Achilles tendon Rupture
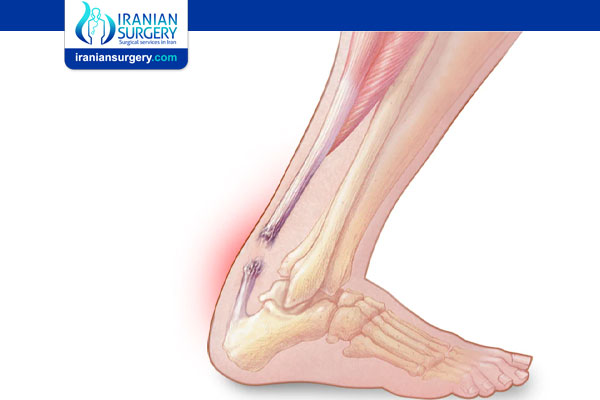
What is Achilles tendon rupture?
Achilles tendon rupture is an injury that affects the back of your lower leg. It mainly occurs in people playing recreational sports, but it can happen to anyone.
The Achilles tendon is a strong fibrous cord that connects the muscles in the back of your calf to your heel bone. If you overstretch your Achilles tendon, it can tear (rupture) completely or just partially.
If your Achilles tendon ruptures, you might hear a pop, followed by an immediate sharp pain in the back of your ankle and lower leg that is likely to affect your ability to walk properly. Surgery is often performed to repair the rupture. For many people, however, nonsurgical treatment works just as well.
Before Achilles tendon rupture treatment
Symptoms
Although it's possible to have no signs or symptoms with an Achilles tendon rupture, most people have:
. The feeling of having been kicked in the calf
. Pain, possibly severe, and swelling near the heel
. An inability to bend the foot downward or "push off" the injured leg when walking
. An inability to stand on the toes on the injured leg
. A popping or snapping sound when the injury occurs
Read more about : Achilles tendon Repair Surgery Recovery
When to see your doctor
Seek medical advice immediately if you hear a pop in your heel, especially if you can't walk properly afterward.
Causes
Your Achilles tendon helps you point your foot downward, rise on your toes and push off your foot as you walk. You rely on it virtually every time you walk and move your foot.
Rupture usually occurs in the section of the tendon situated within 2 1/2 inches (about 6 centimeters) of the point where it attaches to the heel bone. This section might be prone to rupture because blood flow is poor, which also can impair its ability to heal.
Ruptures often are caused by a sudden increase in the stress on your Achilles tendon. Common examples include:
. Increasing the intensity of sports participation, especially in sports that involve jumping.
. Falling from a height
. Stepping into a hole
Risk factors
Factors that may increase your risk of Achilles tendon rupture include:
. Age. The peak age for Achilles tendon rupture is 30 to 40.
. Sex. Achilles tendon rupture is up to five times more likely to occur in men than in women.
. Recreational sports. Achilles tendon injuries occur more often during sports that involve running, jumping, and sudden starts and stops — such as soccer, basketball and tennis.
. Steroid injections. Doctors sometimes inject steroids into an ankle joint to reduce pain and inflammation. However, this medication can weaken nearby tendons and has been associated with Achilles tendon ruptures.
. Certain antibiotics. Fluoroquinolone antibiotics, such as ciprofloxacin (Cipro) or levofloxacin (Levaquin), increase the risk of Achilles tendon rupture.
. Obesity. Excess weight puts more strain on the tendon.
Prevention
To reduce your chance of developing Achilles tendon problems, follow these tips:
. Stretch and strengthen calf muscles. Stretch your calf until you feel a noticeable pull but not pain. Don't bounce during a stretch. Calf-strengthening exercises can also help the muscle and tendon absorb more force and prevent injury.
. Vary your exercises. Alternate high-impact sports, such as running, with low-impact sports, such as walking, biking or swimming. Avoid activities that place excessive stress on your Achilles tendons, such as hill running and jumping activities.
. Choose running surfaces carefully. Avoid or limit running on hard or slippery surfaces. Dress properly for cold-weather training, and wear well-fitting athletic shoes with proper cushioning in the heels.
. Increase training intensity slowly. Achilles tendon injuries commonly occur after an abrupt increase in training intensity. Increase the distance, duration and frequency of your training by no more than 10 percent weekly.
Read more about : Cycling after knee arthroscopy
Diagnosis
During the physical exam, your doctor will inspect your lower leg for tenderness and swelling. Your doctor might be able to feel a gap in your tendon if it has ruptured completely.
The doctor might ask you to kneel on a chair or lie on your stomach with your feet hanging over the end of the exam table. He or she might then squeeze your calf muscle to see if your foot will automatically flex. If it doesn't, you probably have ruptured your Achilles tendon.
