women who experience life-disrupting symptoms from adenomyosis find relief through hormonal treatments and pain relievers. A hysterectomy is a permanent solution that provides long-term symptom relief. After menopause, symptoms should go away.
When should I call the doctor?
You should call your healthcare provider if you experience:
. Extremely heavy periods.
. Severely painful cramps.
. Painful intercourse.
Source:
. https://my.clevelandclinic.org/health/diseases/14167-adenomyosis