If there's a question about the extent of your Achilles tendon injury — whether it's completely or only partially ruptured — your doctor might order an ultrasound or MRI scan. These painless procedures create images of the tissues of your body.
What are possible complications of an Achilles tendon rupture?
The complications of Achilles tendon rupture include tendon scarring and decreased range of motion, as well as muscle weakness.
Tendon re-rupture is a significant concern and can occur in up to 5% of surgically repaired patients and in some studies, up to 40% in conservatively treated patients.
Other complications related to surgery include skin sloughing, wound infection, nerve damage, and scarring.
During Achilles tendon rupture treatment
Treatment of Achilles tendon rupture
Achilles tendon rupture can be treated with either surgery or conservative (non-surgical) measures. Your doctor will assess your injury and discuss if surgery would be an option for you. Which treatment your doctor recommends will depend on several factors, including your age, your general health and how active you are.
You’ll usually need to wear a brace or cast on your leg to protect it from further injury while you wait for treatment. You may be asked not to put weight on the affected leg during this time. You may also be offered medicines to reduce your risk of developing deep vein thrombosis (DVT) while your leg is immobile.
Read more about : Knee Ligament Repair
Non-surgical treatment
Your doctor may be more likely to suggest conservative (non-surgical) treatment if you’re older, have other health problems or aren’t particularly active. This usually involves wearing casts or a brace to support your lower leg while the tendon heals. You may need to take over-the-counter painkillers while your tendon is healing.
Compared to surgery, non-surgical treatment has a smaller chance of complications. But there is a greater chance of having another rupture in the future.
. Casting
Casts are usually from your knee downwards and are put on with your foot in a fully bent downwards position. You may have to wear a cast for several weeks, although they may be changed to gradually move your foot into a more neutral position. You won’t be able to put weight on your leg and will need crutches to move around.
. Brace
A brace is a rigid type of boot with straps to adjust it. It usually fits from your knee downwards. Once the brace is on, it’s adjusted several times over a few weeks to lift your foot up. You can walk and put weight on your leg while wearing the brace, and you can also remove it to move your ankle joint.
Surgery
Your doctor may be more likely to suggest surgery if:
. You’re young and active
. You’re a competitive athlete
. You’ve had a delay in treating the rupture
. You keep rupturing your Achilles tendon
There are several different techniques for surgical repair of Achilles tendon. All involve bringing the torn ends of your tendon back together. You may have open surgery, which involves making a cut into your ankle to fix the tendon. Or you can have minimally invasive surgery, where your surgeon will reach the tendon through small holes.
Having surgery rather than non-surgical treatment means your tendon is less likely to rupture again. But with surgery there is a greater chance of complications, including infection of the wound and development of scar tissue. These risks may be lower with minimally invasive surgery. Your surgeon will explain the different options, so you can decide what’s best for you.
After your operation, you’ll need to wear a cast or an adjustable brace on your leg to help the tendon heal.
Rehabilitation
Whether you had surgery for your Achilles tendon or not, you’ll need a period of rehabilitation after your initial treatment. You should see a physiotherapist, who will guide you on exercises to increase the range of movement and strength in your ankle and lower leg. You’ll start with gentle exercises and build these up over time. You might have some exercises specifically designed to strengthen or stretch your calf muscles. Your physiotherapist may also advise you on what low-impact exercises, such as cycling, jogging or swimming, you can try.
After Achilles tendon rupture treatment
Recovery from Achilles tendon rupture
How long it takes to recover from an Achilles tendon rupture is similar whether you have surgery or not. You can expect to be back to normal activities, including low-impact sports, within four to six months, whichever treatment you have. But it can take longer to get back to high-impact sports, such as football, squash or tennis.
Most people can return to the type of activity that they did before their injury. But if you play sport at a professional level, you may find some limitations in what you can do. It might take a year or more to get back to your previous level of performance. Your physiotherapist or doctor will give you more advice specific to you.
You may need to take time off work to allow the tendon to heal. How long you need to take off will vary depending on a number of things. These include the type of treatment you’ve had, how mobile you were previously, what job you do and any restrictions at your workplace. Your doctor will be able to give you specific advice.
What is the prognosis of an Achilles tendon rupture?
When proper treatment and rehabilitation are undertaken, the prognosis is excellent. The majority of athletes can return to their previous exercise or sports. Those patients who undergo nonsurgical care have an increased risk of repeated rupture.
Sources:
. https://www.mayoclinic.org/diseases-conditions/achilles-tendon-rupture/symptoms-causes/syc-20353234
. https://www.bupa.co.uk/health-information/muscles-bones-joints/achilles-tendon-rupture
. https://www.medicinenet.com/achilles_tendon_rupture/article.htm

